 |
 |
 |
| |
Adverse pregnancy outcomes among HIV-positive women in the era of universal antiretroviral therapy (ART) remain elevated compared with HIV-negative women in Lesotho
|
| |
| |
Download the PDF here

Program abstract
Background: Prior to the ART era, adverse pregnancy outcomes were more common among HIV-positive than HIV-negative women. In the universal ART era, most HIV-positive pregnant women are receiving ART, many prior to pregnancy. There are conflicting data whether adverse pregnancy outcomes among HIV-positive women on ART in the current era of “test and treat” remain higher than among HIV-negative women.
Methods: Pregnancy outcomes data were collected from an ongoing prospective study (started 2016) evaluating a multidisciplinary “Integrated Management Team to Improve Maternal-Child Outcomes (IMPROVE)” intervention to improve maternal-child health and HIV service uptake/retention. HIV-positive and HIV-negative pregnant women at 12 facilities in Lesotho were enrolled at their first antenatal visit (ANC) in a cluster randomized evaluation of the IMPROVE intervention vs standard of care, with prospective follow-up through 12-24 months postpartum. We used combined data from both randomized groups on delivery outcomes. Chi-square tests were used to test for statistical significance of differences between outcomes of HIV-positive vs HIV-negative women.
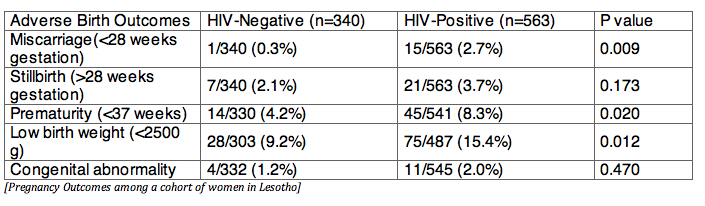
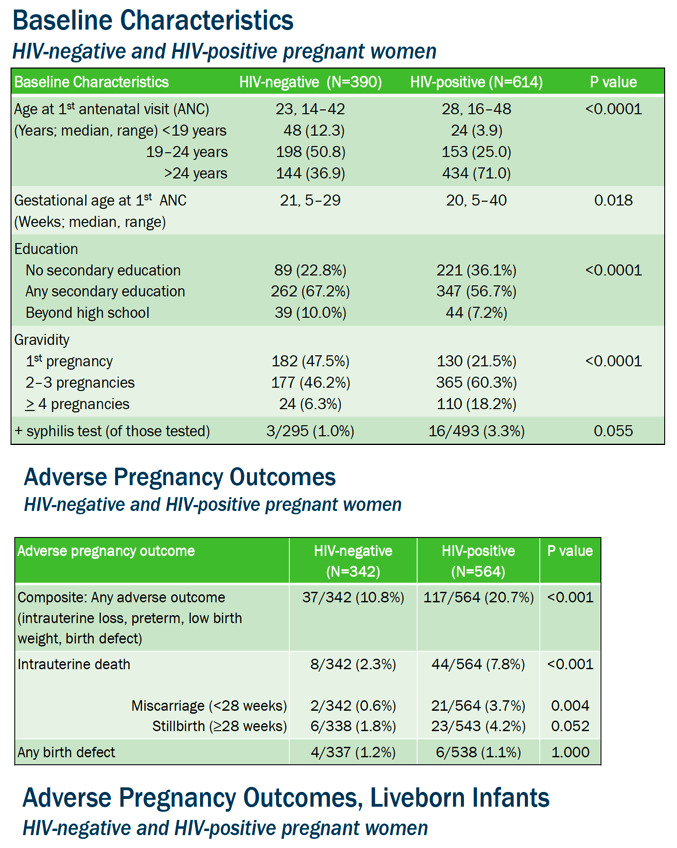
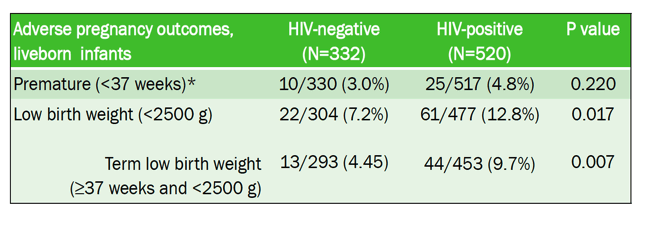
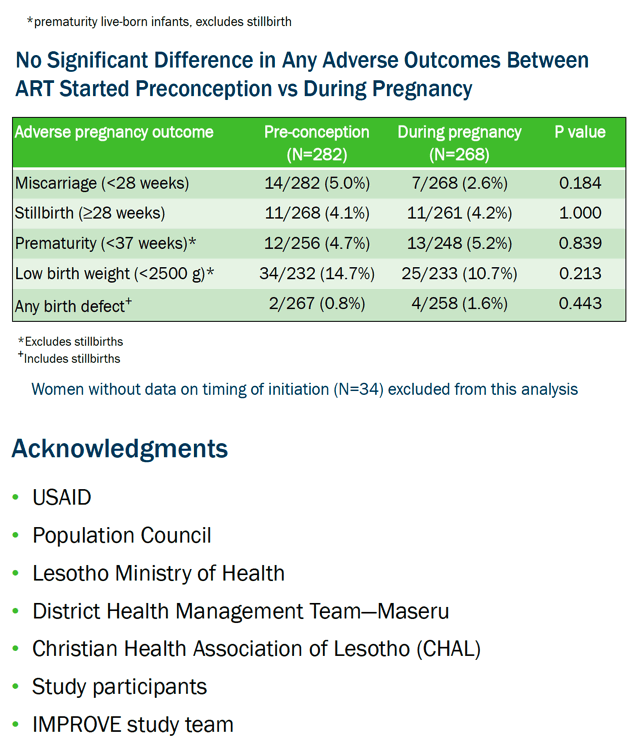
Results: 1,002 women were enrolled, with delivery data captured for 903 women to date (563 HIV-positive and 340 HIV-negative). Mean gestational age at enrollment was 20 weeks regardless of HIV status. Among HIV-positive women, 74% knew their HIV status prior to their first ANC visit, with 92% already receiving ART (88% TDF+3TC+EFV); among women first diagnosed with HIV during pregnancy, 95% started on ART (98% TDF+3TC+EFV). HIV-positive women were more likely than HIV-negative women to experience a miscarriage or have a premature or low birthweight infant (mean 2.8kg vs 3.0kg, respectively) (Table). Stillbirths and congenital anomalies were non-significantly higher in HIV-positive than HIV-negative women (3.7% vs 2.1% and 2.0% vs 1.2%, respectively). Among HIV-positive women, timing of ART initiation was not associated with any of the measured outcomes.
Conclusions: Despite nearly universal ART, with most women on ART before pregnancy, adverse birth outcomes remained elevated among HIV-positive compared to HIV-negative women.




|
| |
|
 |
 |
|
|