 |
 |
 |
| |
Smoking and High HIV Viremia Damage Mitochondrial DNA and May Accelerate mtDNA Aging
|
| |
| |
IAS 2019
Adam S. Ziada1,2, Meng Ying Lu1,2, Jarek Ignas-Menzies3, Sara Saberi1,2, Anthony Y. Y. Hsieh1,2, Beheroze Sattha1,2, P. Richard Harrigan4, Steve Kalloger1, Hélène C.F. Côté1,2,5 and the CIHR team grant on Cellular Aging and HIV Comorbidities in Women and Children (CARMA)
1Department of Pathology & Laboratory Medicine, UBC; Vancouver, BC 2Centre for Blood Research, UBC; Vancouver, BC 3Department of Mechanical Engineering, University of British Columbia, Vancouver, BC, Canada;
4 Department of Medicine, University of British Columbia, Vancouver, BC, Canada, 5Women’s Health Research Institute, Vancouver, BC, Canada
program abstract
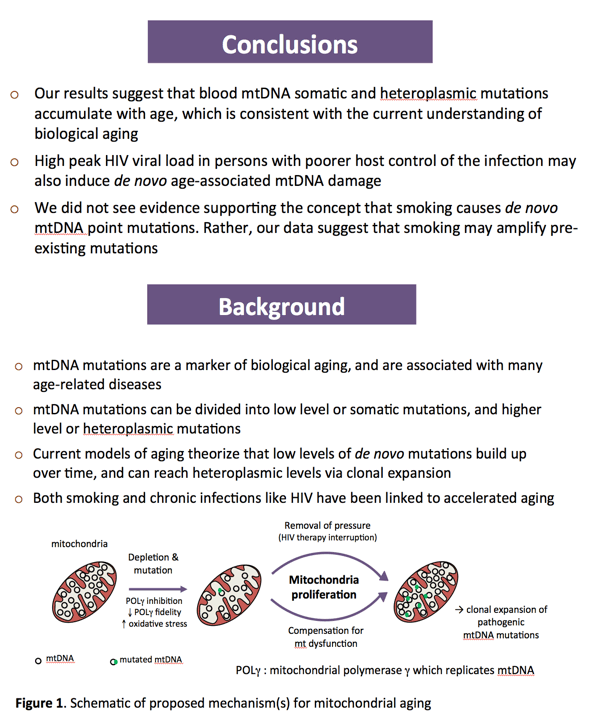
Background: People living with HIV experience accelerated aging. The accumulation of somatic mitochondrial DNA (mtDNA) point mutations is believed to be a marker of biological aging, and has been implicated in several age-associated diseases that manifest prematurely in HIV+ individuals. Current theories of aging describe both de novo mutations, and the clonal expansion of pre-existing mutations, as potential mechanisms for the accumulation of mtDNA mutations. In this study, we hypothesized that somatic mtDNA substitutions (frequency ≤2%), which may represent de novo mutations, and heteroplasmic mtDNA substitutions (frequency >2%), that may result from clonal expansion, would increase with older age, tobacco smoking and HIV infection.
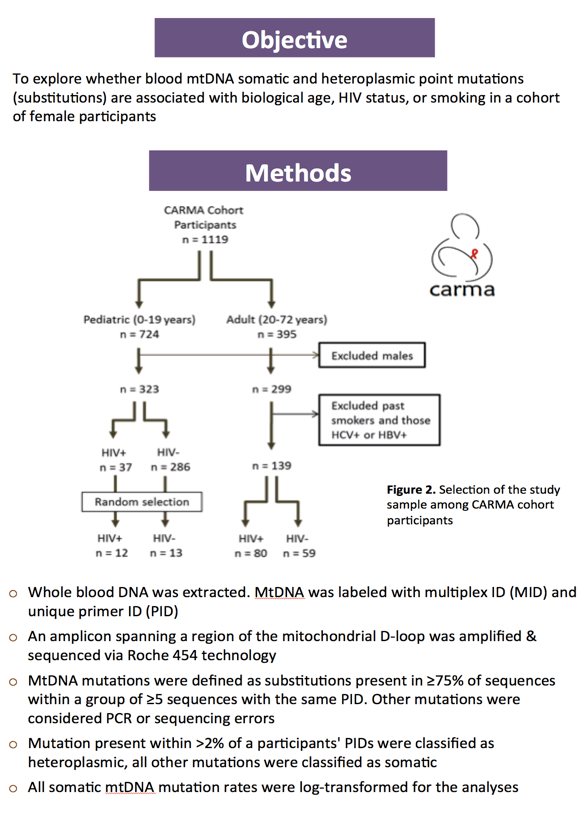
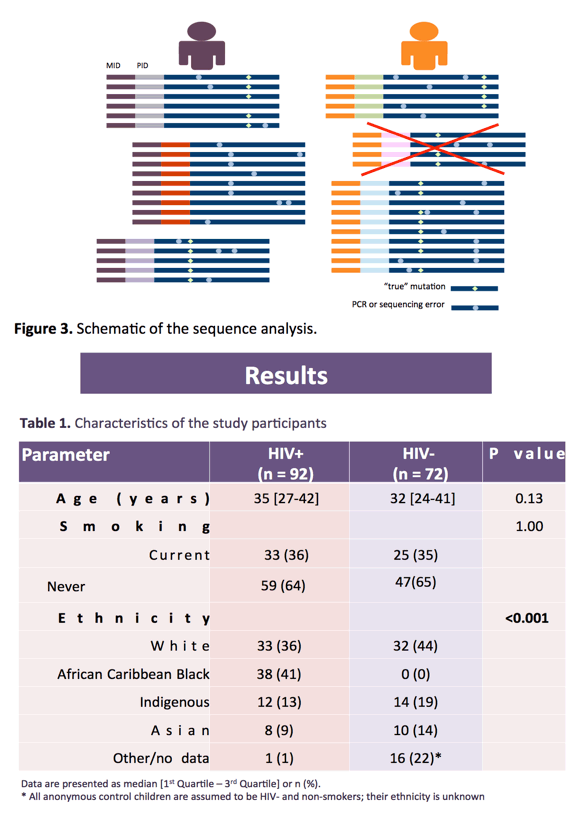
Methods: Participants in this cross-sectional study were HIV+ (n=92) and HIV-negative (n=72) girls and women aged 1-62 years, enrolled in the CARMA cohort, not infected with hepatitis C or B, and either current or never smokers. Whole blood mtDNA substitution mutation rates/10Kb were quantified via next generation sequencing with primer IDs. Univariate associations between our mtDNA measures (occurrence of heteroplasmy and somatic mtDNA mutation rates) and age, smoking, or HIV were examined, along with possible confounders. Variables important univariately (p< 0.1) were considered for inclusion in multivariable models. Age, smoking status and HIV status were included in all models, as per our a priori study design.
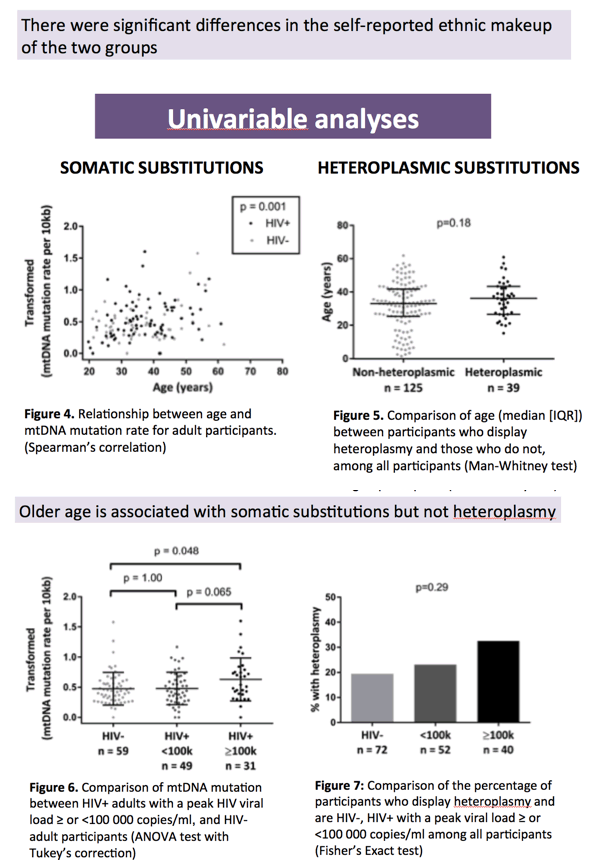
Results: In a model of adult participants (n=139) that included age, smoking status, and HIV status, being older (p=0.003) and having a peak HIV viremia ≥100 000 copies/ml (vs. HIV-) (p=0.045) were independently associated with higher somatic mtDNA mutation frequency. MtDNA heteroplasmy among all participants (n=164), was associated with older age (p=0.006) and being a current smoker (p< 0.001) but not with living with HIV. An interaction was observed between age and smoking whereby heteroplasmy increased in non-smokers (p=0.004) but decreased in current smokers (p=0.025) with age.
Conclusions: Exposure to high HIV viremia may contribute to increased mtDNA mutations and accelerated aging in some people living with HIV. In contrast, smoking seemed to promote the clonal expansion of mutations rather than increase de novo mutations. This too may be consistent with the knowledge that smoking promotes age-related diseases.

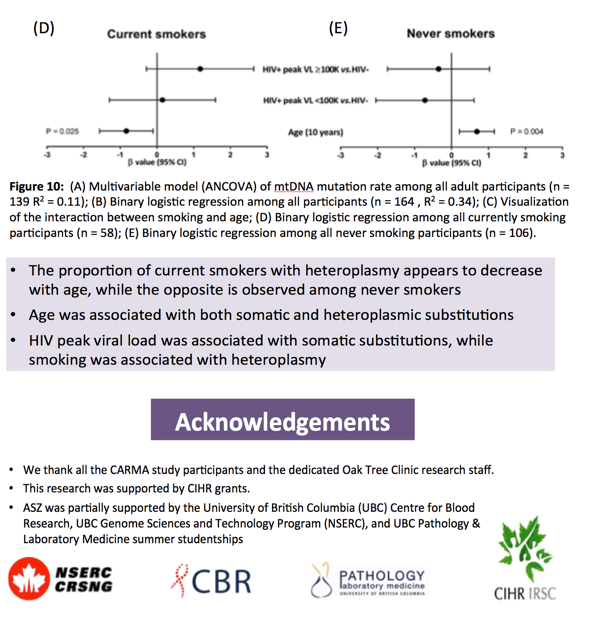
|
| |
|
 |
 |
|
|