 |
 |
 |
| |
Polypharmacy in Nearly All of 65+ HIV Group Tied to Inappropriate Prescribing
|
| |
| |
'The New Mexico team called for "targeted interventions" to limit polypharmacy and inappropriate prescribing in older people with HIV infection….Examples of inappropriate prescribing include: prescriptions that have greater risk than potential benefit'
Nearly everyone in a 65-or-older US HIV group met study criteria for polypharmacy, defined as using 5 or more medications [1]. Two thirds of the New Mexico study group had 1 or more adverse outcomes, and polypharmacy correlated with greater risk of inappropriate prescribing by three measures.
University of Mexico researchers who conducted this study noted that the number of 65-or-older people with HIV jumped more than 50% since 2011. Older people run a greater risk of polypharmacy because of accumulating comorbidities, age-related physiological changes, and reliance on multiple providers. Older individuals taking more drugs also risk more drug-drug interactions and inappropriate prescribing, such as duplicated therapy, inappropriate dosing frequency, and prescribing agents that may lead to significant drug-drug interactions.
To assess the frequency of polypharmacy in an older group with HIV, and to explore its potential consequences, the researchers conducted a retrospective analysis of HIV-positive people at least 65 years old when seen at a University of New Mexico clinic from January 2015 through August 2018. Reviewing patient medication lists, the investigators defined polypharmacy as taking 5 or more medications; they defined inappropriate prescribing by 2012 Beers criteria, 2011 STOPP criteria, and START criteria. To identify potential HIV drug-drug interactions, they used the University of Liverpool HIV drug interactions site [2].
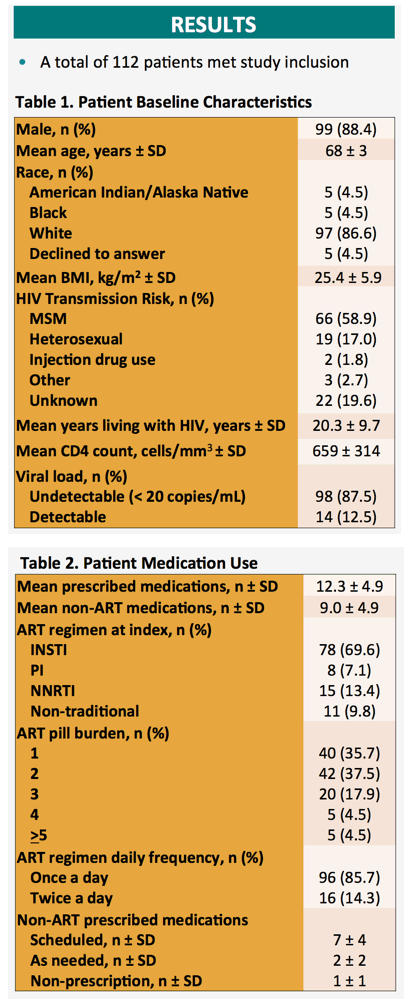
Of the 112 study participants, 99 (88%) were men, 97 (87%) white, and 66 (59%) men who have sex with men. Age averaged 68 years, time with HIV averaged 20.3 years, and 98 people (87.5%) had a viral load below 20 copies. Participants were prescribed an average 12.3 medications, including 9.0 non-HIV medications. Most people, 73%, took only 1 or 2 antiretroviral pills, and 86% took a once-daily antiretroviral regimen.
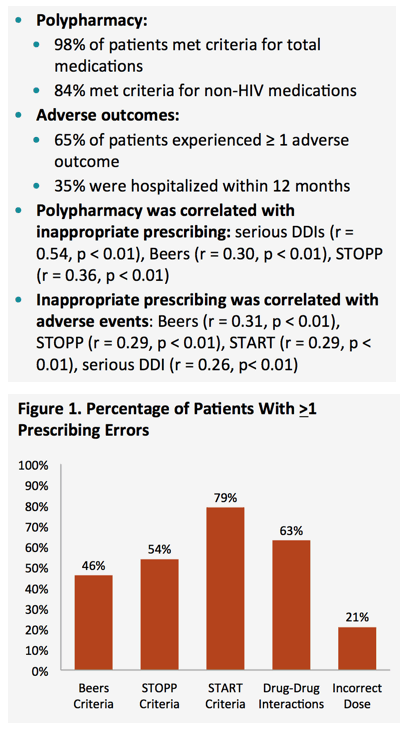
Almost all participants, 98%, met criteria for polypharmacy. When the researchers considered only non-HIV medications, 84% met polypharmacy criteria. Two thirds of participants, 65%, had 1 or more adverse outcomes. Polypharmacy correlated with greater risk of inappropriate prescribing judged by serious drug-drug interactions (r = 0.54, P < 0.01), by Beers criteria (r = 0.30, P < 0.01) and by STOPP criteria (r = 0.36, P < 0.01). Inappropriate prescribing correlated with adverse events by Beers criteria (r = 0.31, P < 0.01), STOPP criteria (r = 0.29, P < 0.01), START criteria (r = 0.29, P < 0.01), and serious drug-drug interactions (r = 0.26, P < 0.01)
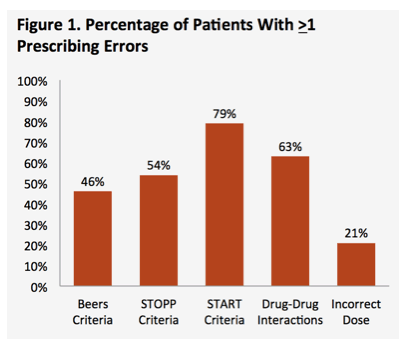
More than half of participants had 1 or more prescribing errors by START criteria (79%), drug-drug interaction criteria (63%), or STOPP criteria (54%). The most frequent potentially inappropriate prescribing errors were (1) pneumococcal vaccine after age 65 (48% by START criteria), (2) NSAID for chronic use (35% by Beers criteria), and (3) any drug without an evidence-based clinical indication (34% by STOPP criteria).
The New Mexico investigators concluded that their study "highlights the pervasiveness of polypharmacy in the aging [HIV] population, which was driven by non-HIV co-medications." They noted that links between inappropriate prescribing and clinical outcomes like hospital admission rest on simple Pearson correlations and need further study. The New Mexico team called for "targeted interventions" to limit polypharmacy and inappropriate prescribing in older people with HIV infection.
References
1. Cabanilla MG, Marzolini C, Conklin JE, et al. Risk of polypharmacy and inappropriate prescribing in persons living with HIV ≥ 65 years of age. 10th IAS Conference on HIV Science (IAS 2019), July 21-24, 2019, Mexico City. Abstract WEPEB314.
2. University of Liverpool. HIV drug interactions. https://www.hiv-druginteractions.org/checker





|
| |
|
 |
 |
|
|