 |
 |
 |
| |
HIV-1 RNA TRANSCRIPTS IN CSF CD4+ T CELLS,
NOT MONOCYTES, ARE LINKED TO BRAIN INJURY
|
| |
| |
CROI 2022 Feb 11-16
John Zaunders
St Vincent's Hospital, Sydney, Australia

What is HIV transcription?
HIV's genes are RNA while the genes inside human cells are DNA. So, in order for the virus to infect the cell, a process called "reverse transcription" makes a DNA copy of the HIV's RNA. This is done with one of HIV's enzymes called reverse transcriptase. The new HIV DNA is also called "proviral DNA."
When HIV RNA enters the cell it must be 'reverse transcribed' into proviral DNA before it can be integrated into the DNA of the host cell. HIV uses its reverse transcriptase enzyme to convert RNA into proviral DNA inside the cell.

program abstract
Abstract Type:
Kazuo Suzuki1, John Zaunders1, Thomas Gates1, Angelique Levert1, Shannen Butterly1, Zhixin Liu2, Takaomi Ishida3, Chin-Shiou Huang4, Caroline Rae5, Lauriane Jugé5, Lucette A. Cysique6, Bruce Brew1
1St Vincent's Hospital, Sydney, Australia, 2University of New South Wales, Randwick, Australia, 3DENKA Life Innovation Research Institute, Tokyo, Japan, 4PlexBio Research Development, Taipei, Taiwan, 5Neuroscience Research Australia, Randwick, Australia, 6University of New South Wales, Sydney, Australia
Background:
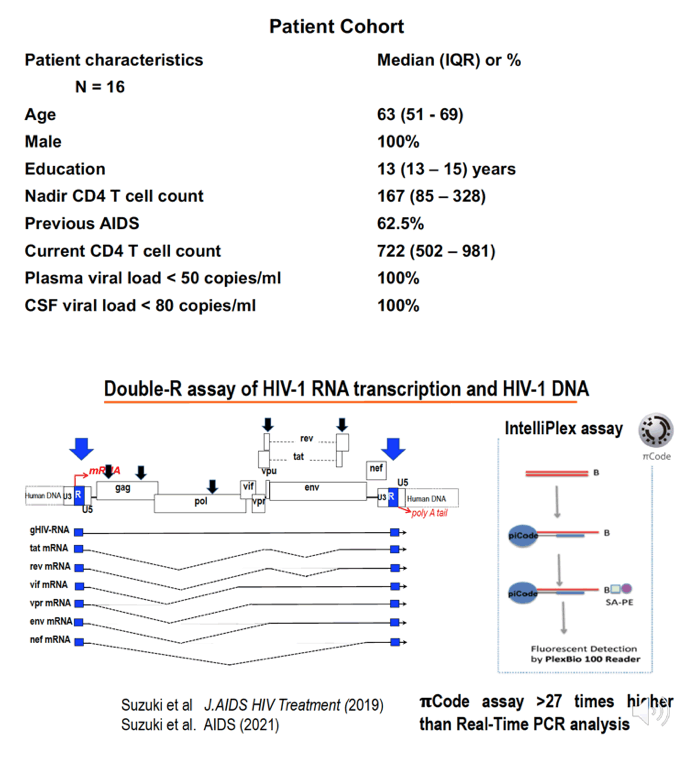
Brain injury is prevalent in people with HIV-1 (PWH), despite suppressive ART. Our previous findings, using the highly sensitive Double-R assay, that high levels of cell-associated (CA) HIV-1 RNA transcripts in CSF cells correlated with current neuronal dysfunction, suggesting an active causal link. Monocytes (Mφ) are widely considered the principal Trojan Horse by which HIV-1 enters and establishes brain infection. We hypothesized that Mφ would be the chief source of transcripts.
Methods:
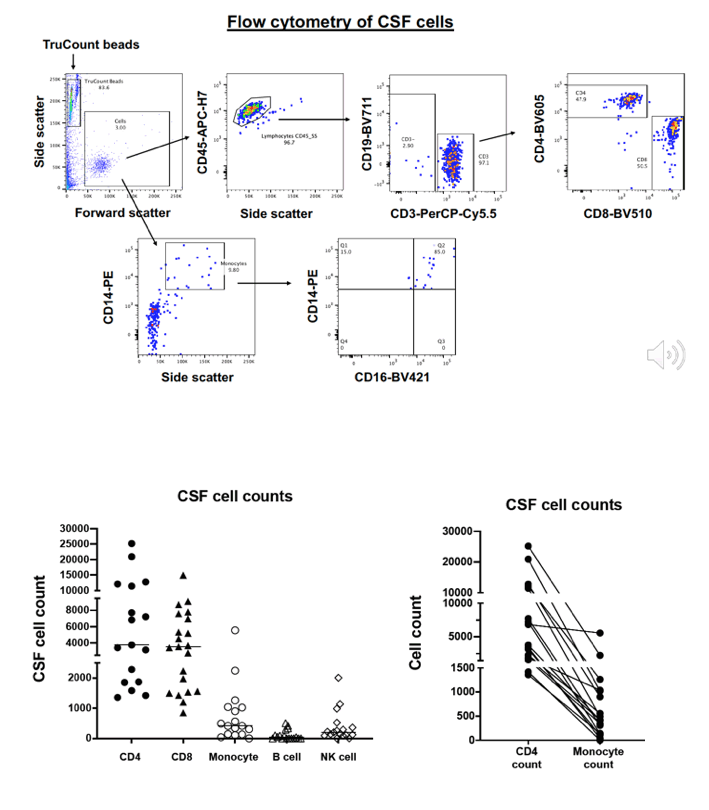
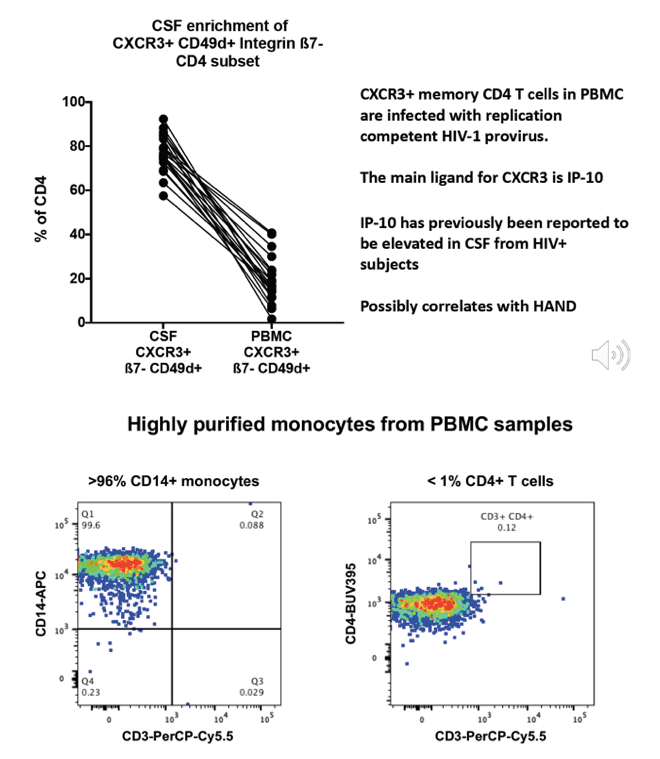
CSF cells and PBMC from 16 PWH on fully suppressive ART were analyzed and accurately counted by 18-colour flow cytometry. Mφ were highly purified from PBMC using magnetic beads and contained a median 0.3% contaminating CD4+ T cells. DNA and RNA were extracted from the samples of pelleted CSF cells, PBMC and purified blood Mφ. CA HIV-1 RNA and DNA were determined by the Double-R πCode MicroDiscs assay, as copies/106 cells. In vivo brain injury was assessed with 1H MR spectroscopy.
Results:
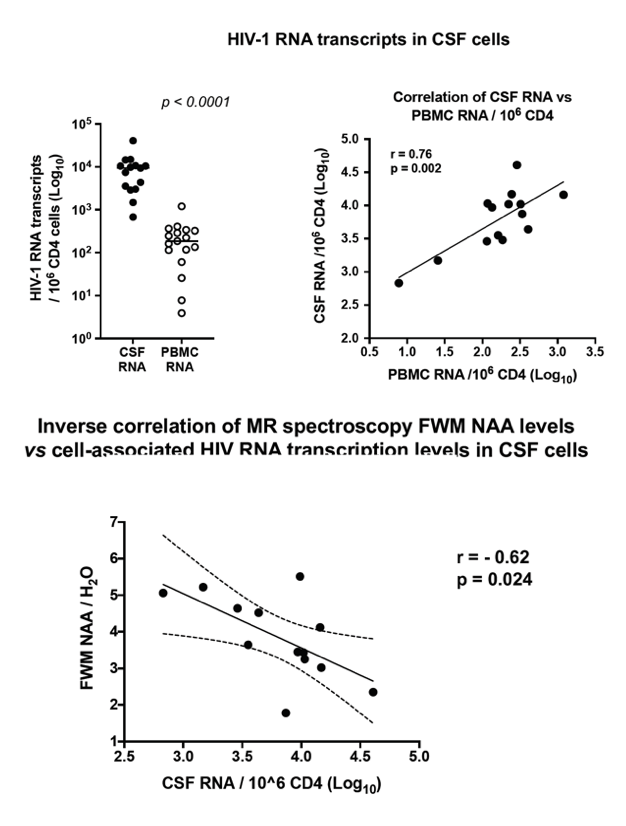
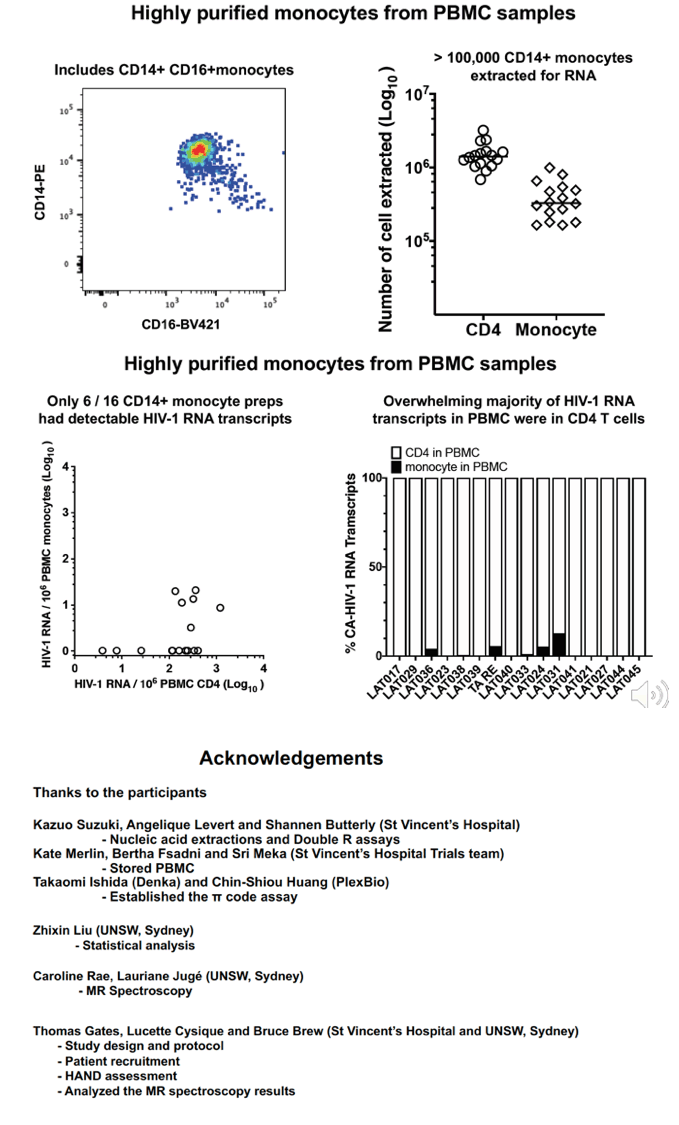
Pelleted CSF cells were 91% memory T cells, including median 3,605 CD4+ and 3,632 CD8 T cells, but only 378 Mφ (>90% intermediate CD14+CD16+ phenotype). 14/16 and 13/16 samples of CSF cell samples had detectable CA HIV-1 RNA and HIV DNA. CA HIV-1 RNA transcripts in CSF numbered 9,226 copies/106 CD4+ T cells, compared to 185 copies/106 CD4+ T cells from PBMC. Importantly, CA HIV-1 RNA levels in CSF cells strongly correlated with their paired PBMC levels (r=0.83; p=0.003; Fig 1A). In contrast, even with >105 highly purified Mφ from PBMC, only 6/16 samples contained detectable CA HIV-1 RNA transcripts, with a median of only 9 copies/106 Mφ vs 306 copies/106 CD4+ T cells from the same PBMC samples, such that the contribution of Mφ transcripts to PBMC was very minor (Fig1B). In CSF, CD4+ T cells were highly enriched with susceptible memory CXCR3+ CD49d+ integrinß7- cells (76% in CSF vs 18% in PBMC), CCR5+ cells (51% vs 28% in PBMC) and activated CD38+ and/or HLA-DR+ cells (18% vs 10%). Higher levels of CSF CA HIV-1 RNA transcripts were associated with greater brain injury in the FWM (Std β=-0.73; p<0.01) and PCC (Std β=-0.61; p<0.05).
Conclusion:
Our results fundamentally challenge the monocyte-centered pathogenetic model of NeuroHIV in virally suppressed patients. Our results suggest a model where the residual infected memory CD4+ T cells in blood seed the brain through trafficking, with subsequent involvement of longer-lived resident brain macrophage lineage cells.
|
| |
|
 |
 |
|
|