 |
 |
 |
| |
Rates of COVID Testing, Diagnosis,
and Hospital Admission Higher With HIV
|
| |
| |
IDWeek 2020, October 22-25, 2020
Mark Mascolini
In a large Los Angeles-area healthcare system, people with HIV got tested for COVID-19 more than HIV-negative people, got diagnosed with COVID-19 at a higher rate, and went to the hospital for their coronavirus infection more often than people without HIV [1]. Race/ethnicity, comorbidities, and mortality did not differ significantly between COVID-19 patients with versus without HIV in this Kaiser Permanente analysis.
As the HIV and SARS-CoV-2 pandemics merged across the world, researchers scrambled to learn how these complex and potentially devastating viral infections might affect each other. Two key questions underlie much of this work: Would people with HIV prove more susceptible to COVID-19, and would COVID-19 be worse in people with HIV? Early attempts at answering these questions yielded some apparently contradictory answers because study populations and methods inevitably differ.
The large Kaiser Permanente healthcare system offers a chance to understand the impact of HIV/SARS-CoV-2 coinfection better because Kaiser researchers can compare large HIV populations with vast HIV-negative cohorts, all of them receiving similar care. Kaiser Permanente Southern California (KPSC) researchers set out to address several questions about HIV infection in the context of COVID-19 in a network that serves more than 4.6 million people.
This retrospective cohort study included all KPSC members 18 or older with at least 1 day of membership between March 1 and May 31, 2020. Researchers used electronic health records to identify members with HIV infection and to extract swaths of other clinical data relevant to this analysis. They identified COVID-19 patients with either a SARS-CoV-2 molecular diagnostic test or a clinical diagnosis by ICD-10 codes.
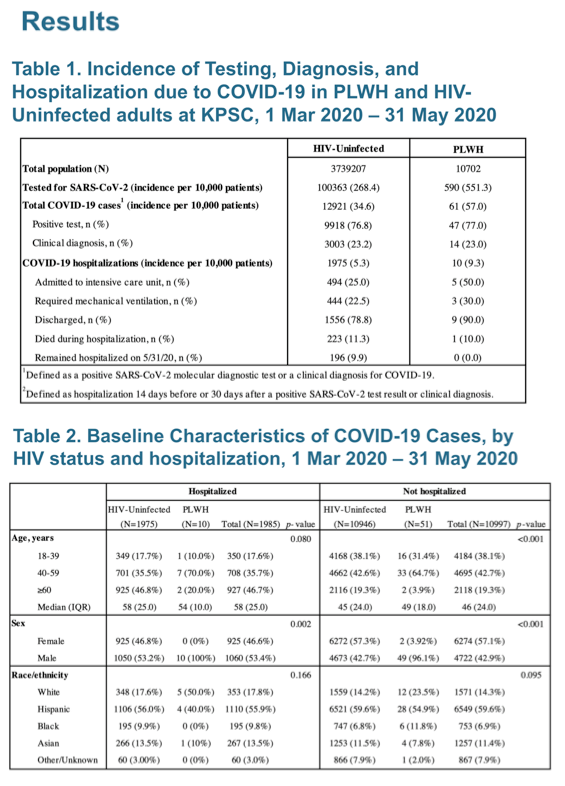
Kaiser records yielded 10,702 adults with HIV and 3,739,207 without HIV during the March-through-May study period. SARS-CoV-2 testing proved twice as frequent in the HIV group-551.3 versus 268.4 tests per 10,000 patients. Perhaps partly as a result, the COVID-19 diagnosis rate in people with HIV far exceeded the rate in HIV-negative KPSC members-57 versus 34.6 per 10,000. And COVID-19 hospital admissions proved almost twice as likely with than without HIV-9.3 versus 5.3 per 10,000.
Intensive care unit admission incidence in people with HIV doubled that in their HIV-negative counterparts-50 versus 25 per 10,000 patients. A higher proportion of people with than without HIV required mechanical ventilation-30 versus 22.5 per 10,000. But in-hospital mortality was similar with and without HIV-10 and 11.3 per 10,000. The researchers warned that the preceding comparisons may be more tenuous because of the low numbers of HIV-positive people for each outcome analyzed.
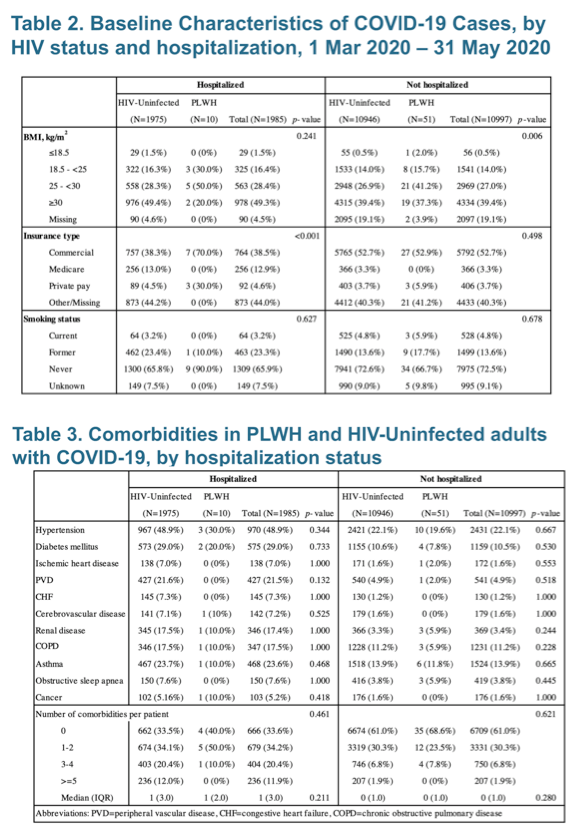
Comparing 10 HIV-positive and 1975 HIV-negative COVID-19 patients admitted to the hospital, the KPSC team found a nonsignificantly younger median age in the HIV group (54 versus 58, P = 0.080). In a similar comparison of 51 HIV-positive and 10,946 HIV-negative COVID-19 patients not sent to the hospital, the researchers found a significantly older age in the HIV group (49 versus 45, P < 0.001). Nearly everyone with COVID-19 and HIV was a man in both the inpatient and outpatient groups, compared with 53% of HIV-negative inpatients (P = 0.002) and 43% of HIV-negative outpatients (P < 0.001).
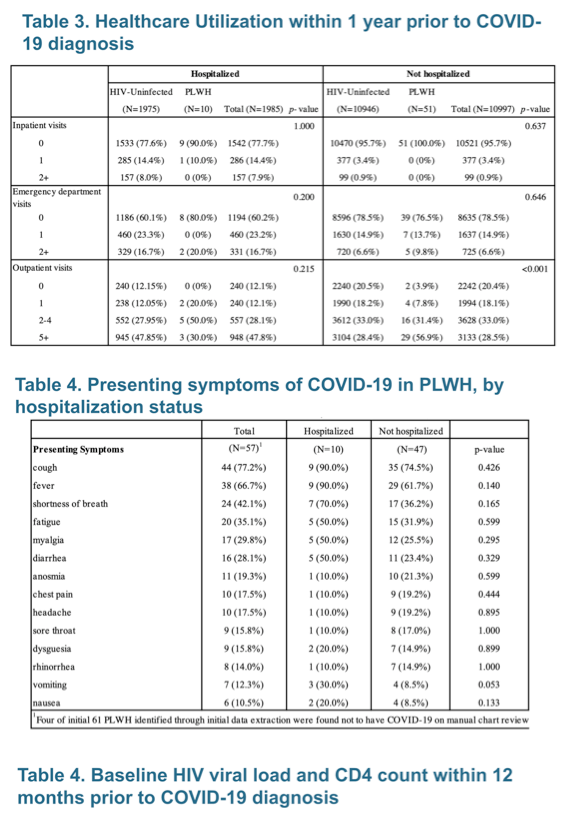
Comparing these same subgroups of HIV-positive and negative inpatients and outpatients, the researchers found no significant differences by HIV status in race or ethnicity, in body mass index, smoking status, or rates of 11 individual comorbidities or number of comorbidities per person, though all 11 comorbidities were more frequent in people admitted to the hospital than in those not admitted. Nor did the HIV-positive and negative subgroups differ significantly in number of inpatient visits or emergency department visits in the year before COVID-19 diagnosis. But HIV-positive outpatients had 5 or more outpatient visits significantly more often than HIV-negative outpatients (56.9% vs 28.4%, P < 0.001), partly because Kaiser typically requires at least two annual outpatient visits for people with HIV.
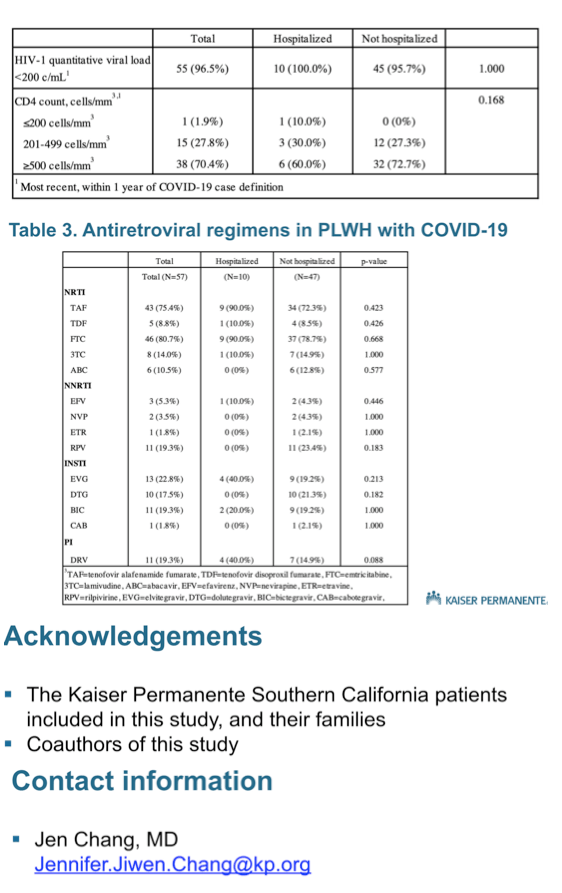
Comparing 10 HIV-positive COVID-19 inpatients with 47 HIV-positive COVID-19 outpatients, the researchers uncovered no significant differences in COVID-19 presenting symptoms, with the possible exception of more frequent vomiting in the inpatient group (30% versus 8.5%, P = 0.053). Among COVID-19 patients with HIV, almost all inpatients and outpatients had a viral load below 200 copies before COVID-19 diagnosis. CD4 count strata did not differ significantly between HIV-positive inpatients and outpatients. Individual antiretrovirals being used did not differ significantly between COVID-19 HIV patients admitted to the hospital and those staying home.
The KPSC investigators noted that only further study can determine whether HIV infection itself independently predicts poor outcomes with COVID-19.
Reference
1. Chang JJ, Bruxvoort K, Chen LH, et al. COVID-19 testing, characteristics, and outcomes among people living with HIV in an integrated health system. IDWeek 2020, October 22-25, 2020. Abstract 80.





|
| |
|
 |
 |
|
|