 |
 |
 |
| |
HCV REINFECTION AFTER DAA TREATMENT
AMONG PEOPLE LIVING WITH HIV IN SAN DIEGO
|
| |
| |
CROI 2020
Reported by Jules Levin
Lucas Hill1, Natasha Martin1, Sonia Jain1, Francesca Torriani1, Xiaoying Sun1, Huifang Qin1, Craig Ballard1, W. C. Mathews1, Edward R. Cachay1
1University of California San Diego, La Jolla, CA, USA
Program Abstract
Previously, we reported the HCV reinfection rate in San Diego from 2000 to 2014 among HIV-infected men who have sex with men (MSM) during the interferon era was 2.89/100 PYFU. Herein, we report the HCV re-infection rates in all groups of people living with HIV (PLWH) treated with interferon-free direct-acting antivirals (DAA) in San Diego, California
Retrospective cohort analysis of adult PLWH treated with DAA at the University of California, San Diego between 2014 and April 2019. PLWH with documented sustained virologic response (SVR), and at least one subsequent HCV RNA measurement before September 2019 were included. HCV re-infection was defined as new HCV viremia after documented SVR. Follow up time was calculated from the date of SVR documentation until the first subsequent positive HCV RNA or the last negative HCV RNA. Clinical onset of re-infection was defined as the date of the first noted HCV RNA. Person-time incidence rates [95% C.I.] per 100 years-at-risk (PYFU) were estimated using the Poisson distribution
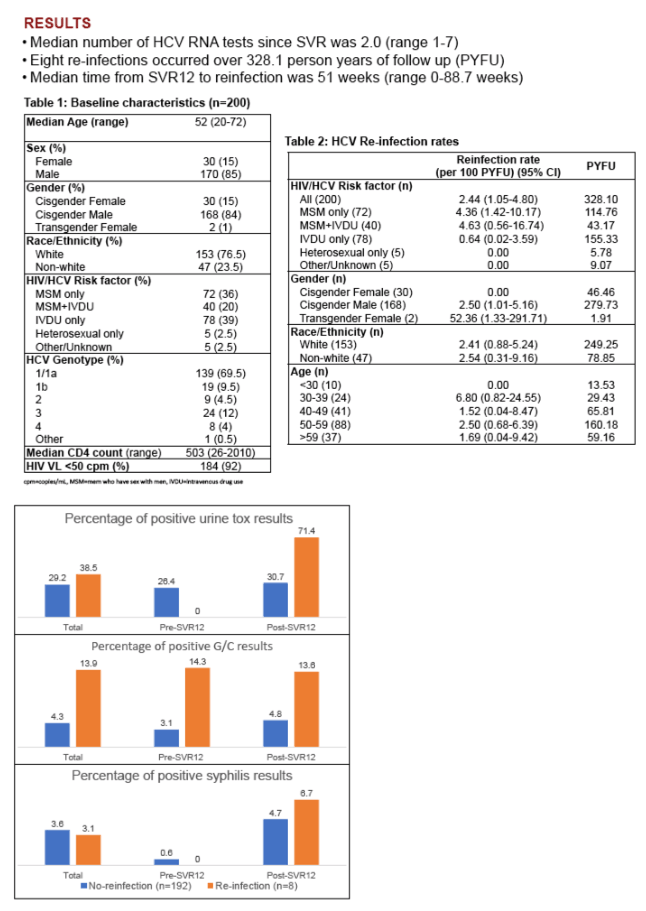
There were 204 PLWH with documented SVR. Their median age was 52 years (95% CI: 50-53.4), 83.3% were male, and 21.6% were non-white. HCV genotypes distribution were 1a in 139 (68.1%), 1b in 20 (9.8%), 3 in 27 (13.2%) and other in 18 (8.8%). The median CD4 count in cells/uL was 503 (95% CI: 464-562) and 188 (92.2%) had undetectable HIV viral load. HCV risk factors were MSM in 54.9%, of which 40.2% also had a history of intravenous drug use (IVDU), and IVDU as the only risk factor in 39.2%. Six men acquired a new HCV infection over 321.7 PYFU. The HCV reinfection incidence rate overall was 1.87 and in MSM non-IVDU 3.54 per 100 PYFU. The median time from end-of-DAA-treatment to reinfection was 54 weeks (range 7-95.4 weeks). Of the six reinfected patients, three had a change in genotype and one had cirrhosis with documented SVR a year after finishing DAA before his reinfection. The table shows reinfection rates by HCV risk category, gender, ethnicity, and age. There were no reinfections among females. Five reinfected patients were-treated successfully, with one pending retreatment with DAA
The overall reinfection rate in San Diego among PLWH in the DAA era is low, and is highest among MSM but comparable to previously observed in the interferon era. This result may help guide future interventions to prevent HCV reinfection in PLWH at risk in San Diego


|
| |
|
 |
 |
|
|