 |
 |
 |
| |
CANNABIS USE ASSOCIATED WITH DECREASED
ART ADHERENCE IN AGING PEOPLE WITH HIV
|
| |
| |
CROI 2021 Reported by Jules Levin
Jennifer A . Manuzak1, Janeway Granche2, Katherine Tassiopoulos2, Ronald J. Ellis3, Karl Goodkin4, Anjali Sharma5, Kristine Erlandson6, for the ACTG A5322 Study Team
1Tulane National Primate Research Center, Covington, LA, USA, 2Harvard TH Chan School of Public Health, Boston, MA, USA, 3University of California San Diego, La Jolla, CA, USA, 4University of Nebraska Medical Center, Omaha, NE, USA, 5Albert Einstein College of Medicine, Bronx, NY, USA, 6University of Colorado Anschutz Medical Campus, Aurora, CO, USA
Background: Cannabis is commonly used in the United States, particularly among people with HIV (PWH). Conflicting evidence exists on the impact of cannabis use on care of PWH, particularly among older adults. Here, we leveraged data collected through ACTG A5322, an observational study of PWH ≥40 years in long-term follow-up, to longitudinally characterize associations between cannabis use and antiretroviral therapy (ART) adherence.
Methods: A5322 participants with ≥2 substance use surveys were included. At each visit, participants were categorized as 100% ART adherent if they indicated no missed doses of antiretroviral medication within the past 7 days, and as <100% adherent otherwise; visits during which participants were not on ART were excluded. Cannabis use was updated at each visit; participants were were categorized as current cannabis users if they reported use within the past month, intermittent users if they reported use within the past year but >1 month ago, and non-users if they reported use ≥1 year ago or never. Generalized linear models using generalized estimating equations (GEE) were fit. Inverse probability weighting (IPW) was used to adjust for static and time- varying confounders and drop-out.
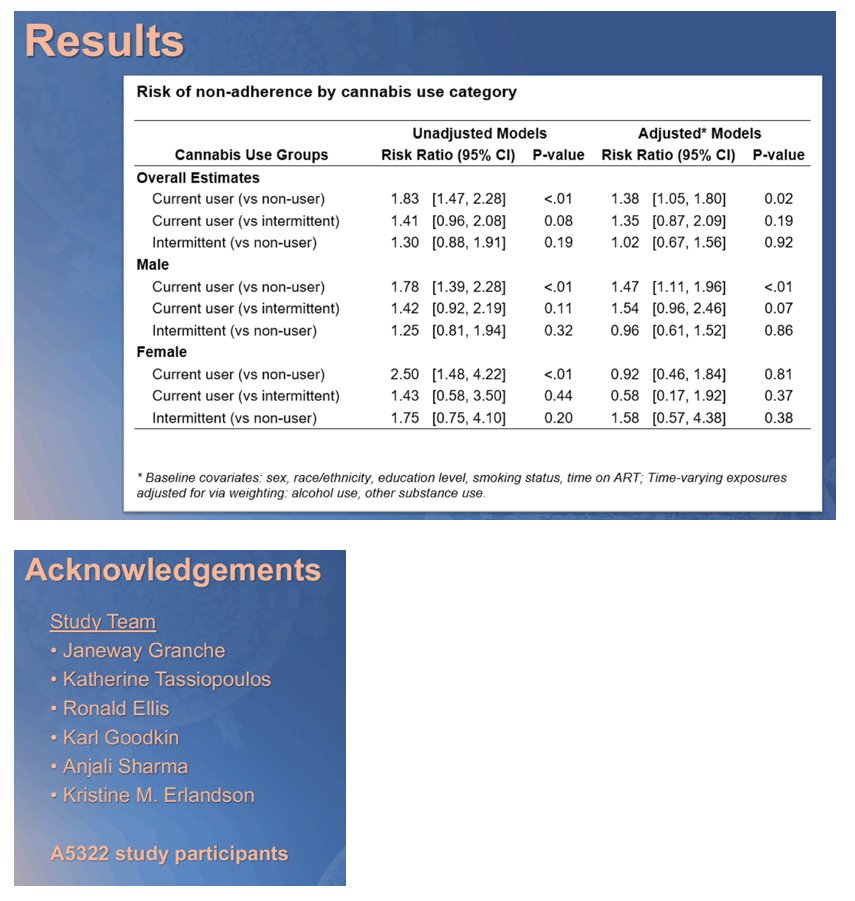
Results: A total of 963 participants contributed up to 6 years of data. At A5322 entry, 18% reported current cannabis use, 6% intermittent use, and 76% non-use; 88% reported 100% ART adherence. Mean age at entry was 51 years, 81% were male at birth, and 49% identified as White non-Hispanic, 30% as Black non-Hispanic, 18% as Hispanic and 2% another race/ethnicity. Participants who were cannabis users and reported current use were more likely to be <100% ART adherent than non-users (adjusted relative risk [aRR]=1.65, CI95=1.26, 2.16) and intermittent users (aRR=1.68, CI95=1.01, 2.81) (Table). There was no association between intermittent vs non-use and ART adherence (aRR=0.98, CI95=0.61, 1.57).
Conclusion: Current cannabis-using PWH had a higher risk of being <100% adherent to their ART regimen when compared to intermittent and non-users. These findings have clinical implications, as poor ART adherence is associated with less effective viral suppression, drug resistance and comorbidities. Further research is needed to elucidate the underlying biobehavioral mechanisms by which cannabis use elicits decreased ART adherence in older PWH and the downstream impacts on risk for comorbid conditions.



|
| |
|
 |
 |
|
|