| |
Prevalence and mapping of hepatitis C infections among men who have sex with men in New York City
|
| |
| |
Dowload the PDF here
July 18, 2018
Overall HCV seroprevalence was 2.8% among community-recruited MSM in NYC, with higher prevalence among HIV-positive MSM compared to HIV-negative MSM. Only two participants were found to have recent HCV infection, with no evidence of a clustered HCV epidemic based on phylogenetic analysis. Our results support testing of HCV infection among HIV-negative MSM if they report having a recent STI and IDU in the past rather than universal HCV testing in all HIV-negative MSM.
This study involving a large sample of community-recruited HIV negative and HIV positive MSM in NYC found an overall HCV seroprevalence of 2.8%. The community-recruited sample had a low prevalence of individuals who reported injecting drugs ever in the past of 5.2%, although they did report sexual risk behaviors that would place them at risk for sexual transmission of HCV, with 14.2% of the MSM reporting any condomless insertive anal sex and 16.8% reporting any condomless receptive anal sex with a male partner in the last 3 months. We found a higher HCV prevalence among HIV-positive MSM compared to HIV-negative MSM (8.1% vs. 1.5%, respectively, p = <0.001), consistent with previously published data showing higher rates of HCV infection among HIV-infected compared to uninfected MSM[13, 15-25]. Of the 29 men who were HCV antibody-positive in our study, only 12 or 41% were HCV RNA-positive, indicating chronic hepatitis C infection. Our HCV seroprevalence of 8.1% (17/209) among HIV-infected MSM is lower than what has been reported in the literature for NYC. In one study, the proportion of HCV infections among HIV-infected individuals in NYC who are MSM dramatically increased from 7% in 2000 to 24% in 2010[64]. In another NYC study from 1999-2007, 10.5% of HCV and HIV co-infected individuals were found to be non-IDU MSM; this study had an older sample of individuals with mean age of 50.4 years[65]. These rates are markedly higher than those reported in other U.S. cities, including San Francisco where HCV prevalence among non-IDU HIV-positive MSM decreased from 9% in 2004 to 2% in 2011[66, 67].
In multivariate analyses in our study, we found that HCV antibody seropositivity was significantly associated having reported any STI in the last 3 months, along with older age, IDU ever history, and HIV-positive serostatus. In contrast to other studies, methamphetamine use was not significantly associated with HCV seropositivity. This may be due to a Type II error given the low number of HCV antibody-positive participants found in our study. In a study comparing prevalence of HCV infection among IDU MSM and non-IDU MSM in the Multicenter AIDS Cohort Study, HCV antibody seroprevalence among IDU MSM was 42.9%, significantly higher than 4.0% among non-IDU MSM; in addition, HCV clearance was lower among IDU MSM compared to non-IDU MSM. In both IDU and non-IDU MSM, HIV infection, older age, and Black race were associated with higher HCV antibody seroprevalence.
Abstract
Emerging sexually transmitted hepatitis C virus (HCV) epidemics among men who have sex with men (MSM) have been reported worldwide, with higher HCV infection rates among those who are HIV-infected. This study aims to determine prevalence of recent and chronic HCV infections among community-recruited MSM in New York City (NYC), map HCV infections by home, social, and sexual neighborhoods, and identify clusters of genetically linked HCV variants using phylogenetic analysis.
The NYC M2M study recruited MSM via modified time-space, venue-based sampling and internet/mobile app-based recruitment during 2010-13. Participants completed a Google Earth map on neighborhoods of where they lived, socialized, and had sex in the last 3 months, an ACASI questionnaire, and a sexual network inventory about their sex partners. The men received HIV testing and provided serum samples. Testing on stored serum samples included HCV antibody and RNA viral load, HCV antibody avidity assay (avidity index <30% with positive viral load is considered recently infected), and HCV RNA extraction and amplification to generate a 432 base-pair region of Core/E1 for sequencing and phylogenetic analysis. Historic local controls were included in the phylogenetic analysis.
Of 1,028 MSM, 79.7% were HIV-negative and 20.3% HIV-positive. Twenty nine MSM (2.8%) were HCV antibody-positive.
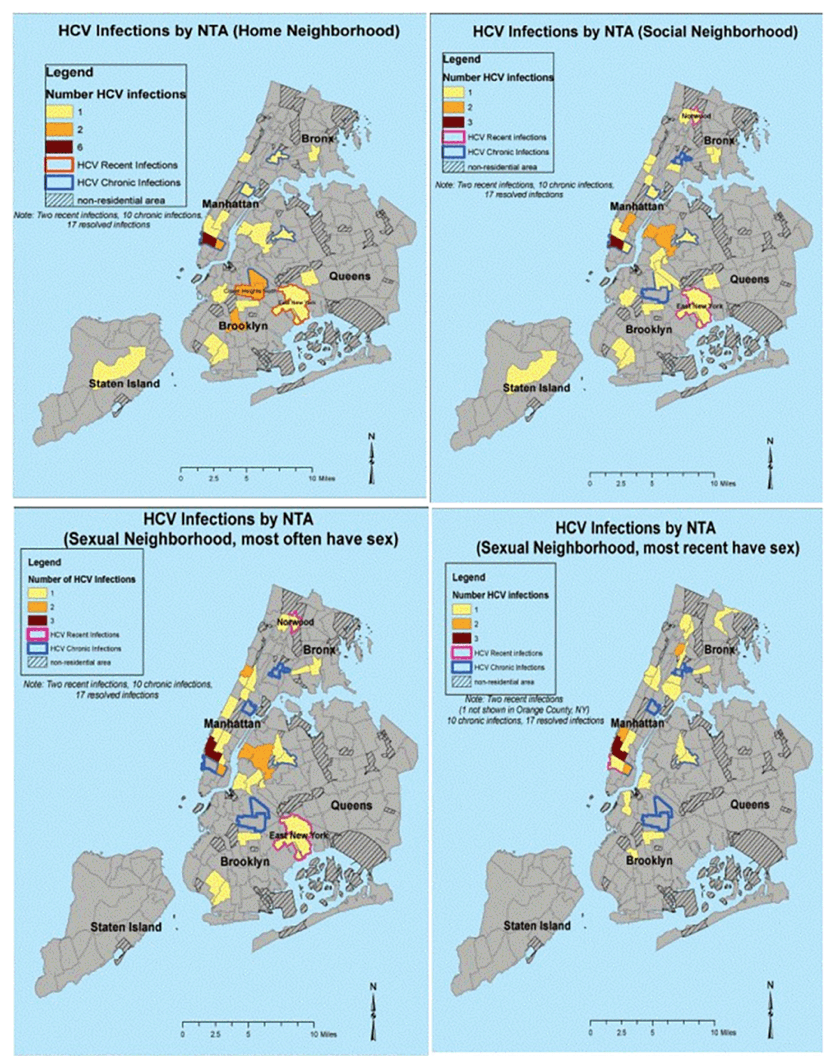
MSM who were HCV antibody-positive reported a median of 2 male sex partners in last 3 months, with 6.9% aged 18-24, 17.2% 25-29, 13.8% 30-39, and 62.1% 40 and over. 8.1% of HIV-positive MSM were HCV antibody-positive vs. 1.5% of HIV-negative men (p<0.0001). Of 29 HCV-antibody positive MSM, 12 (41%) were HCV RNA-positive (11 subtype 1a and 1 subtype 1b). Two of 12 HCV RNA-positive participants had low antibody avidity values, suggesting recent HCV infection. HCV antibody seropositivity was significantly associated with older age >40 years, adjusted odds ratio (aOR) 3.56 (95% CI 1.57, 8.08), HIV-positive serostatus, aOR 3.18 (95% CI 1.40, 7.22), any sexually transmitted infection (STI) in the last 3 months, aOR 2.81 (95% CI 1.11, 7.13), and injection drug use (IDU) ever, aOR 4.34 (95% CI 1.69, 11.17). Mapping of HCV infections differed slightly by home, social, and sexual neighborhoods. Based on phylogenetic analysis from 12 HCV RNA-positive samples, no evidence of a clustered HCV epidemic was found. Overall HCV seroprevalence was 2.8% among community-recruited MSM in NYC, with higher prevalence among HIV-positive MSM compared to HIV-negative MSM. Only two participants were found to have recent HCV infection, with no evidence of a clustered HCV epidemic based on phylogenetic analysis. Our results support testing of HCV infection among HIV-negative MSM if they report having a recent STI and IDU in the past rather than universal HCV testing in all HIV-negative MSM.
Introduction
Although primary transmission of hepatitis C virus (HCV) is through the parenteral route[1], epidemics of sexually transmitted HCV infection among men who have sex with men (MSM) have been reported in Europe, Australia, Asia, and North America, with blood remaining the likely medium for sexual transmission of HCV in these outbreaks[2-14]. These sexually transmitted HCV outbreaks have mostly involved HIV-infected MSM, with lower HCV infection rates in HIV-negative MSM[13, 15-26]. Many studies have also reported strong associations between HCV infection risk and sexual risk behaviors, including high number of sexual partners[10, 27], condomless anal sex[10, 11, 17, 27], recreational drug use during sex[10, 11], and traumatic sexual practices such as fisting[10, 27, 28]. In the Multicenter AIDS Cohort Study (MACS) study of HCV infections among HIV positive and HIV negative MSM in four U.S. metropolitan areas from 1984-2011, 115 cases of incident HCV infection were reported (incidence rate of 2.08/1,000 person-years [PYs]). In multivariate analysis, condomless receptive anal sex with more than one male partner, older age, HIV infection, heavy alcohol use, hepatitis B surface antigen positivity, and syphilis infection were significantly associated with incident HCV infection[17]. High rates of HCV reinfection of up to 15/100 PYs have been reported among HIV-infected MSM who had previously received successful HCV treatment or had spontaneously cleared their HCV infections[29-32].
Untreated HCV infection leads to chronic hepatitis in 60-80% of cases. Spontaneous clearance of HCV without treatment is seen in approximately 25% of exposed individuals in the first 6 months. Serious complications of chronic hepatitis include liver cirrhosis and hepatocellular carcinoma[1, 33-37]. With the introduction of new, oral direct acting antiviral drugs, treatment success rates for chronic HCV infection have improved markedly[38-40]. Interferon-based HCV treatment early after diagnosis is associated with higher rates of sustained virologic response compared to delayed treatment of chronic HCV infection[41-44], with the use of direct acting antiviral drugs under investigation for recent HCV infection. Early treatment has public health implications by potentially decreasing the risk of onward sexual and parenteral transmission of HCV to partners. Cost-effectiveness studies show that early HCV treatment after diagnosis maximizes medical costs savings and gains in quality-adjusted life years[45-47].
Given the benefits of early compared to late HCV treatment, accurate diagnosis of recent HCV infection is important. Clinical diagnosis of recent HCV infection can be challenging since newly infected individuals are frequently asymptomatic[48]. Diagnosis can also be delayed and problematic, as it can be difficult to distinguish between acute, resolved, and chronic infections when using immunoglobulin M (IgM) anti-HCV testing[48, 49].HCV antibody avidity assays are research tools that measure the binding strength of anti-HCV antibodies in infected individuals. These assays can be used in research to distinguish recent infection from chronic and resolved HCV infections[48, 50-56]. HCV antibody avidity increases gradually over the course of HCV infection: antibodies produced early in infection have weak antigen-binding ability while mature antibodies generated later in infection have strong antigen-binding capacity. HCV antibody avidity assays can provide advantages over traditional laboratory diagnosis of recent HCV infection and can be important for estimating HCV incidence using cross-sectional research data[55].
This study aims to determine prevalence of recent and chronic HCV infections among community-recruited MSM in New York City (NYC) by using HCV antibody avidity assays, determine sociodemographic and risk behavior characteristics that are associated with HCV infection, map HCV infections by home, social, and sexual neighborhoods, and identify clusters of genetically linked HCV variants using phylogenetic analysis. This study is based on the NYC M2M study (NIH R01 HD059729, PI: Koblin), a cross-sectional study conducted between 2010-2013 to identify urban environment characteristics that influence sexual risk behaviors, substance use, and depression among 1,458 MSM in NYC[57-61].
| |
| |
| |
|
|
|