 |
 |
 |
| |
Short-course alendronate for the prevention
of art-associated bone loss
Alendronate for 14 Weeks Before and
During First ART Wards Off 48-Week Bone Loss
|
| |
| |
CROI 2021, Conference on Retroviruses and Opportunistic Infections, March 6-10, 2021
Mark Mascolini
Taking oral alendronate for 14 weeks, beginning 2 weeks before starting antiretroviral therapy (ART), prevented total hip bone loss through 48 weeks of ART in a 50-person double-blind, placebo-controlled trial [1]. At the lumbar spine this protective effect lasted through 24 weeks of ART.
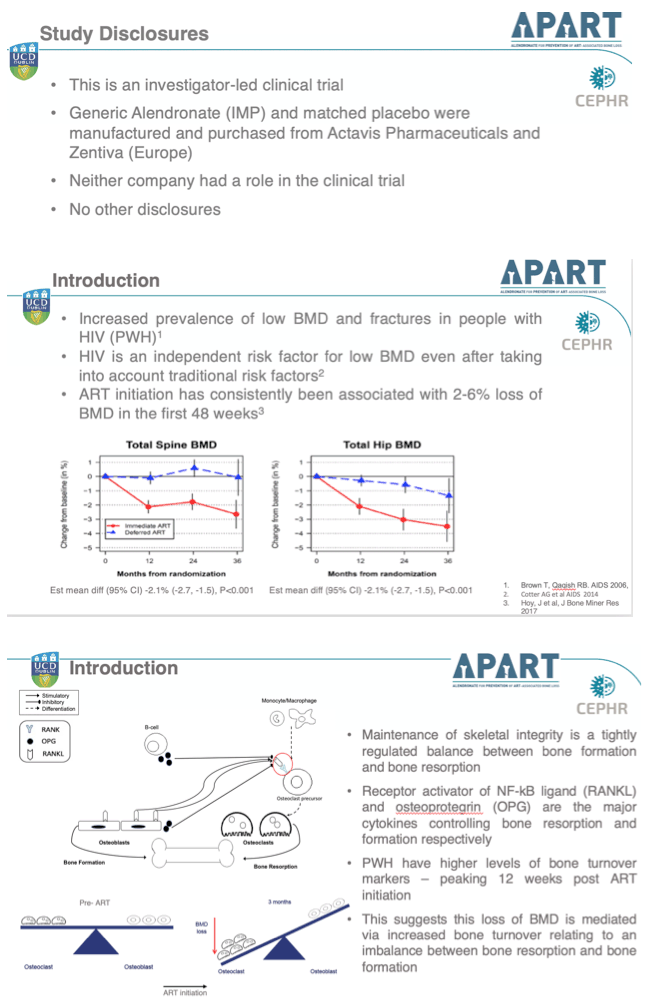
Researchers who ran this investigator-initiated trial, APART, noted that HIV infection boosts the risk of low bone mineral density (BMD) even after accounting for traditional bone-loss risk factors. Trials consistently chart a 2% to 6% BMD loss in the first 48 weeks of ART. Evidence suggests that an imbalance favoring bone loss over bone formation drives osteopenia and osteoporosis in people with HIV.
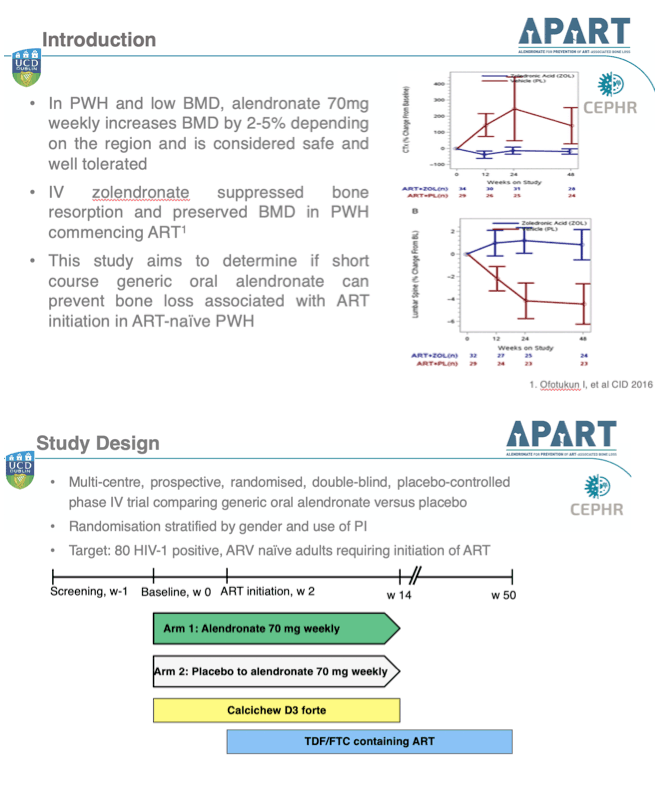
An inhibitor of osteoclast-mediated bone resorption (loss), alendronate is licensed to treat or prevent osteoporosis. A dose of 70 mg weekly boosts BMD 2% to 5% in people with HIV, the investigators said. They mounted this multicenter, double-blind, placebo-controlled trial to assess the impact of generic oral alendronate on BMD in people about to start their first antiretroviral regimen.
Participants had to be men older than 25 or women older than 30. They could not have a history of osteoporosis or fracture, chronic renal failure, hypo- or hypercalcemia, recent significant steroid exposure, or previous treatment with a bisphosphonate (alendronate’s drug class). Women could not be pregnant or breastfeeding. The primary endpoint was between-group difference in percent change in total hip BMD from baseline to week 50 in participants who took at least one dose of study drug.
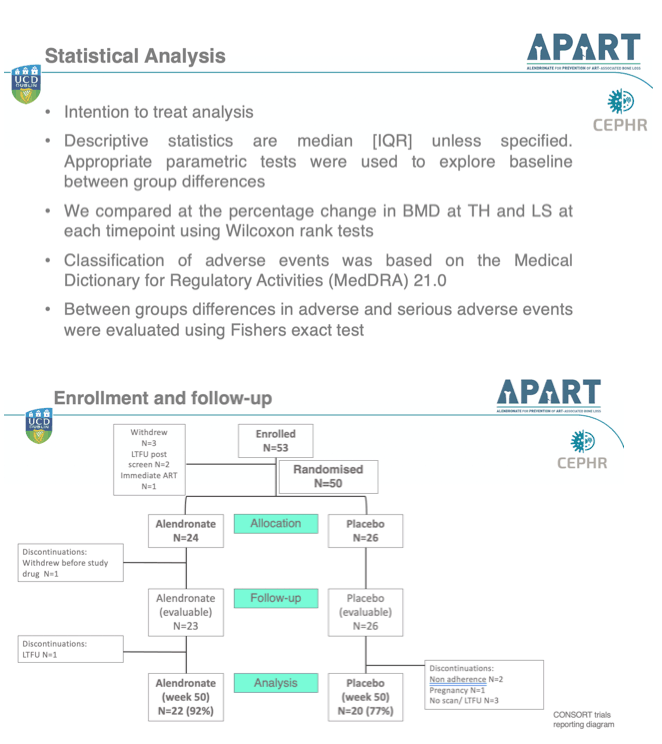
Researchers randomized 24 participants to alendronate (70 mg weekly) and 26 to placebo; all received calcium and vitamin D supplementation (Calcichew D3 forte) for 14 weeks. People took their assigned regimen for 2 weeks, then started an antiretroviral combination containing tenofovir disoproxil fumarate (TDF) and emtricitabine (TDF/FTC). Alendronate or placebo continued for a total 14 weeks.
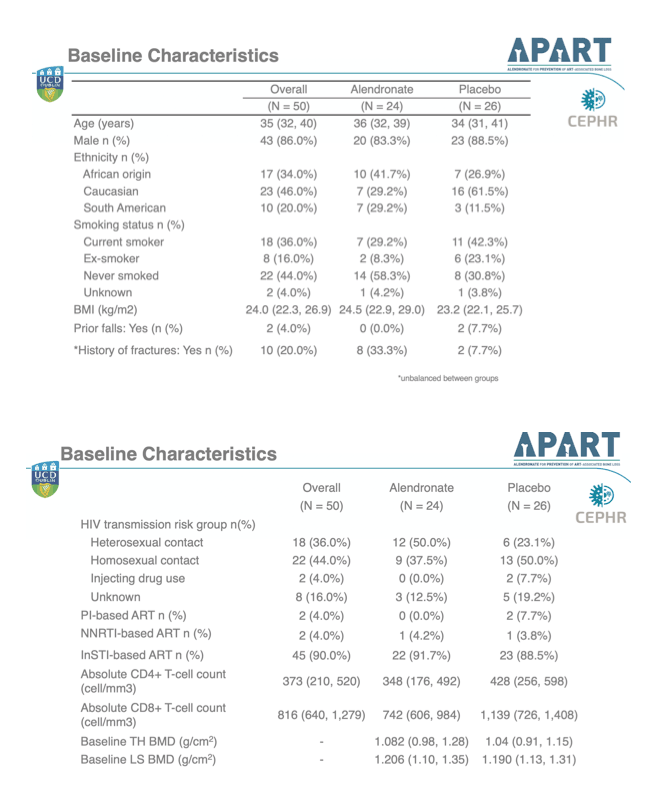
The alendronate and placebo groups were similar in age (median 35 overall), percentage of men (86% overall), and body mass index (24 kg/m2 overall). The alendronate group had a higher proportion of people of African origin (42% vs 27%), a higher proportion with a fracture history (33% vs 8%), and lower proportions of current smokers (29% vs 42%) and ex-smokers (8% vs 23%). Median pretreatment CD4 count stood at 348 in the alendronate group and 428 in the placebo group). Most people (90% overall) took an integrase inhibitor with TDF/FTC.
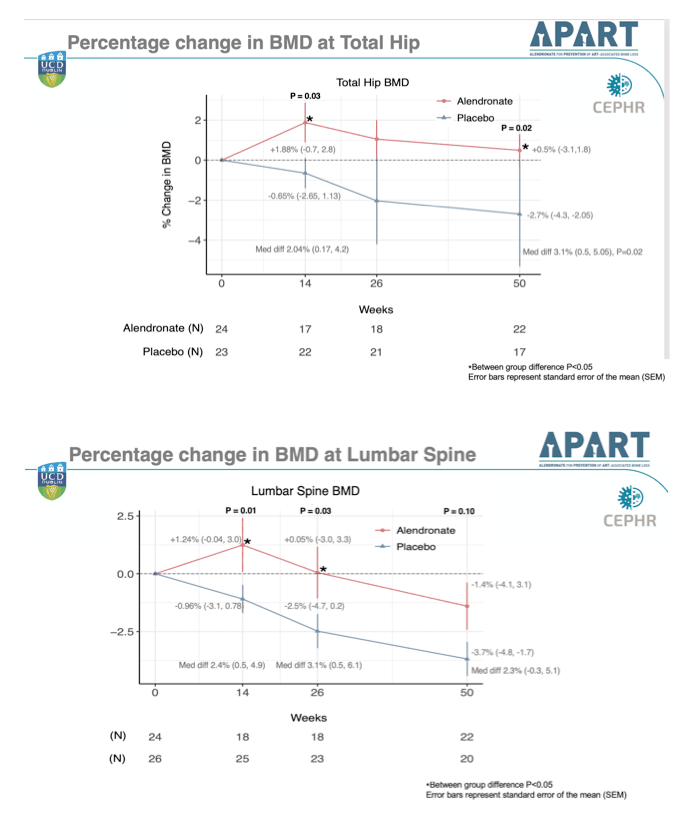
In intention-to-treat analyses, after 14 weeks of alendronate (and 12 weeks of ART), change in total hip BMD averaged +1.88% with alendronate and -0.65% with placebo (median difference 2.04%, P = 0.03). After 50 weeks (48 weeks of ART) change in total hip BMD averaged +0.5% with alendronate and -2.7% with placebo (median difference 3.1%, P = 0.02).
At the lumbar spine week-14 change in BMD averaged +1.24% with alendronate and -0.96% with placebo (median difference 2.4%, P = 0.01). After 50 weeks lumbar spine BMD change averaged -1.4% with alendronate and -3.7% with placebo (median difference 2.3%, not significant, P = 0.10).
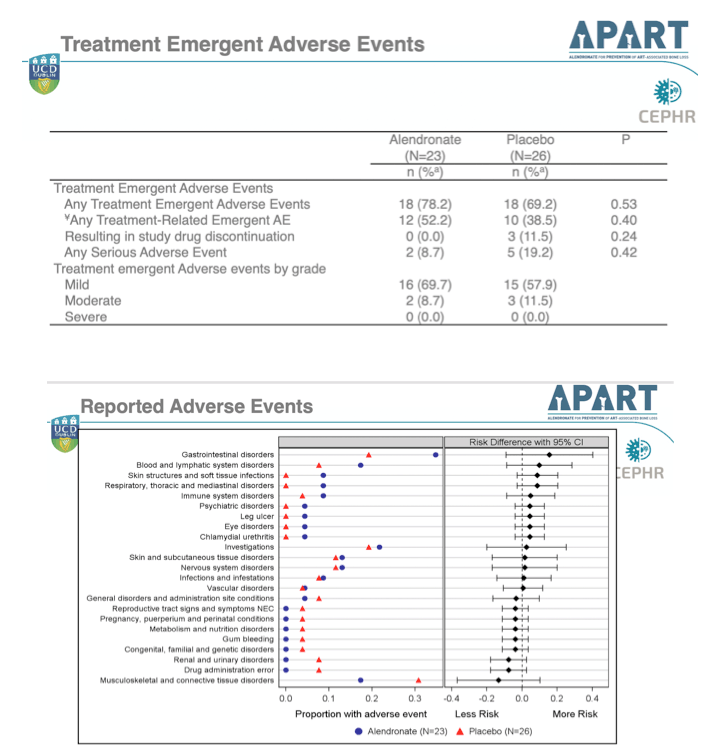
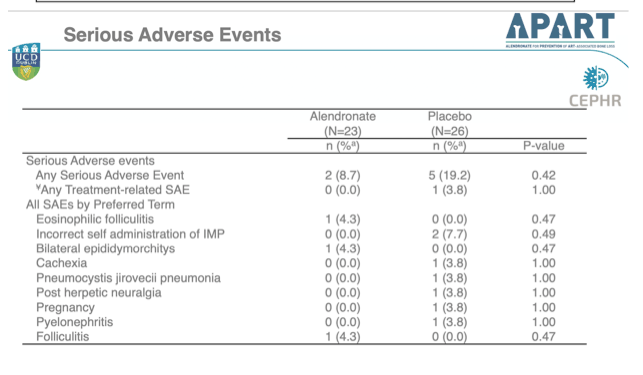
Treatment-related adverse events affected 52.2% taking alendronate and 38.5% taking placebo (not significant, P = 0.40). No one in the alendronate group had a treatment-emergent adverse event that made them drop out of the study, compared with 3 (11.5%) in the placebo group (not significant, P = 0.24). Serious adverse events arose in 8.7% randomized to alendronate and 19.2% randomized to placebo (not significant, P = 0.42). There was 1 treatment-related serious adverse event in the placebo group and none in the alendronate group (not significant).
The researchers noted that their study is limited by its small size and low percentage of women. And the study group was much younger than many HIV populations (median 35 years). The APART investigators concluded that short-course generic alendronate prevents ART-related bone loss through 48 weeks at the total hip and through 24 weeks at the lumbar spine. The investigators added that generic alendronate is cheap, readily available, safe, and well tolerated by people with HIV.
Reference
1. McGinty T, Alvarez-Barco E, Tinago W, et al. Short-course alendronate for the prevention of art-associated bone loss. CROI 2021, Conference on Retroviruses and Opportunistic Infections, March 6-10, 2021. Abstract 96.



|
| |
|
 |
 |
|
|