 |
 |
 |
| |
HIV REBOUND IN CONTROLLERS IS ASSOCIATED WITH SPECIFIC FECAL MICROBIOME PROFILE
|
| |
| |
CROI 2021 March 6-10 Reported by Jules Levin
Yanhui Cai1, Steven G. Deeks2, Cynthia Brinson3, Moti Ramgopal4, Norman Jones2, Edwin DeJesus5, Anthony Mills6, Peter Shalit7, Brian Moldt1, Liao Zhang1, Elena Vendrame1, Devi SenGupta1, Diana Brainard1, Jeffrey Wallin1, Ondrej Podlaha1
1Gilead Sciences, Inc, Foster City, CA, USA, 2University of California San Francisco, San Francisco, CA, USA, 3Central Texas Clinical Research, Austin, TX, USA, 4Midway Immunology and Research Center, Fort Pierce, FL, USA, 5Orlando Immunology Center, Orlando, FL, USA, 6Mens Health Foundation, West Hollywood, CA, USA, 7Peter Shalit MD and Associates, Seattle, WA, USA
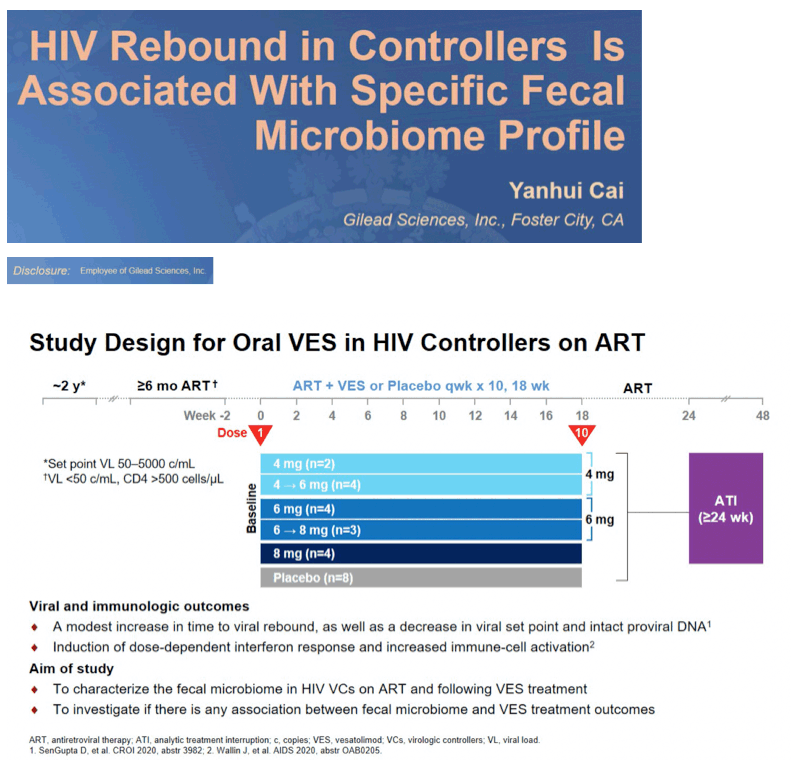
Background: HIV infection negatively impacts gut immune homeostasis and frequently leads to dysbiosis which can only be partially restored by antiretroviral therapy (ART) in people with HIV (PWH). In a placebo-controlled Phase 1b trial, vesatolimod (VES), an oral TLR7 agonist, was shown to increase interferon stimulated genes (ISGs), immune cell activation, and modestly delay viral rebound after ART interruption in HIV virologic controllers (VC). We investigated the fecal microbiome dynamics and association with virologic outcome in this trial.
Methods: We enrolled 25 VC (pre-ART viral load 50-5000 c/mL) on ART. Seventeen participants received 10 biweekly VES doses, and 8 received placebo prior to an analytical treatment interruption (ATI). Fecal samples from male participants were assessed at baseline and 2 weeks after the 10th dose for microbial abundance and diversity evaluation. Feces from an additional 14 male healthy volunteers and 9 male ART-suppressed chronic HIV infected participants (CHI) were included to assess baseline differences due to HIV infection by Wilcoxon test. Associations between immune biomarkers and bacterial abundance at the phylum level were measured by Spearman's rank correlation. A univariate Cox Proportional Hazard regression model explored the association between time to viral rebound and the abundance of microbiota species.
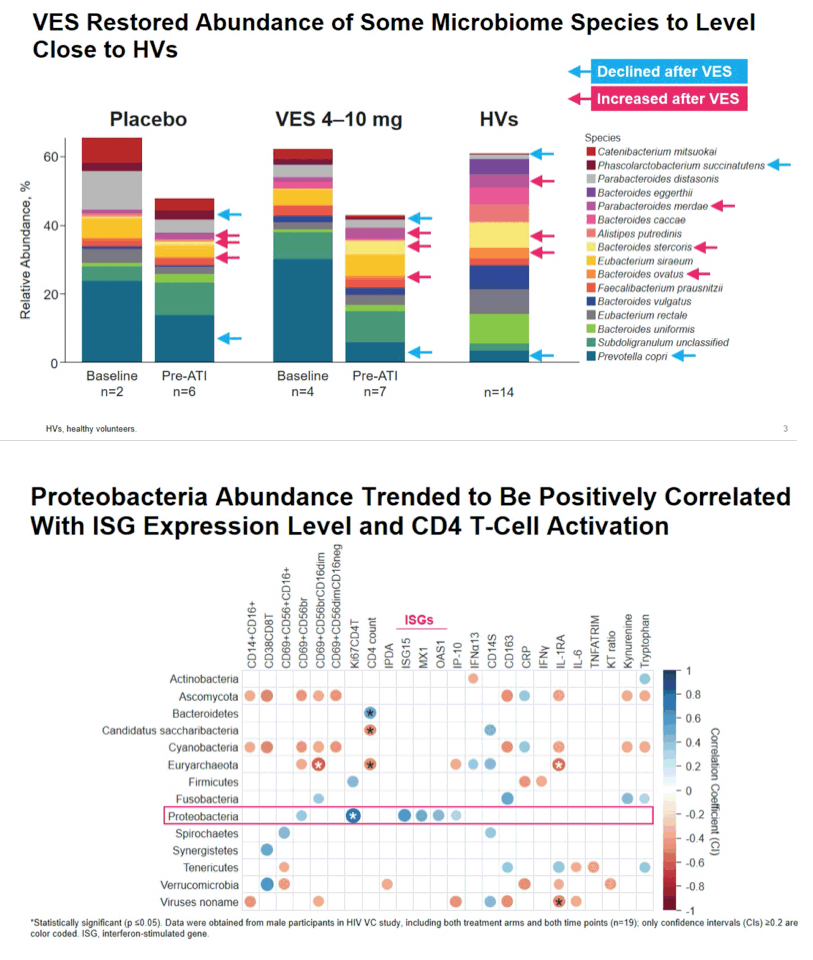
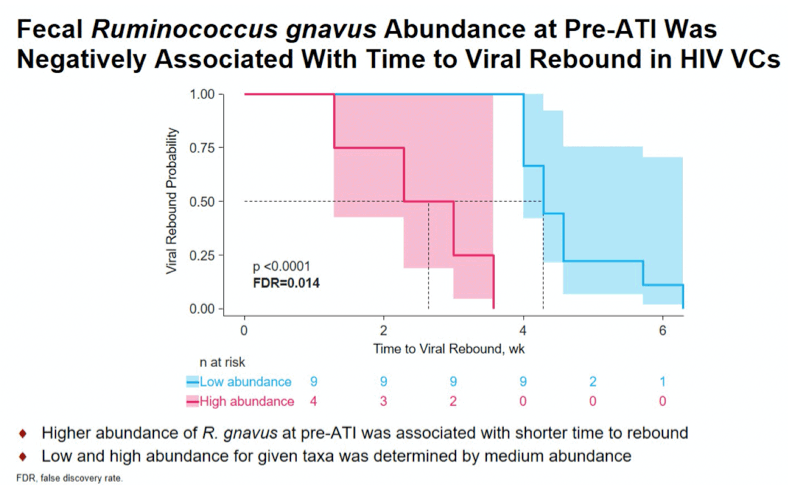
Results: Prevotella copri was enriched in VC at baseline (p=0.0018), as well as in CHI (p=0.0024), compared to healthy volunteers. VES partially reversed this dysbiosis by decreasing Prevotella copri levels closer to those in healthy volunteers. Proteobacteria abundance was positively correlated with VES-induced elevation of ISGs and Ki67+CD4+ T cells (r=0.75, p=0.01). Higher abundance of fecal Rumminococcus gnavus at the pre-ATI timepoint was associated with shorter time to viral rebound after ATI in the overall study population (FDR adjusted p-value=0.014).
Conclusion: The enrichment of certain microbiome species may contribute to HIV persistence, as evidenced by faster rebound off ART. VES enhances the immune response and can potentially favorably alter the composition of the fecal microbiome. Further studies are needed to understand the mechanistic interactions between immune modulation and microbiome, and subsequent impacts on antiviral responses and HIV reservoir in cure studies.

|
| |
|
 |
 |
|
|