 |
 |
 |
| |
CHANGES IN ACCESS TO CARE FOR WOMEN LIVING WITH HIV DURING THE COVID-19 PANDEMIC
|
| |
| |
CROI 2021 March 6-10 Reported by Jules Levin
Caitlin Bernard1, John M. Humphrey2, Julie Thorn3, Shukri Hassan4, Victor Omodi5 , Beatrice Jakait6, Kara Wools-Kaloustian1, Rena Patel4, Mercy Maina6
1Indiana University, Indianapolis, IN, USA, 2Indiana University, Bloomington, IN, USA, 3University of Toronto, Toronto, Canada, University of Washington, Seattle, WA, USA, 4Academic Model Providing Access to Healthcare, Eldoret, Kenya, 6Moi Teaching and Referral Hospital, Eldoret, Kenya
Background: The COVID-19 pandemic has disrupted health services globally. We examined the self-reported impact of the pandemic on access to HIV and family planning (FP) services among women living with HIV (WLHIV) at a large HIV treatment program in Kenya.
Methods: Telephone surveys were conducted among a non-random, purposeful sample of WLHIV ≥15 years of age exposed to dolutegravir
(DTG) at HIV clinics affiliated with the Academic Model Providing Access to Healthcare (AMPATH), a PEPFAR-supported treatment program in western Kenya. Participants completing phone interviews for a DTG-focused study named Chaguo Langu were asked structured questions about their HIV and FP experiences and pregnancy intentions in the context of the pandemic. Multivariable logistic models were used to estimate the odds of self-reported difficulty refilling medications and obtaining care, respectively, adjusted for age, partner status, number of children, time on ART, and HIV clinic site.
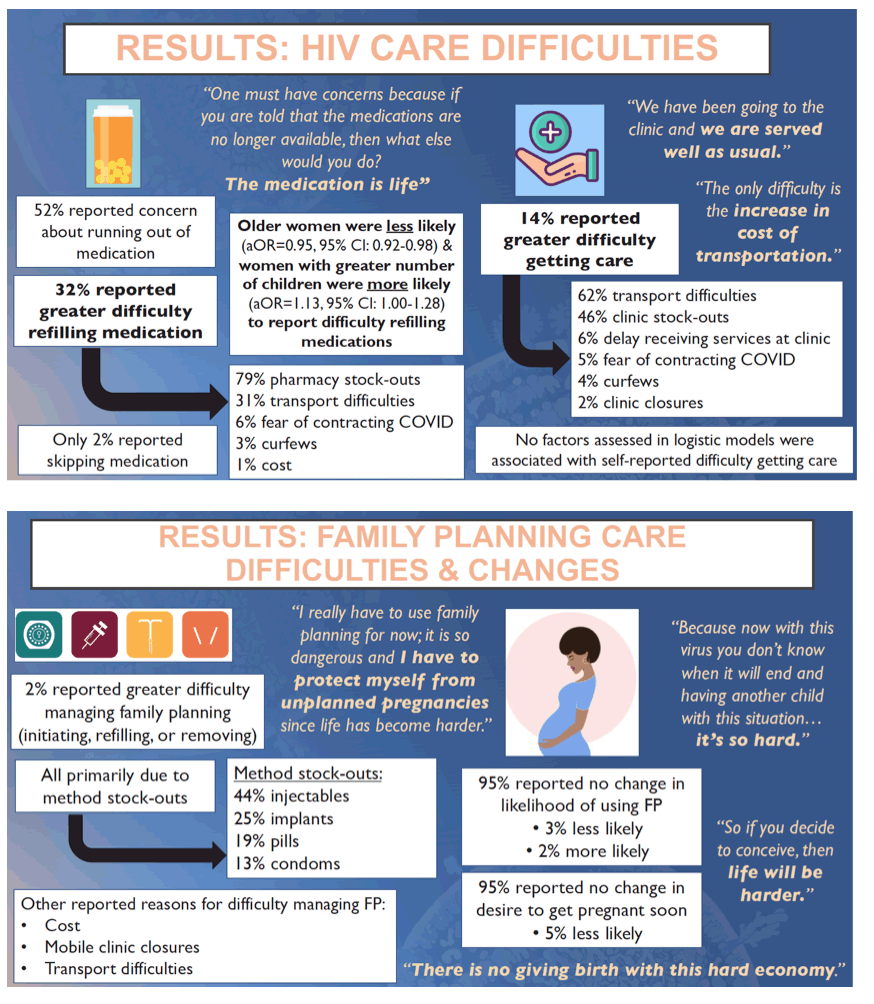
Results: Among 814 women called from June-October 2020, 784 (96%) completed the survey. Overall, 14% reported experiencing increased difficulty obtaining care during the pandemic, primarily due to cost or unavailability of transportation (61%). Further, 32% reported increased difficulty refilling medications during the pandemic, primarily due to medication stock-outs (79%). However, only 2% reported missing medication doses. Only 2% reported increased difficulty managing (including initiating, refilling, and removing) FP methods, primarily due to stock-outs of implants and injectables (69%). Most (95%) reported no impact of the pandemic on their intentions to use FP or become pregnant. None of the factors assessed in the multivariable model were associated with difficulty obtaining care. Older women were less likely (aOR=0.95, 95% CI: 0.92-0.98), and women with a higher number of children were more likely (aOR=1.13, 95% CI: 1.00-1.28) to have an association with difficulty refilling medications.
Conclusion: A significant proportion of WLHIV report experiencing greater difficulty obtaining HIV care and medication refills during the pandemic, while women's ability to manage FP during the pandemic largely remained stable. Addressing medication stock-outs and transportation challenges may help HIV programs in resource-constrained settings ensure that access to HIV and FP services is not disrupted during the COVID-19 pandemic. As the pandemic continues, FP access and use should continue to be monitored to avoid unintended pregnancies.


|
| |
|
 |
 |
|
|