 |
 |
 |
| |
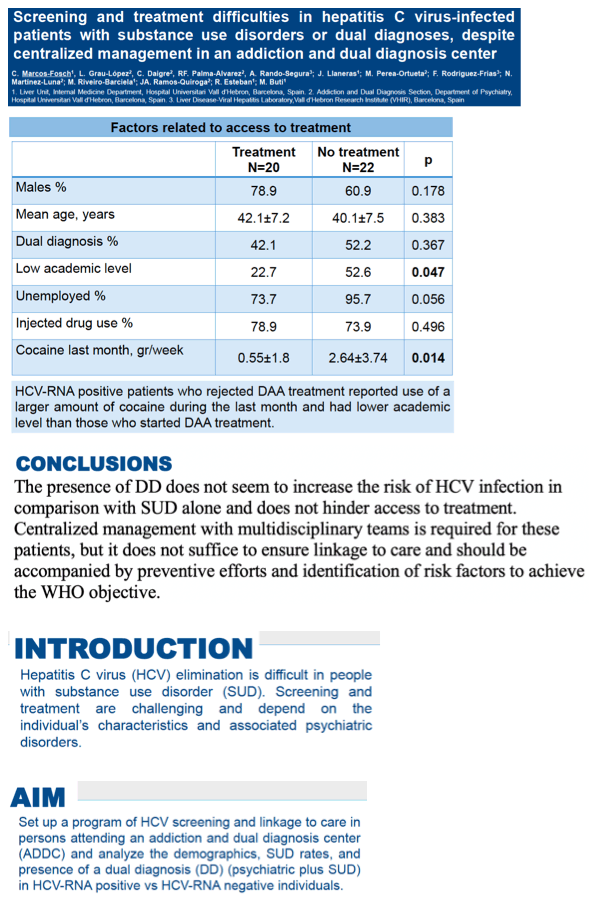
Screening and treatment difficulties of hepatitis C virus infected patients with substance use disorders or dual pathology, despite centralized management in an addiction and dual diagnosis center
|
| |
| |
EASL: Efficacy of Sofosbuvir/Velpatasvir (S/V): Impact of Treatment Adherence - (08/27/20)
EASL: Global real-world evidence of sofosbuvir/velpatasvir(SOF/VEL) as a highly effective treatment and elimination tool in underserved patient populations experiencing mental health disorders, incarceration or homelessness - (08/27/20)
EASL: Real-World Clinical Practice Outcomes in Hepatitis C-Infected Patients With Psychiatric and Substance Use Disorders Treated With Glecaprevir/Pibrentasvir for 8 or 12 Weeks: A Pooled Analysis Across 9 Countries - (08/27/20)
EASL HCV in the Australian primary care setting: Real-world effectiveness of 12 weeks of sofosbuvir/velpatasvirfor the treatment of chronic hepatitis C - (08/27/20)
EASL: Directly observed therapy for hepatitis C with sofosbuvir/velpatasvir alongside opioid substitution as a tailored microelimination strategy in PWIDs with a high risk of nonadherence - real-world data from Vienna, Austria - (08/27/20)
EASL: Barriers to Hepatitis C Virus Elimination in Germany: Why Aren't Diagnosed Patients Initiating Therapy? - (08/27/20)
--------------------------
In HCV/Substance Use Initiative, Fewer Than Half Offered DAAs Start
EASL 2020, Digital International Liver Congress, August 27-29, 2020.
Mark Mascolini
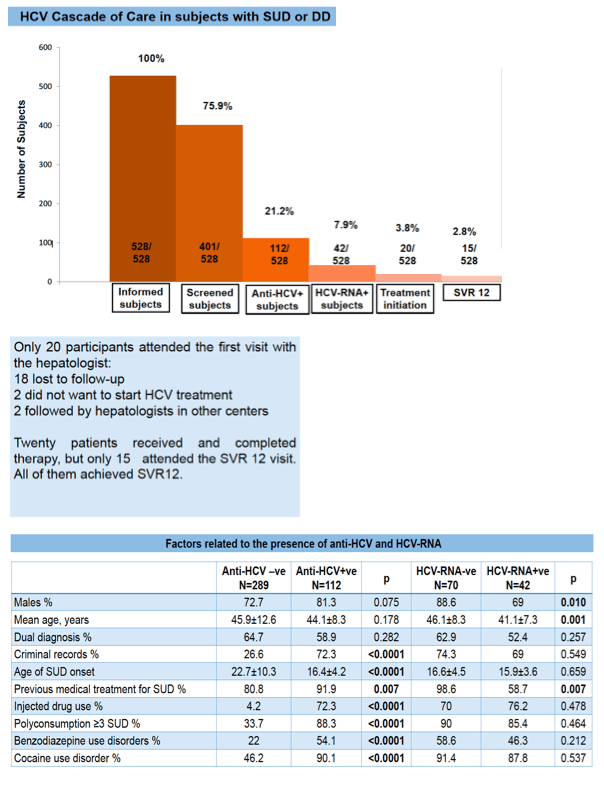
A Barcelona program to screen people with substance use disorder for HCV and link them to care had mixed results in its first 8 months [1]. Among the 42 people who tested positive for HCV RNA (of 528 people invited to join the program), only 20 (48%) started treatment and only 15 (36%) came back to be checked for sustained virologic response (SVR). Among the 528 invited to start the program, 127 (24%) declined.
Clinical researchers at Barcelona's Hospital Universitari Vall d'Hebron began a program for HCV screening and linkage to care at an addiction center caring for people with substance use disorder (SUD), including a dual diagnosis of psychiatric illness plus SUD. They aimed to integrate HCV care in the management of people with SUD or a dual diagnosis, including screening, diagnosis, and treatment with DAAs within the first 6 months of HCV diagnosis.
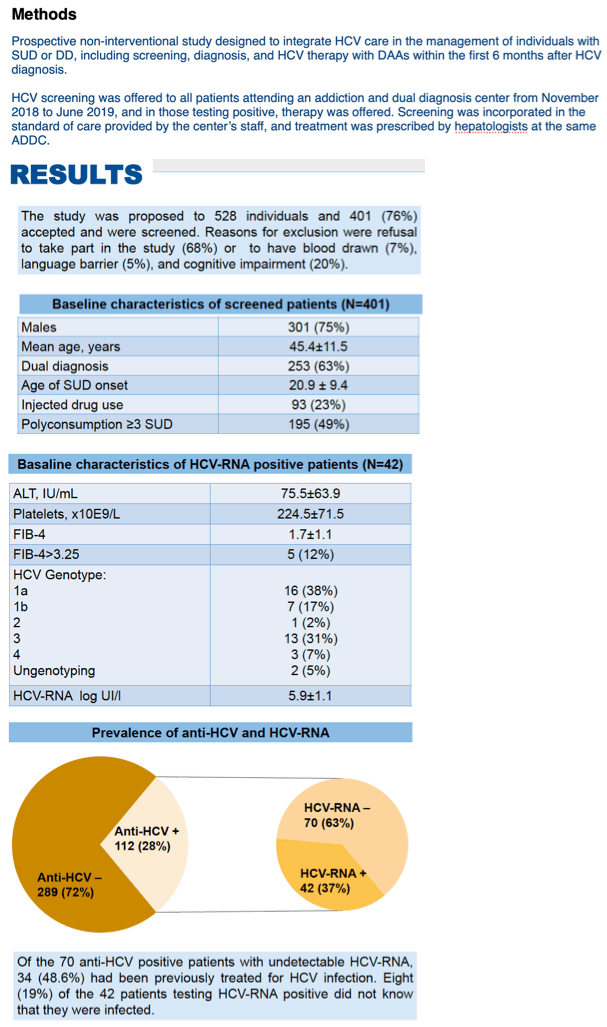
Health workers at the addiction center offered HCV screening to everyone seeking care at the center from November 2018 through June 2019. They offered DAA therapy to everyone positive for HCV RNA. Of the 528 people invited to enter the program, 401 (76%) agreed. Of those who declined to join, 68% did not want to be part of a study, 20% had cognitive impairment, 7% declined to have blood drawn, and 5% had a language barrier.
Of the 401 people who agreed to begin the program, 301 (75%) were men, age averaged 45.4 years, and age when SUD began averaged 20.9. There were 253 people (63%) with a dual diagnosis, 195 (49%) used 3 or more substances, and 93 (23%) injected drugs. Among these 401 people, 112 (28%) were anti-HCV-positive, meaning they had HCV infection sometime in the past. Of these 112 people, 42 (37.5%) tested positive for HCV RNA, meaning they had current HCV infection. Eight of the 42 people (19%) positive for HCV RNA did not already know they had HCV infection.
Compared with the 289 anti-HCV-negative people, the 112 positive for anti-HCV were more likely to have previous treatment for HCV (92% vs 81%, P = 0.007), more likely to have a criminal record (72% vs 27%), younger when SUD began (average 16.4 vs 22.7 years), more likely to inject drugs (72% vs 4%), more likely to use 3 or more substances (88% vs 34%), more likely to have benzodiazepine use disorder (54% vs 22%), and more likely to have cocaine use disorder (90% vs 46%) (all P < 0.0001 except previous HCV treatment). Only two factors differed significantly between HCV RNA-positive and negative people. Those positive for HCV RNA were less likely to be men (69% vs 89%, P = 0.010) and less likely to have previous treatment for SUD (59% vs 99%, P = 0.007).
Among the 42 HCV RNA-positive people, HCV load averaged 5.9 log10 IU/L and alanine aminotransferase (ALT) 75.5 IU/mL. Twenty of the 42 HCV RNA-positive people (48%) attended their first visit with a hepatologist and started DAAs. Of the 22 who did not keep the appointment, 18 were listed as loss to follow-up, 2 said they did not want to start therapy, and 2 went to hepatologists at other centers. Compared with people who started DAAs, those who did not were more likely to have a low academic level (53% vs 23%, P = 0.047) and used more cocaine in the last month (average 2.64 vs 0.55 g/week, P = 0.014). Fifteen of 20 people who started DAAs came back for their first SVR visit, and all 15 attained SVR12.
The researchers conclude that a dual diagnosis of substance use disorder and psychiatric illness did not appear to raise the risk of HCV infection or hinder access to treatment. They recommend centralized management and multidisciplinary care for people with substance use but caution that this strategy "does not suffice to ensure linkage to care and should be accompanied by preventive efforts and identification of risk factors."
Reference
1. Marcos Fosch C, Palma-Alvarez F, Rando A, et al. Screening and treatment difficulties of hepatitis C virus infected patients with substance use disorders or dual pathology, despite centralized management in an addiction and dual diagnosis center. EASL 2020, Digital International Liver Congress, August 27-29, 2020. Abstract THU344.
|
| |
|
 |
 |
|
|