 |
 |
 |
| |
Doubled Risk of non-HIV Mortality in US People at Risk for HIV
|
| |
| |
CROI 2020, March 8-11, 2020, Boston
Mark Mascolini
Compared with low-risk heterosexuals, HIV-negative men who have sex with men (MSM) and HIV-negative people who inject drugs ran a doubled risk of non-HIV mortality in a 40,000-person US analysis [1]. Adults at high risk for HIV through heterosexual sex ran a 60% higher chance of non-HIV death than their low-risk heterosexual counterparts.
People who put themselves at risk for HIV infection by injecting drugs or having unsafe gay or straight sex often have other lifestyle traits that boost chances of sickness and death, like smoking, using dangerous drugs, and getting sexually transmitted infections. Because little is known about non-HIV death risk in this diverse HIV-negative group, researchers from Massachusetts General Hospital and other centers set out to estimate excess mortality according to HIV risk factor: MSM sex, risky heterosexual sex, and drug injection.
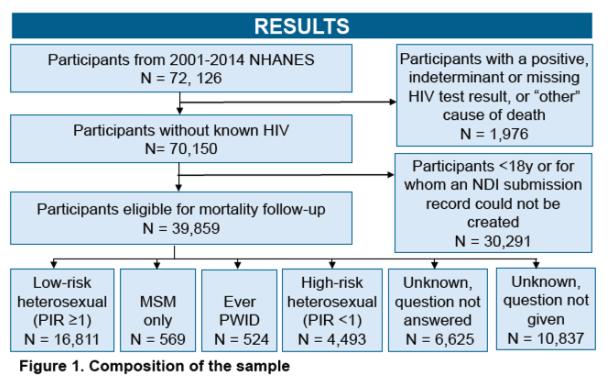
The analysis involved people in the 2001-2014 cycles of the National Health and Nutrition Examination Survey (NHANES) and its Linked Mortality File, updated with input from the National Death Index through December 2015. The study excluded people under 18 years old, those with a positive, indeterminate, or missing HIV test result, and those with an "other" cause of death. Participants self-reported sexual orientation and drug use. The researchers classified heterosexuals as high-risk or low-risk according to socioeconomic status and poverty income ratio.
The investigators identified 39,859 NHANES participants eligible for mortality follow-up, including 16,811 low-risk heterosexuals, 4493 high-risk heterosexuals, 569 MSM only, and 524 people who ever injected drugs. The remaining people were classified as "unknown, question not answered" (6625 people) or "unknown, question not given" (10,837 people).
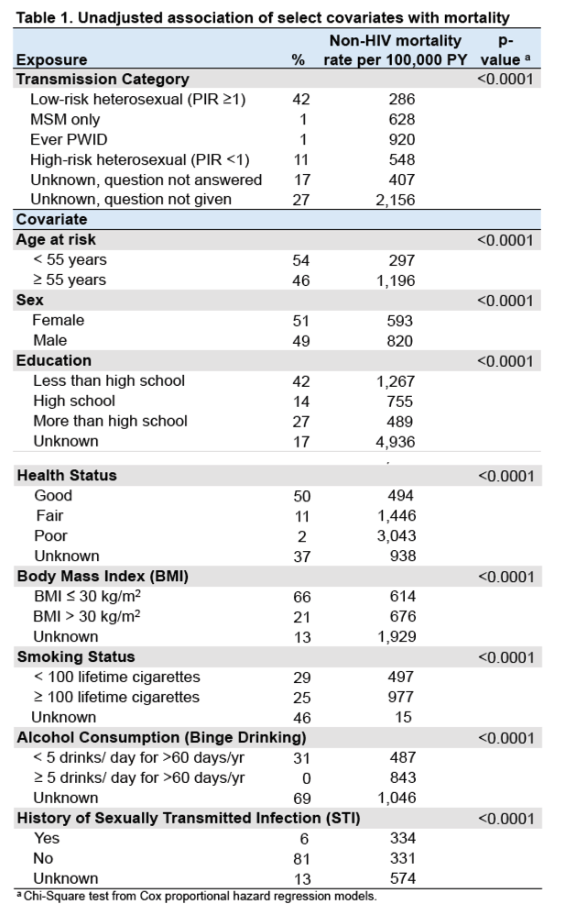
Among the four major just-described HIV risk groups, low-risk heterosexuals had the lowest non-HIV mortality (286 deaths per 100,000 person-years), followed by high-risk heterosexuals (548 per 100,000), MSM only (628 per 100,000), and people who ever injected drugs (920 per 100,000) (P < 0.0001 across groups).
Men had a significantly higher non-HIV death rate than women (820 versus 593 per 100,000, P < 0.0001). Less educated people had higher non-HIV mortality than more educated people (less than high school, 1267 per 100,000; high school, 755 per 100,000; more than high school, 489 per 100,000, P < 0.0001). This analysis also confirmed the health risks of other well-known factors, such as overweight or obesity, 100 or more lifetime cigarettes, 5 or more drinks a day for more than 60 days a year, and a history of sexually transmitted infections.
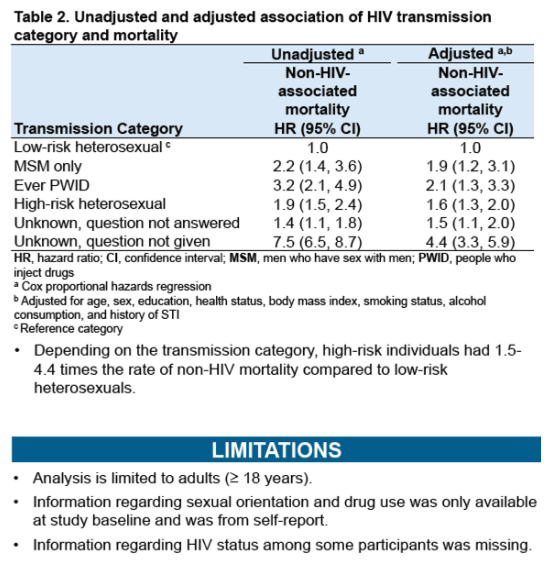
Cox proportional hazards regression adjusted for the above factors plus age and health status determined that the three groups at risk for HIV (but still HIV-negative) all had an independently higher risk of non-HIV death than low-risk heterosexuals, at the following adjusted hazard ratios (aHR) and 95% confidence intervals (CI):
-- MSM only: aHR 1.9, 95% CI 1.2 to 3.1
-- Ever injected drugs: aHR 2.1, 95% CI 1.3 to 3.3
-- High-risk heterosexual: aHR 1.6, 95% CI 1.3 to 3.0
People who did not answer or were not asked questions about HIV risk also had independently higher risks of death than the low-risk heterosexuals.
The findings underline the substantial risk of death among HIV-negative people who also place themselves at risk for HIV infection. Some of the heightened mortality in people with HIV certainly carries over from their pre-HIV lifestyle choices and perhaps socioeconomic factors reflected in educational attainment.
Reference
1. Shebl FM, Foote JH, Reddy KP, et al. Increased mortality among people at high risk for HIV in the United States. Conference on Retroviruses and Opportunistic Infections (CROI). March 8-11, 2020. Boston. Abstract 874.

Fatma M. Shebl,1,2Julia H. Foote,1Krishna P. Reddy,1,2Yiqi Qian,1Kenneth A. Freedberg,1,2,3Rochelle P. Walensky,1,2,3 Emily P. Hyle1,2,3
1 Massachusetts General Hospital, Boston, MA; 2 Harvard Medical School, Boston, MA; 3 Harvard University Center for AIDS Research, Cambridge, MA

|
| |
|
 |
 |
|
|