 |
 |
 |
| |
Clinical characteristics and prognostic
factors in people living with HIV
hospitalized with COVID-19: findings
from the WHO Global Clinical Platform
|
| |
| |
IAS 2021 July 18-22
S. Bertagnolio 1, S.S. Thwin 2, R. Silva 2, N. Ford 1, R. Baggaley 1, M. Vitoria 1, W. Jassat 3, M. Doherty 1, J. Diaz 4
1
World Health Organization, Department of HIV, Hepatitis and STI Programmes, Geneva, Switzerland, 2Word Health Organization, Sexual and Reproductive Health and Research, Geneva, Switzerland, 3National Institute for Communicable Diseases (NICO), National Health Laboratory Service (NHLS), Johannesburg, South Africa, 4World Heath Organization, Department of Country Readiness Strengthening, Geneva, Switzerland
--------------------------------------
WHO warns that HIV infection increases risk of severe and critical COVID-19 - (07/15/21)
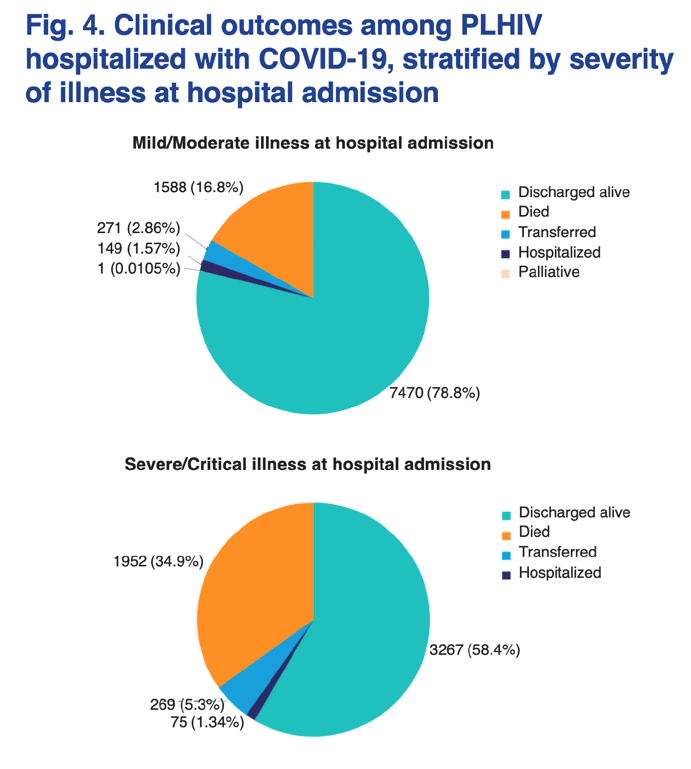
A sensitivity analysis was repeated to assess the impact of the country of origin on the severity outcome. After excluding data from South Africa, a total of 38 774 cases were available. Of those, 840 were people living with HIV, and 425 had information on severity status. In this analysis, HIV positive status remained an independent risk factor for severe/critical illness at hospital admission (aOR 2.27, 95% CI 1.73-2.97) after adjusting for age, sex and the presence of underlying conditions (diabetes, neoplasms and chronic cardiac disease).
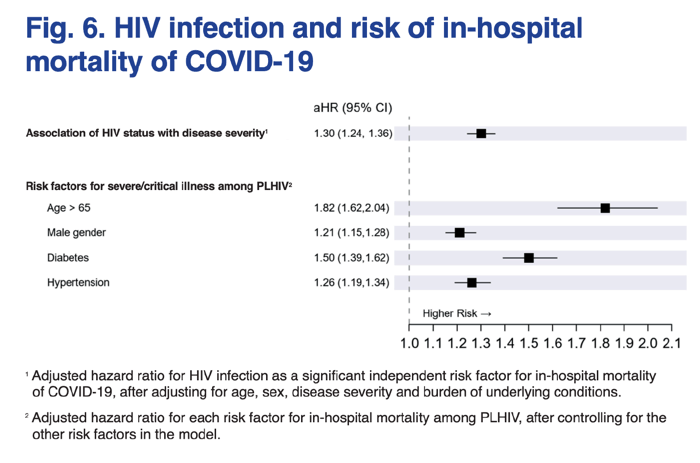
We performed a subgroup analysis, stratifying mortality risk by WHO geographic region. After adjusting for age, sex, underlying conditions and clinical presentation at hospital admission (mild/moderate versus severe/critical illness), HIV infection was independently associated with an increased risk for in-hospital mortality in the WHO African Region (aHR 1.29, 95% CI 1.23-1.34) but not in the WHO European Region (aHR 0.59, 95% CI 0.29-1.2) or the WHO Region of the Americas (aHR 0.92, 95% CI 0.37-2.31). For other Regions, modelling for mortality outcomes was not possible due to the limited sample size. A sensitivity analysis was repeated to assess the impact of the country of origin on the mortality. When excluding data received from South Africa (resulting in a total of 311 HIV positive cases compared with 7474 HIV negat ive cases with a known outcome), the risk of death in people living with HIV hospitalized with COVID-19 remained elevated, but was no longer statistically significant (aHR 1.16, 95% CI 0.90-1.51). Adjustment for covariates other than sex and age was not possible due to the limited sample size.
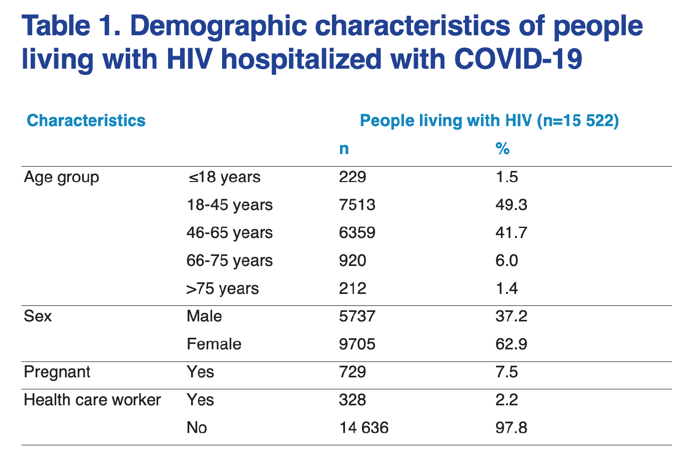
In this analysis, the data are predominantly from South Africa. Although this may limit the generalizability of the results, it is worth noting that this country is the epicenter of the HIV pandemic and has the largest AIDS epidemic globally, accounting for 20% of all people living with HIV worldwide and 20% of new HIV infections.
Not all potentially relevant risk factors, such as body mass index (BMI), were considered in the regression model due to insufficient data reported; and this may have influenced our findings. In addition, findings only refer to in-hospital mortality and do not capture information on post-discharge outcomes, thus potentially underestimating the impact of HIV infection on overall mortality due to COVID-19.
---------------------------------------------





|
| |
|
 |
 |
|
|