 |
 |
 |
| |
12-Year Cognitive Decline is Associated with Lung Disease, Diabetes, and Depression
|
| |
| |
CROI 2021 March 6-10 Reported by Jules Levin
Scott Letendre, M.D
University of California, San Diego
San Diego, California USA
Scott Letendre1, Ronald J. Ellis1, Bin Tang1, Donald Franklin1, Ned Sacktor2, Leah Rubin2, Susan Morgello3, J. Allen McCutchan1, Christina M. Marra4, Benjamin B. Gelman5, Ann C. Collier4, David Clifford6, Robert K. Heaton1
1University of California San Diego, San Diego, CA, USA, 2Johns Hopkins University School of Medicine, Baltimore, MD, USA, 3Icahn School of Medicine at Mt Sinai, New York, NY, USA, 4University of Washington, Seattle, WA, USA, 5University of Texas at Galveston, Galveston, TX, USA, 6Washington University in St Louis, St Louis, MO, USA
Background: Cognitive impairment is more common in people with HIV (PWH) than in the general population and is associated with worse quality of life and worse health outcomes. Most studies of cognitive change in PWH have focused on decline over a few years but no projects have assessed cognitive change and its correlates over more than a decade. To address this key gap, the 6-site, U.S. CHARTER project reassessed 397 participants 12 years after their initial assessment.
Methods: Standardized, comprehensive neuromedical and neurocognitive assessments were performed at the initial and 12-year timepoints and included a neuropsychological test battery that assessed 7 cognitive domains as well as medical history, prescribed medications, drug use, and blood collection. The outcome was regression-based change score (RBCS), which was calculated using normative data from people without HIV. Decline was defined as change worse than the 5th percentile of the normative data. Demographic, disease, drug use, and therapy characteristics were analyzed using multivariable regression with α=0.20 for covariate inclusion.
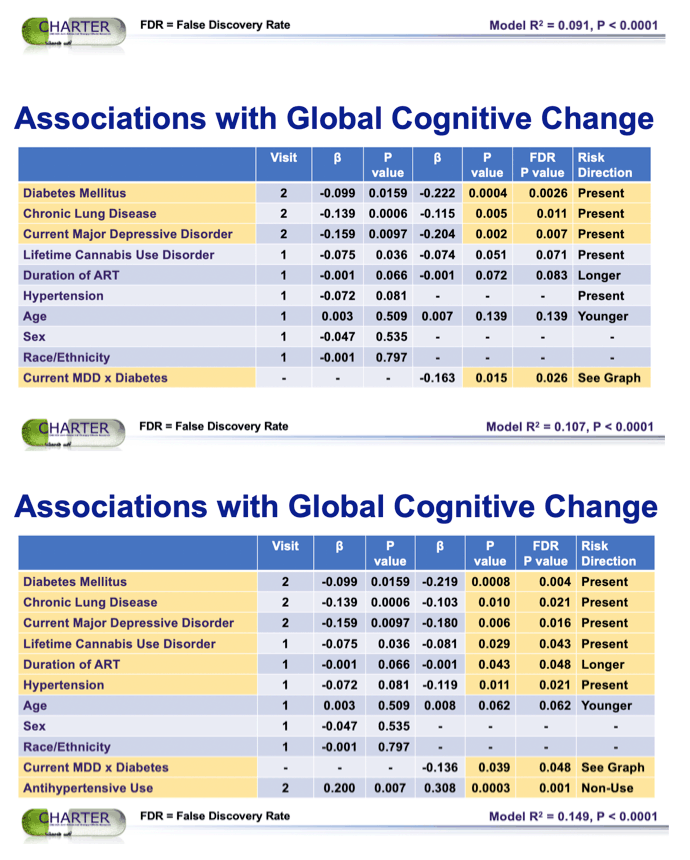
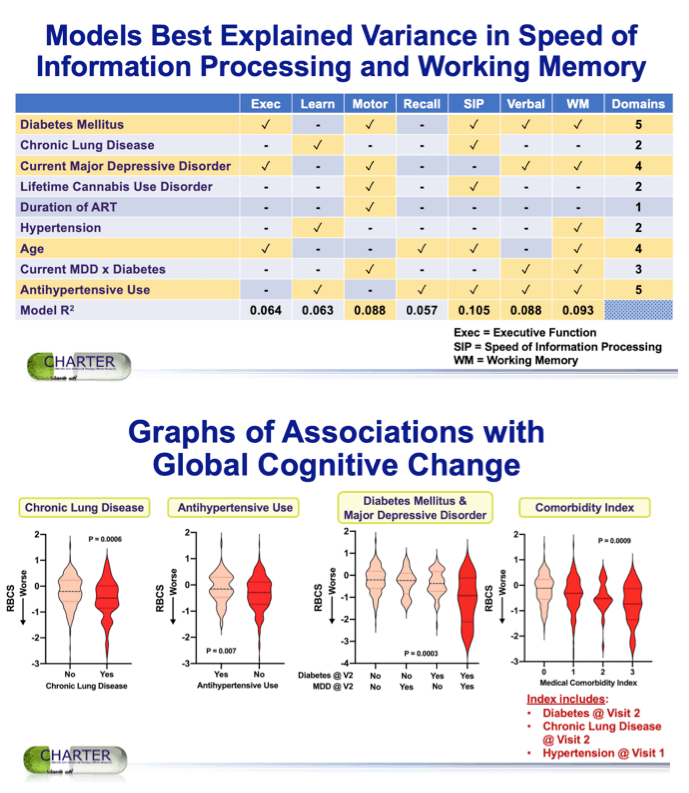
Results: At the 12-year visit, mean age was 56 (range 33-81), 23% were women, 58% had race/ethnicity other than white, and 96% took antiretroviral therapy (ART, mean 15.3 years) with mean CD4+ T-cell count 607/μL and plasma HIV RNA ≤ 200 cp/mL in 90%. The criterion for cognitive decline was met in 23.4%. In the best model, worse RBCS was associated with chronic lung disease (p=0.002) and lifetime cannabis use disorder (p=0.037) (model p<0.0001). The model also included an interaction between diabetes and major depressive disorder (MDD) (p=0.026): people with diabetes and MDD had worse cognitive decline than people with diabetes without MDD or people with neither condition. Hypertension also entered some models and a comorbidity index that combined it with diabetes and chronic lung disease was incrementally associated with decline (p<0.0001).
During the Q&A Dr Letendre was asked about the association with cannabis & he said in his experience mild to moderate use is not associated with decline but higher use he thinks is what they found. In my opinion, perhaps any use has negative impact for some not just on cognition but other affects including heart disease and lung disease. Jules
Conclusion: Nearly a quarter of treated PWH experienced cognitive decline over 12 years and worse change was associated with previously reported aging- related risk factors (e.g., diabetes) but also with other risk factors that have not been reported (chronic lung disease, MDD, cannabis use disorder). The CHARTER cohort was intended to reflect PWH who receive outpatient healthcare in the U.S. when it was first recruited but these 12-year findings may be affected by survivor bias and selection bias.


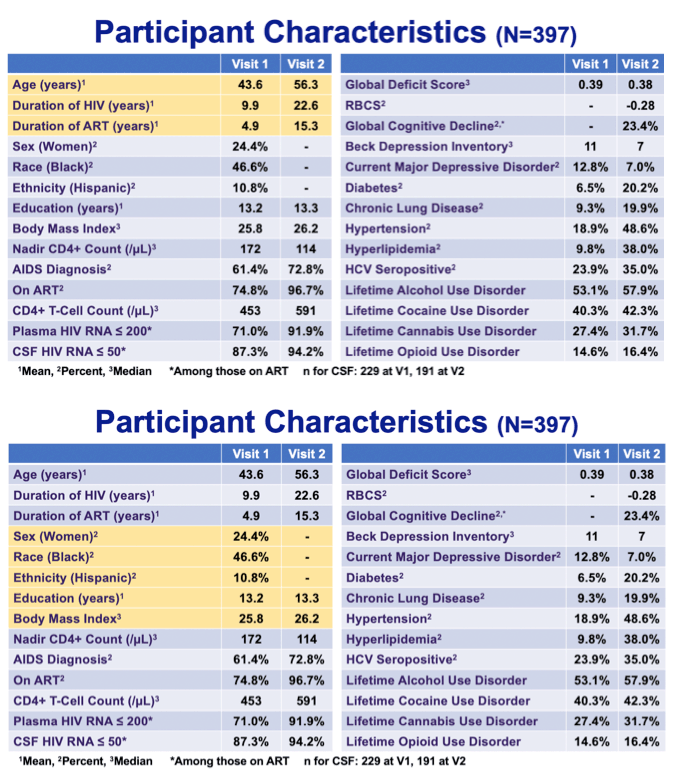
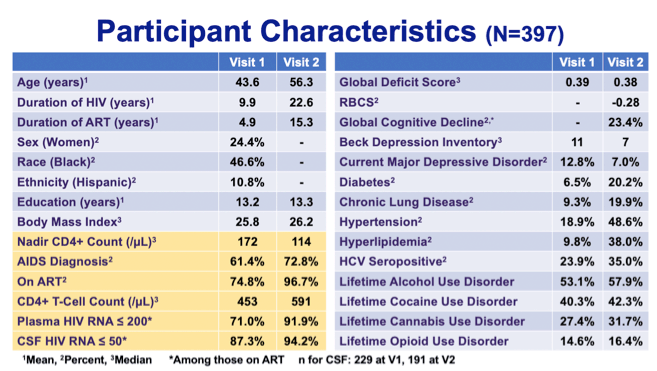
note: 23.4% had global cognitive decline at visit 2. Lentedre said median Global Deficit score above 0.5 is considered bad so 0.38 is blow that but bear in mind that 0.38 is a median. Note the increases in comorbidities from visit 1 to 2. Jules
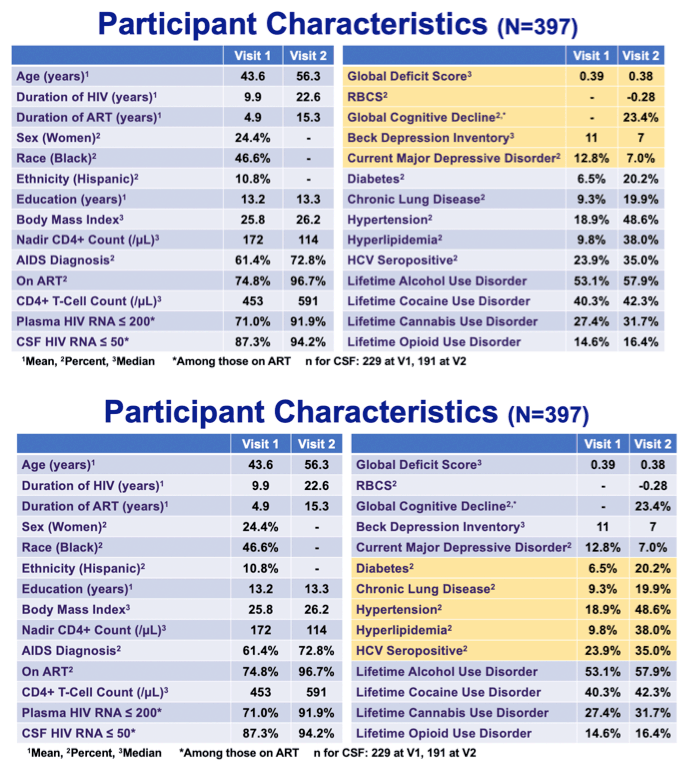
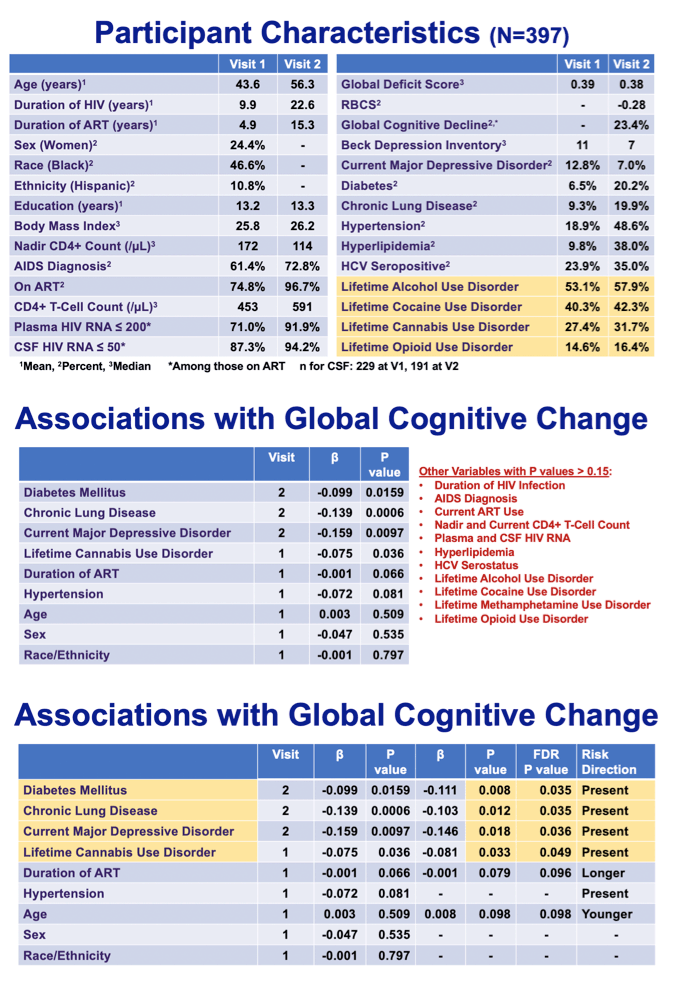

|
| |
|
 |
 |
|
|