 |
 |
 |
| |
Risk factors for progression from prediabetes to diabetes in persons with HIV - Integrase Inhibitors Tied to Lower Risk of Progression from Prediabetes to Diabetes - HAILO
|
| |
| |
CROI 2021, Conference on Retroviruses and Opportunistic Infections, March 6-10, 2021
Mark Mascolini
Taking an integrase inhibitor regimen lowered risk of progression from prediabetes to diabetes in a US AIDS Clinical Trials Group (ACTG) cohort [1]. The finding is at odds with a US insurance database analysis that linked integrase inhibitor use to a higher risk of newly diagnosed prediabetes or diabetes [2]. The ACTG result also raises questions about how weight gain fits into the equation, since integrase inhibitors tend to raise weight and both higher body mass index and wider waists inflated progression risk in this analysis.
There is no question about the higher rates of diabetes in people with HIV than in the general population. But diabetes risk factors remain incompletely defined among people with HIV in the current antiretroviral era. A 111,652-person US medical insurance database analysis tied starting an integrase inhibitor regimen to new-onset diabetes (adjusted hazard ratio [aHR] 1.22), particularly with dolutegravir (aHR 1.47) or elvitegravir (aHR 1.20) but not with raltegravir [2].
The ACTG study took a different approach with a smaller cohort to find predictors of progression from prediabetes (fasting blood glucose 100 to 125 mg/dL) to diabetes (fasting blood glucose at or above 126 mg/dL, treatment for diabetes, or a clinical diagnosis). The study group consisted of people in ACTG A5322 (HAILO), an ongoing observational 32-site US cohort of people who began treatment for HIV in an ACTG trial and who have been in an ACTG group ever since.
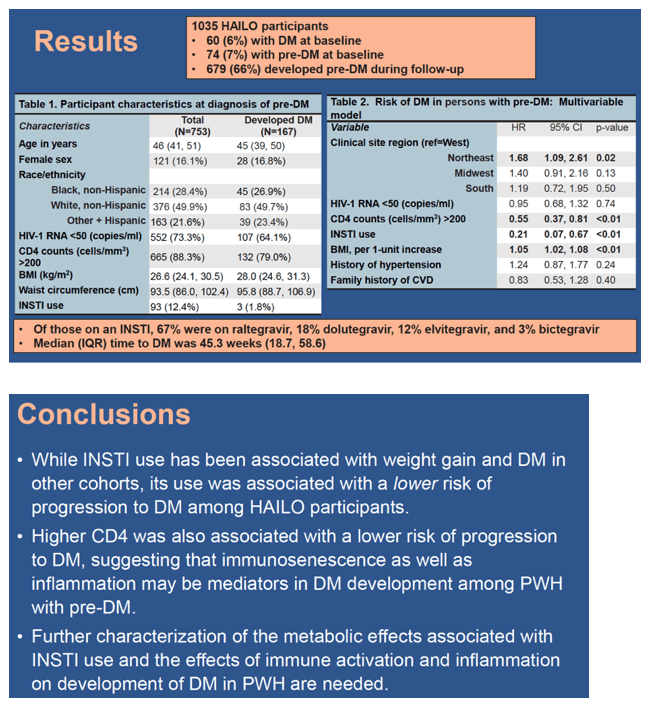
The analysis focused on 1035 HAILO participants, including 60 (6%) who had diabetes at their first HAILO visit and 74 (7%) who had prediabetes at their first visit. During follow-up prediabetes developed in another 679 people, a whopping two-thirds (66%) of the cohort. That gave the researchers 753 participants with prediabetes, 73% of the HAILO cohort.
Of these 753 people, at prediabetes diagnosis median age stood at 46 years, 16% were women, 50% white, 28% black, and 22% Hispanic. Median body mass index stood at 26.6 kg/m2 (in the lower overweight range), and median waist circumference measured 93.5 cm (36.8 inches). Two thirds of the group (73%) had a viral load below 50 copies at prediabetes diagnosis, and 88% had a CD4 count above 200.
Ninety-three of these people (12.4%) took an integrase inhibitor before or at diagnosis of their prediabetes. Among these 93 people, 67% took raltegravir, 18% dolutegravir, 12% elvitegravir, and 3% bictegravir.
Among the 753 people with prediabetes, diabetes developed in 167 (22%) in a median time of 45.3 weeks. Cox regression models identified four independent predictors of progression from prediabetes to diabetes. Living in the Northeast versus the West boosted progression risk by two thirds (aHR 1.68, 95% confidence interval [CI] 1.09 to 2.61, P = 0.02). A CD4 count above 200 at prediabetes diagnosis almost halved progression risk (aHR 0.55, 95% CI 0.37 to 0.81, P < 001). Every 1 unit higher body mass index hoisted progression risk 5% (aHR 1.05, 95% CI 1.02 to 1.08, P < 0.01). When the researchers substituted waist circumference for body mass index in the model, every 1-unit higher waist size upped progression risk 3% (aHR 1.03, 95% CI 1.01 to 1.04, P < 0.01).
Taking an integrase inhibitor regimen at or before a prediabetes diagnosis cut the risk of later progression to diabetes almost 80% (aHR 0.21, 95% CI 0.07 to 0.67, P < 0.01).
The HAILO team speculated that the link between higher CD4 count and lower risk of progression from prediabetes to diabetes could mean that immunosenescence and inflammation help drive diabetes development in HIV-positive people with prediabetes. But what explains the tie between integrase inhibitor use and lower progression risk, despite the tendency of integrase drugs to raise weight (and therefore diabetes risk)?
In a lively online discussion accompanying this poster, principal investigator Mary Clare Masters (Northwestern University) agreed with the suggestion of diabetes expert Todd Brown (Johns Hopkins University) that predominant use of raltegravir in the HAILO cohort (by 67%) could have influenced the association with lower progression risk since raltegravir had no impact on development of new diabetes in the big US insurance database study [2]. Brown wondered whether grouping the integrase inhibitors into older drugs (raltegravir and elvitegravir) and newer drugs (dolutegravir and bictegravir) would change the results.
Statistics and epidemiology maven Caroline Sabin (University College London) said she always gets suspicious when she sees an "extremely strong association" (like 0.2) for an antiretroviral effect. Clinicians would notice an association that strong in the clinic, she maintained. Sabin wondered if other antiretrovirals in the regimens had an impact or whether unmeasured biases weakened the model. She thought it would be interesting to include integrase inhibitor use as a time-updated covariate in the model.
References
1. Masters MCC, Bao Y, Tassiopoulos K, et al. Risk factors for progression from prediabetes to diabetes in persons with HIV. CROI 2021, Conference on Retroviruses and Opportunistic Infections, March 6-10, 2021. Abstract 518.
2. O'Halloran J, Sahrmann J, Olsen M, et al. Incident diabetes associated with integrase strand transfer inhibitor initiation. CROI 2021, Conference on Retroviruses and Opportunistic Infections, March 6-10, 2021. Abstract 516.

|
| |
|
 |
 |
|
|