 |
 |
 |
| |
One Third in US Stopped PrEP During COVID Shutdown, 90% Trimmed HIV Risk
|
| |
| |
AIDS 2020: 23rd International AIDS Conference Virtual, July 6-10, 2020
Mark Mascolini
One third of PrEP users responding to a US survey reported stopping PrEP during shelter-in-place orders (SIPO) because of the COVID-19 epidemic [1]. But almost 90% of providers did not recommend that patients change their PrEP routines during SIPO. About 90% of PrEP users reported no sex or less sex and avoiding Apps to find sex partners in this period.
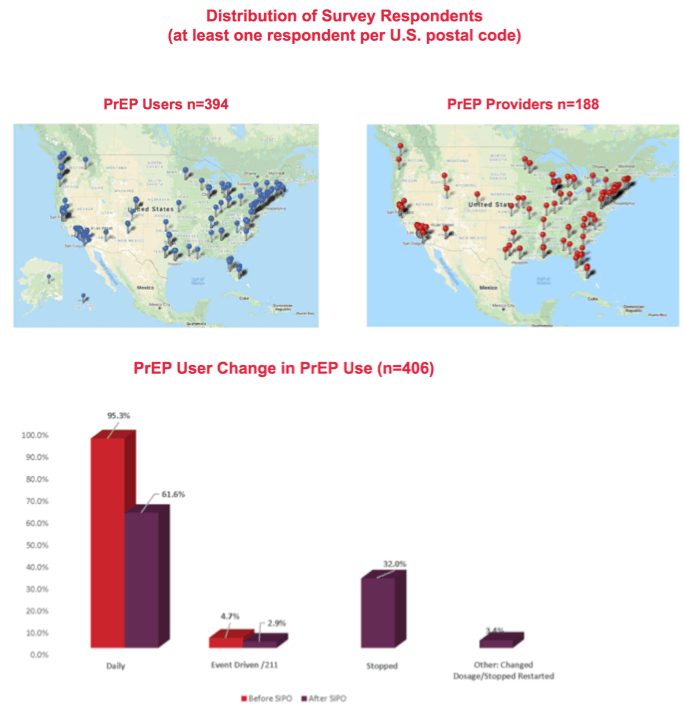
American Academy of HIV Medicine (AAHM) researchers and colleagues at other centers surveyed a convenience sample of US PrEP users and prescribers during 25 days at the height of SIPO in the United States. The research team contacted PrEP users via social media and snowball sampling of PrEP advocates; they reached PrEP providers via email to more than 2500 AAHM providers offering a link to an online survey.
The 394 PrEP user respondents and 188 providers lived mainly in the eastern half of the United States or on the west coast. One third of PrEP users (32%) stopped PrEP during SIPO. Proportions using PrEP daily fell from 95.3% before SIPO to 61.6% during SIPO, while proportions who used PrEP as needed shrank from 4.7% before SIPO to 2.9% during SIPO. In an Australian study also presented at AIDS 2020, 42% of gay or bisexual men stopped PrEP after COVID-19 arrived [2].
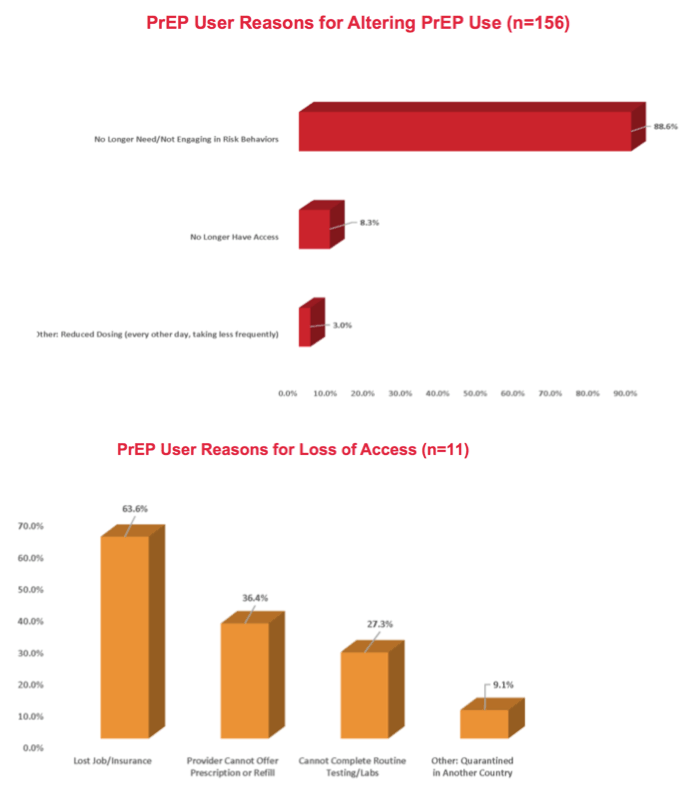
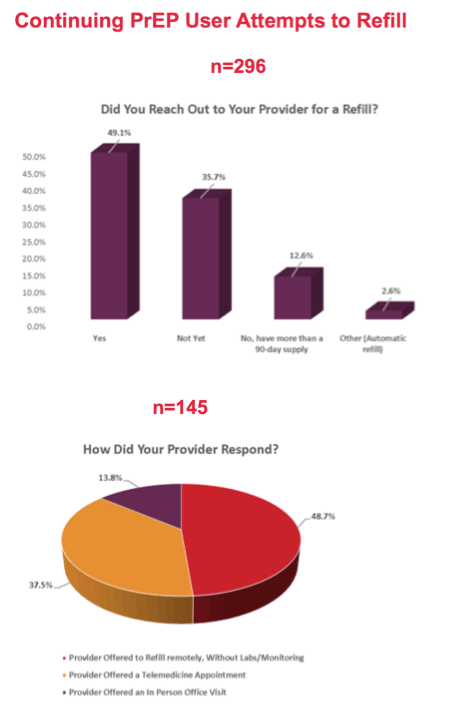
In the US study, among 156 PrEP users who altered PrEP use during SIPO, 88.6% did so because they no longer felt the need or no longer engaged in risk behaviors. Only 8.3% changed their PrEP habits because they could no longer get PrEP pills, and only 3.0% said they cut the frequency of PrEP. Among 11 people who lost access to PrEP, 7 lost their job or insurance, 4 could not get a prescription or refill, 3 could not complete routine testing needed for PrEP, and 1 got stuck outside the country. Among 296 PrEP users, 49.1% said they asked their provider for a PrEP refill during SIPO, 35.7% said they hadn’t asked yet, 12.6% hadn’t contacted their provider because they still had an adequate supply, and 2.6% had an automatic refill.
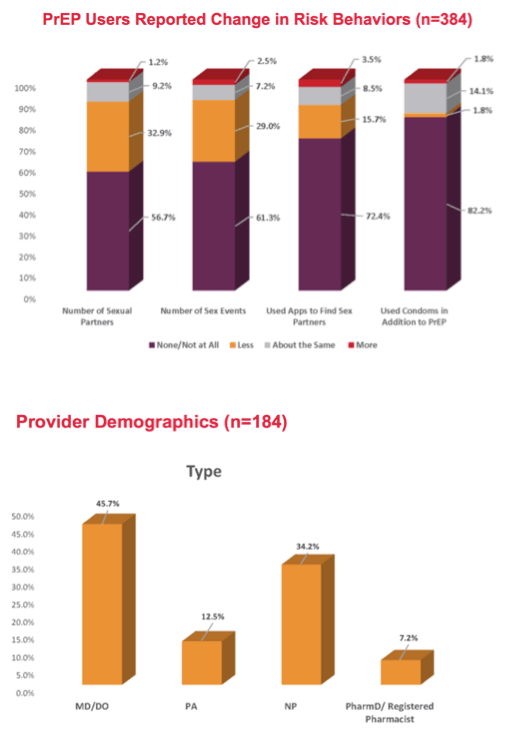
Among 384 PrEP users asked about HIV risk behavior during SIPO, 56.7% had no sex partners in that period, 32.9% had fewer sex partners, and the rest had the same number or more partners. Most respondents, 61.3%, reported having no sex during SIPO, while 29% had less sex. Almost three quarters, 72.4%, stopped using Apps to find sex partners, and 15.7% used Apps less.
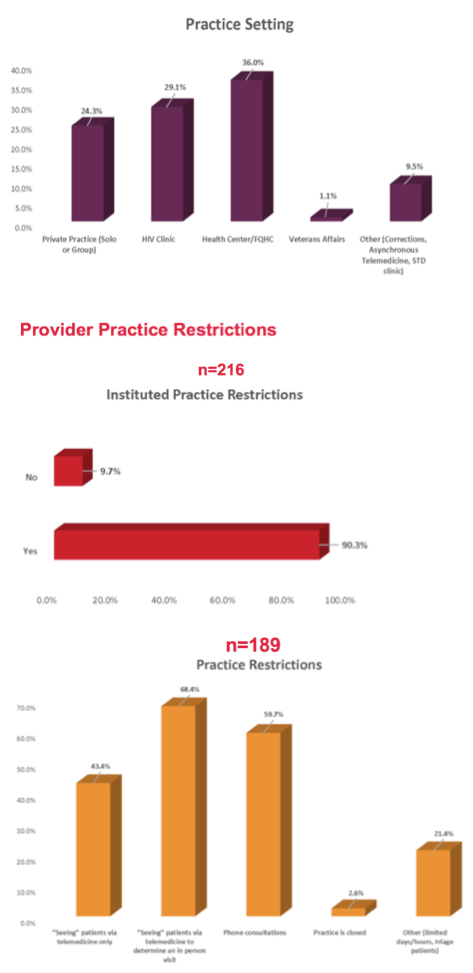
Of 184 provider respondents, 45.7% were MDs or DOs, 34.2% nurse practitioners, 12.5% physician assistants, and 7.2% pharmacists. Nine in 10 providers experienced practice restrictions during SIPO. The most frequent restrictions were screening patients via telemedicine (68.4%), having phone consultations (59.7%), and only seeing patients via telemedicine (43.4%). Only 2.4% of providers reported their practice closed during SIPO.
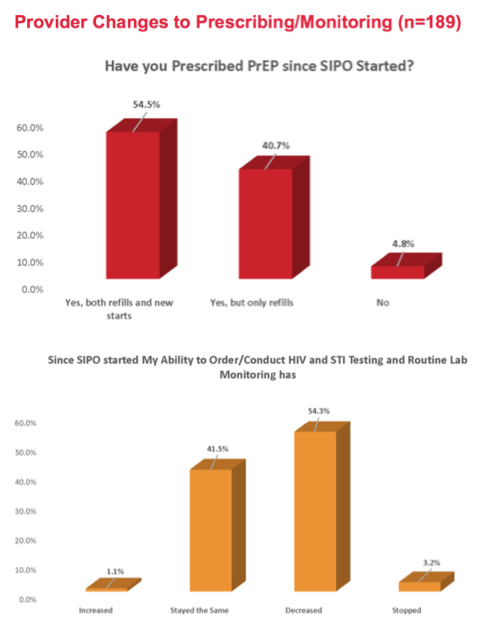
Just over half of 189 providers, 54.5%, wrote new PrEP prescriptions or authorized refills during SIPO, while 40.7% OK’d refills only. More than half, 54.3%, said their ability to test for HIV or sexually transmitted infection (STI) waned during SIPO, while 41.5% said that ability stayed the same. Only 3.2% said they could no longer test for HIV or STIs during SIPO.
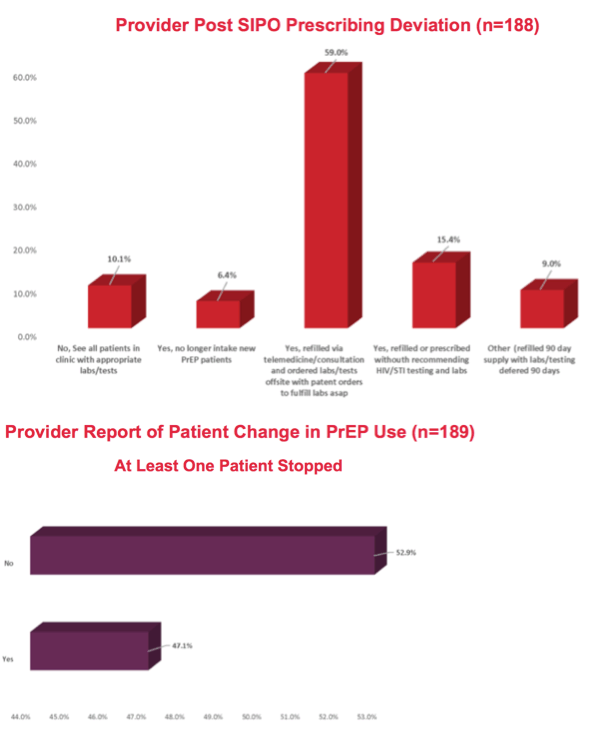
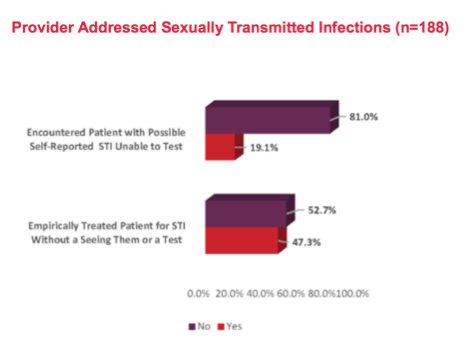
Among 189 providers, 52.9% said no patient stopped PrEP during SIPO, while 47.1% said at least 1 patient stopped. A large majority of prescribers, 88.9%, reported not recommending PrEP dose changes during SIPO. Only 1 in 5 providers, 19.1%, had a patient with a possible self-reported STI they could not test for during SIPO, and almost half, 47.3%, empirically treated a patient for an STI without seeing or testing them.
The researchers stressed that one third of PrEP-using respondents reported stopping PrEP during the SIPO period, but a big majority of that group stopped voluntarily. About 90% of PrEP users trimmed numbers of sex partners, numbers of sex acts, and use of Apps to meet partners. Most providers continued to prescribe PrEP during their SIPO span, despite some form of practice restriction reported by more than 90%.
Researchers pointed out one apparent disconnect between PrEP user and provider reports: The combined findings that 89% of providers did not recommend a change in PrEP routines during SIPO and the high frequency of empirical STI treatment indicate that providers felt their patients continued HIV risk behavior, whereas almost 90% of PrEP users who changed their PrEP routine claimed they did so because they reined in or gave up risk behaviors.
References
1. Brawley S, Dinger J, Nguyen C, Anderson J. Impact of COVID-19 related shelter-in-place orders on PrEP access, usage and HIV risk behaviors in the United States. AIDS 2020: 23rd International AIDS Conference Virtual. July 6-10, 2020. Abstract OADLB0101.
2. Grulich A, Maher L, Holt M, et al. Impact of social distancing due to COVID-19 on sexual behaviour among gay and bisexual men in Australia: Implications for trends in HIV and other sexually transmissible infections. AIDS 2020: 23rd International AIDS Conference Virtual. July 6-10, 2020. Abstract OACLB0103.




|
| |
|
 |
 |
|
|