 |
 |
 |
| |
HEPATITIS C VIRUS INFECTION AND COINFECTION WITH HIV AMONG PWID IN 10 US CITIES
|
| |
| |
CROI 2020
Reported by Jules Levin
Johanna Chapin-Bardales1, Alice Asher1, Dita Broz1, Eyasu Teshale1, Tonya Hayden1, Carlos Blanco2, Senad Handanagic1, Cyprian Wejnert1
1CDC, Atlanta, GA, USA,2National Institute on Drug Abuse, Rockville, MD, USA
Abstract Body:
Understanding the burden of acute and chronic hepatitis C virus (HCV) infection and HIV/HCV co-infection among persons who inject drugs (PWID) is important for informing HIV and HCV elimination efforts. We measured HCV infection and HIV/HCV co-infection among PWID in 10 U.S. cities.
In 2018 National HIV Behavioral Surveillance, PWID were recruited using respondent-driven sampling and offered a behavioral survey, HIV testing, and HCV antibody and RNA testing in Chicago, Dallas, Houston, Los Angeles, Miami, New York City, Philadelphia, San Francisco, San Juan, and Washington DC. We examined prevalence of acute (anti-HCV non-reactive/RNA detected) and chronic (anti-HCV reactive/RNA detected) HCV infection and HIV/HCV co-infection. We obtained adjusted prevalence ratios (aPRs) and 95% confidence intervals (CIs) to assess characteristics associated with current HCV infection (RNA detected vs. not detected) and HIV/HCV co-infection (vs. no HIV/HCV co-infection).
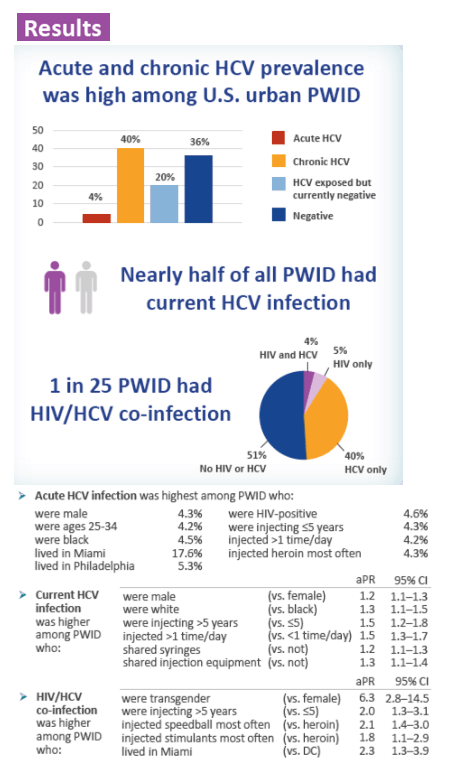
Overall, 62.4% (3239/5,190) had a reactive anti-HCV result, 44.2% (1678/3795) had HCV RNA detected, and 4.0% (153/3,779) had HIV/HCV co-infection. Of those with both antibody and RNA test results, 3.9% (149/3795) had acute and 40.3% (1529/3795) had chronic HCV infection. Acute infection was highest among PWID who were male (4.3%), ages 25-34 (4.2%), black (4.5%), HIV-positive (4.6%), injecting 5 years (4.3%), injected >1 time/day (4.2%), injected heroin most often (4.3%), and were from Miami (17.6%) or Philadelphia (5.3%). Current HCV infection was higher among PWID who were male (aPR 1.2, 95% CI 1.1-1.3), white (aPR 1.3, 95% CI 1.1-1.5), injecting >5 years (aPR 1.5, 95% CI 1.2-1.8), injected >1 time/day (aPR 1.5, 95% CI 1.3-1.7), and shared syringes (aPR 1.2, 95% CI 1.1-1.3) or injection equipment (aPR 1.3, 95% CI 1.1-1.4) in the past year. HIV/HCV co-infection was higher among participants who were transgender (aPR 6.3, 95% CI 2.8-14.5), injecting >5 years (aPR 2.1, 95% CI 1.3-3.1), injected speedball (heroin and cocaine injected together) (aPR 2.1, 95% CI 1.4-3.0) or stimulants (aPR 1.8, 95% CI 1.1-2.9) most often (vs. heroin), and were from Miami (aPR 2.3, 95% CI 1.3-3.9).
Acute and chronic HCV prevalence was high among a sample of U.S. urban PWID. Nearly one in two PWID had current HCV infection and one in 25 had HIV/HCV co-infection in our sample. HCV and HIV elimination efforts should focus on providing treatment and reducing risk behaviors among PWID to prevent further transmission.


|
| |
|
 |
 |
|
|