 |
 |
 |
| |
Simulated Driving Worse in Pro Drivers With Than Without HIV - "Cognitive functioning and driving ability in HIV-infected professional drivers"
|
| |
| |
Download the PDF here
10th IAS Conference on HIV Science (IAS 2019), July 21-24, 2019, Mexico City
Mark Mascolini
A pilot study of 40 professional drivers with or without HIV infection found significantly worse video simulator driving in the HIV group [1]. Drivers with HIV also had significantly worse cognitive test results. University of Cape Town researchers stressed that cognitive impairment--but not HIV itself--predicted risky simulated driving.
Prior research reported poor driving performance in HIV-positive lay drivers with neurocognitive impairment [2]. But the impact of cognitive function on driving among professional drivers remained unknown until this study. Because cognitive impairment persists in people responding to antiretroviral therapy, and because more people with HIV now work, better understanding of how cognitive function affects work performance seems prudent.
To address these issues, University of Cape Town researchers and collaborators at other centers conducted a cross-sectional pilot study of 20 HIV-positive and 20 HIV-negative male professional drivers in southern Africa. They matched positive and negative men by education and age, which averaged 39.2 years. Study participants completed a comprehensive neuropsychological battery including tests in 7 domains. Researchers determined a global deficit score by calculating deficit scores across all neuropsychological tests. The driving simulator tested participants for standard deviation of lateral position on the road, speed deviation, crashes, and response latency and accuracy on divided-attention stimuli.
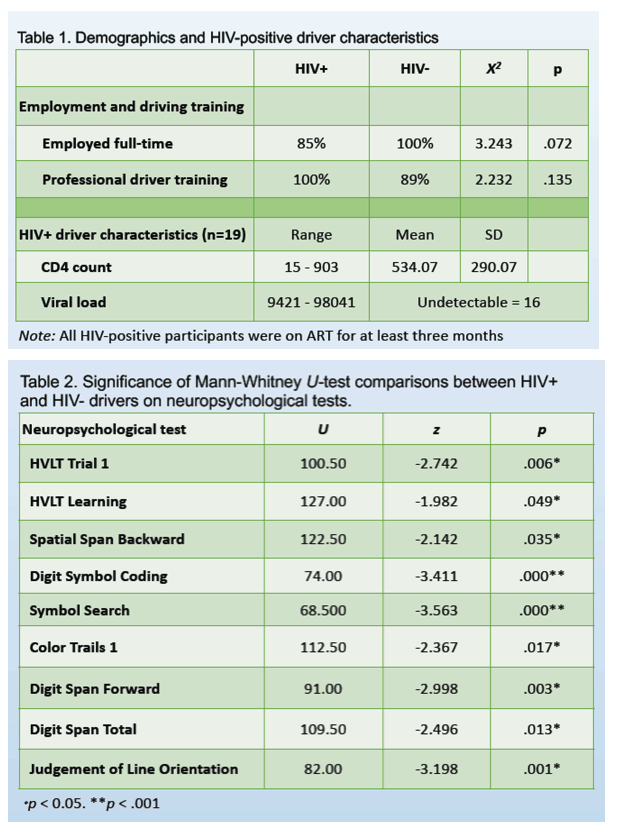
All HIV-negative drivers had a full-time job, compared with 85% of HIV-positive drivers, a difference that approached statistical significance (P = 0.072). All HIV-positive drivers and 89% of HIV-negative drivers had professional driver training, a nonsignificant difference (P = 0.135). CD4 count averaged 534 and ranged from 15 to 903 in the HIV group. Sixteen of 19 HIV-positive drivers had an undetectable viral load.
Compared with HIV-negative drivers, those with HIV performed significantly worse on neuropsychological tests of (1) verbal learning and verbal memory/delayed recall, (2) processing speed, (3) attention/working memory, and (4) visuospatial functioning. Three HIV-negative drivers (15%) and 12 HIV-positive drivers (60%) had neurocognitive impairment determined by global deficit score. On the simulated driving test, drivers with HIV were more likely to exceed the speed limit (P = 0.024), not maintain lane position (P = 0.020), and have more collisions (P = 0.044).
Worse results on a processing speed test and an attention/working memory test correlated positively with increased speeding. Worse performance on a processing speed testing strongly correlated positively with driving out of lane and collisions.
The researchers concluded that their small study found worse cognitive function and worse simulated driving in professional drivers with than without HIV. And by several measures, impaired cognitive function predicted poor driving. But HIV itself did not predict worse driving. The investigators believe their preliminary results suggest that professional drivers with HIV may improve their driving by participating in cognitive rehabilitation or other programs that can improve cognition (such as those aiming to bolster antiretroviral adherence).
In the earlier study of HIV-positive lay drivers in the United States [2], those with neurocognitive impairment had 5-fold higher odds of failing a driving simulation test and 6-fold higher odds of accidents in a simulation of city driving.
References
1. Gouse H, Robbins R, Masson CJ, et al Cognitive functioning and driving ability in HIV-infected professional drivers. 10th IAS Conference on HIV Science (IAS 2019), July 21-24, 2019, Mexico City. Abstract TUPED748.
2. Marcotte TD, Heaton RK, Wolfson T, et al. The impact of HIV-related neuropsychological dysfunction on driving behavior. The HNRC Group. J Int Neuropsychol Soc. 1999;5:579-592

Gouse H1., Robbins, R2., Masson,C.J1., Henry, M3., Thomas, K.F.G4., Munsami, A1., London, L5., Kew, G5., Joska, J.A1., Marcotte, T.D6.
1HIV Mental Health Research Unit, Department of Psychiatry and Mental Health, University of Cape Town (UCT); 2HIV Center for Clinical and Behavioral Studies, New York State Psychiatric Institute and Columbia University Medical Center; 3Centre for Higher Education Development, UCT; 4Depeartment of Psychology, UCT; 5School of Public Health and Family Medicine, UCT; 6HIV Neurobehavioral Centre, University of San Diego.




|
| |
|
 |
 |
|
|