 |
 |
 |
| |
COST-EFFECTIVENESS OF HCV TESTING STRATEGIES FOR HCV ELIMINATION AMONG MSM IN THE US
|
| |
| |
CROI 2021 March 6-10 Reported by Jules Levin
Antoine Chaillon1, Louis MacGregor2, Peter Vickerman2, Daniel Fierer3, Natasha Martin1
1University of California San Diego, La Jolla, CA, USA, 2University of Bristol, Bristol, UK, 3Mt Sinai School of Medicine, New York, NY, USA
Background: Background: Despite current hepatitis C virus (HCV) elimination efforts in the United States (US), men who have sex with men (MSM), both with HIV and without HIV, continue to have high rates of HCV transmission. We hypothesized that better testing could result in a lower rate of transmission. We therefore used a cost-effectiveness model to determine the optimal HCV testing strategies for HCV elimination among MSM.
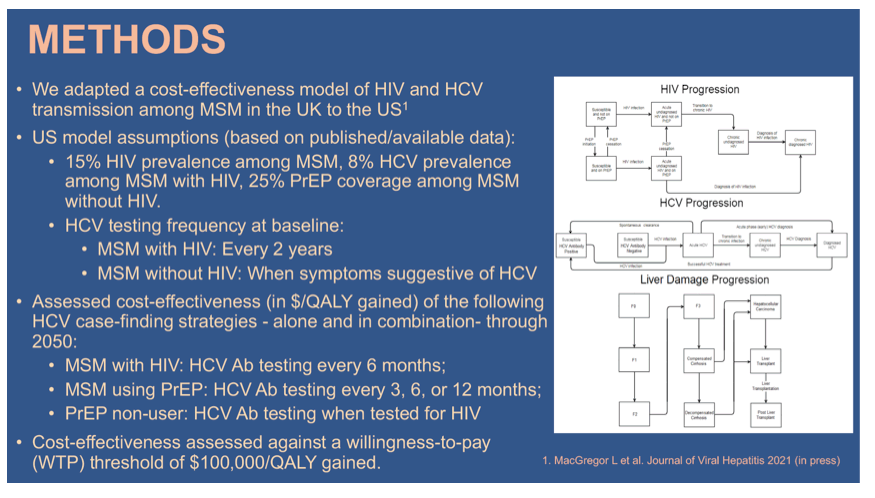
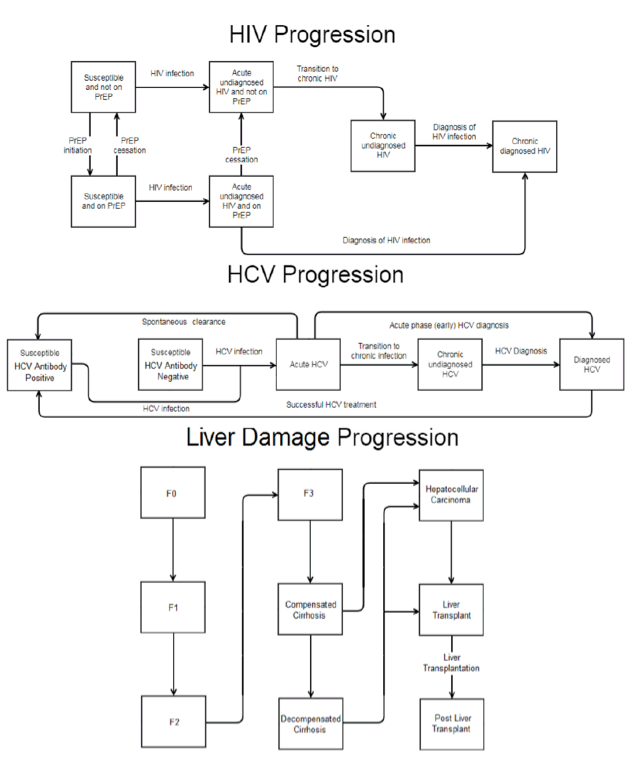
Methods: Methods: We adapted a cost-effectiveness model of HIV and HCV transmission among MSM to determine the cost-effectiveness of improving HCV testing strategies among MSM in the US. The model assumed 15% HIV prevalence among MSM, 8% HCV prevalence among MSM with HIV, and 25% PrEP coverage among MSM without HIV. We evaluated testing strategies
that could achieve a 90% reduction in HCV incidence from 2015 as a baseline, through 2030. At baseline, we assumed no systematic HCV screening (i.e. testing only for symptoms) in MSM without HIV not using PrEP (PrEP non-users) and the currently recommended frequency of HCV screening among MSM with HIV (~50%/year). We assessed the following HCV case-finding strategies: screening in parallel with HIV testing in PrEP non-users; screening every 12/6/3 months in MSM using PrEP; and screening every 6 months in MSM with HIV. These strategies were considered alone and in combination, with the cost-effectiveness compared incrementally. Costs (USD) and quality adjusted life-years (QALYs) were assessed to estimate the mean incremental cost-effectiveness ratio (ICER) through 2050, compared to a willingness-to-pay (WTP) threshold of $100,000/QALY gained.
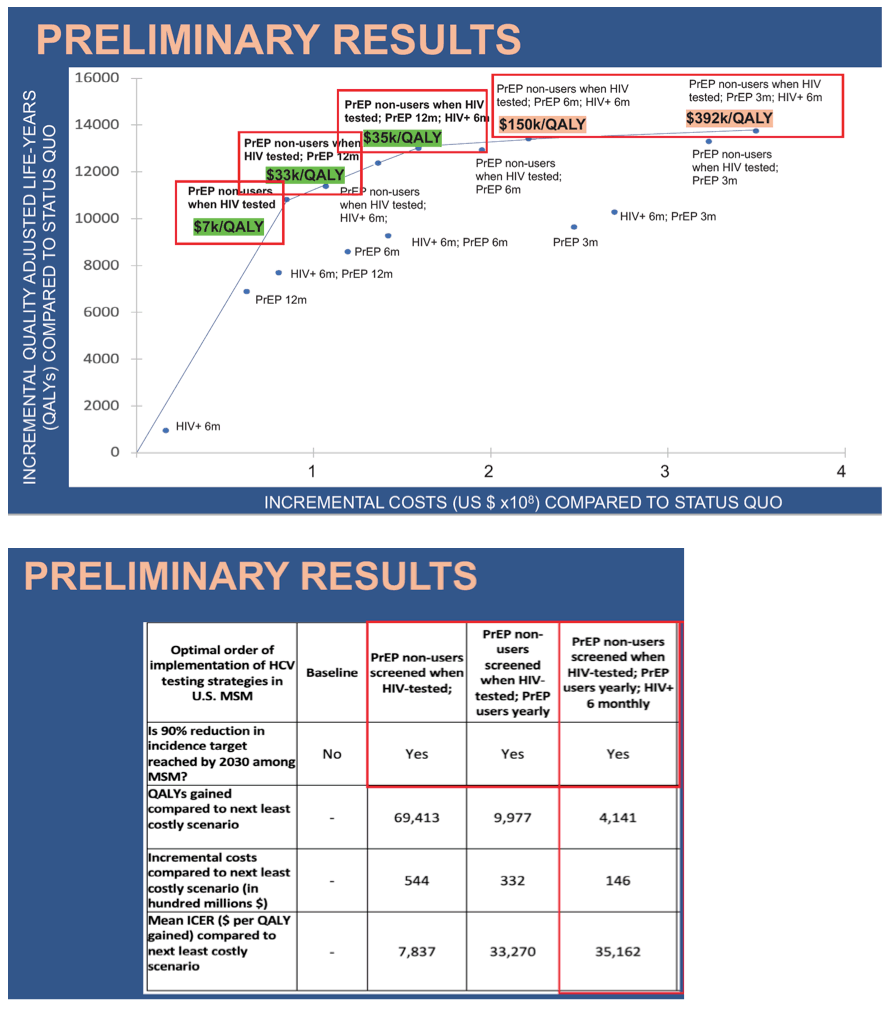
Results: Results: Our economic model predicted the optimal HCV testing strategy to achieve HCV elimination among MSM in the US to be every 6 months for MSM with HIV; annually for MSM using PrEP; and at the time of HIV testing for PrEP non-users. This testing schedule resulted in an incremental ICER of $35,000/QALY gained (Table 1).
Conclusion: Conclusions: HCV elimination can be achieved among MSM in U.S. by a relatively nominal and logistically feasible increase in the frequency of HCV screening over what is currently recommended, and is cost-effective.

"Increasing to every 6 or 3 months increased benefits (brown highlighted) but were substantially more costly with OCERs falling above the willingness to pay threshold indicating they are unlikely to be cost effective.” Natasha Martin
|
| |
|
 |
 |
|
|