 |
 |
 |
| |
IMPACT OF SVR WITH DAAs IN COINFECTED PATIENTS WITH ADVANCED FIBROSIS/CIRRHOSIS
|
| |
| |
CROI 2022
Teresa Aldamiz-Echevarría1, Juan Berenguer1, Víctor Hontañon2, Chiara Fanciulli1, Carmen Quereda3, Carmen Busca2, Lourdes Domínguez4, Cristina Hernandez5, Jorge Vergas6, Gabriel Gaspar7, Lucio J García-Fraile8, Marta De Miguel 9, Jose M Bellon1, Juan Gonzalez-García2 and GeSIDA 10318-Marathon Study Team.
1Hospital General Universitario Gregorio Marañon, Madrid. 2Hospital Universitario La Paz, Madrid. 3Hospital Universitario Ramon y Cajal, Madrid. 4Hospital Universitario 12 de Octubre, Madrid. 5Hospital Universitario Príncipe de Asturias, Alcala de Henares. 6Hospital Clínico de San Carlos, Madrid. 7Hospital Universitario de Getafe, Getafe. 8Hospital Universitario de la Princesa, Madrid. 9Fundacion SEIMC-GeSIDA, Madrid.

program abstract
Background:
Direct-acting antivirals (DAAs) are highly successful in HIV/HCV-coinfected patients with advanced fibrosis (F3) or cirrhosis (F4), but little is known about their impact on clinical events.
Methods:
We studied coinfected patients with F3/F4 with a sustained viral response (SVR) following all-oral DAA-Rx (Rx) from 2014 to 2017 in observational GeSIDA cohorts (Spain). The censoring date was December 31, 2019. The primary outcome was time from the finalization of DAA-Rx to clinical progression (CP), defined as decompensation (DEC), hepatocellular carcinoma (HCC), or death, whichever occurred first. Variables included liver disease category (F3, compensated F4 [F4c], and decompensated F4 [F4d]), age, sex, current smoking, current high alcohol intake (>50 g/d), prior AIDS-defining conditions, metabolic syndrome (AHA/NHLBI criteria), CD4+ cell count, serum albumin, liver stiffness (LS), FIB4 index, triglyceride and glucose index (TyG), hepatic steatosis index (HIS); and % decrease in LS (D-LS) and % decrease in FIB4 (D-FIB4) 1 year after finalization of DAA-Rx. Multivariable Cox regression analysis, with multiple imputations by chained equations for missing data, was used to assess the effect of the independent variables on the outcome.
Results:
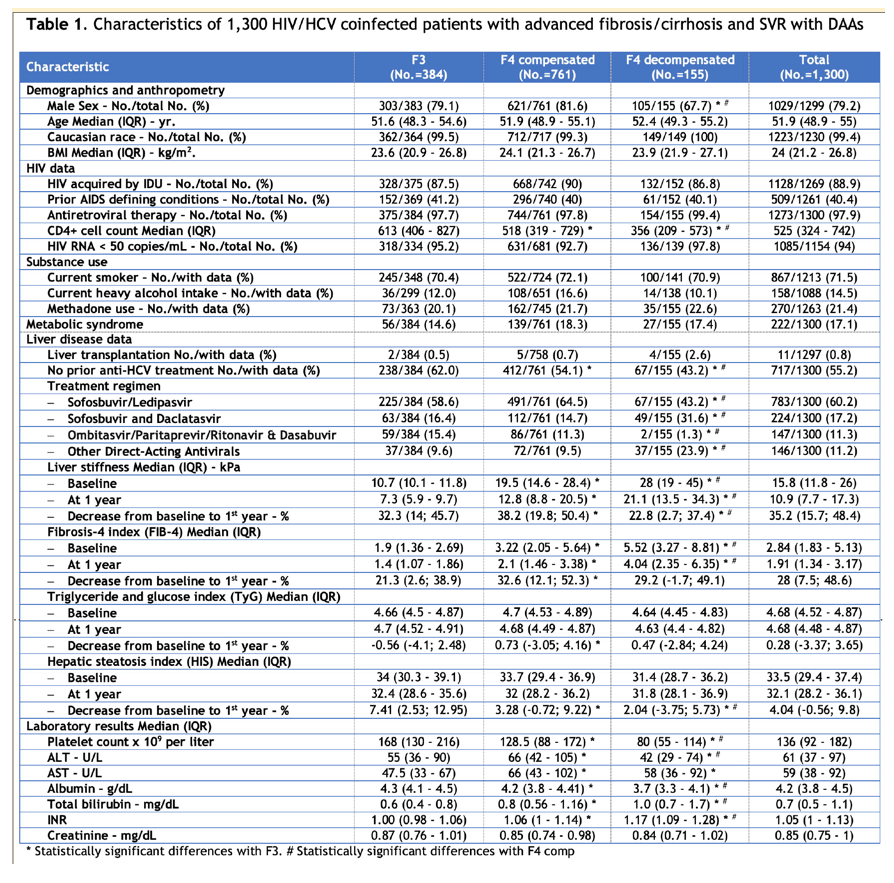
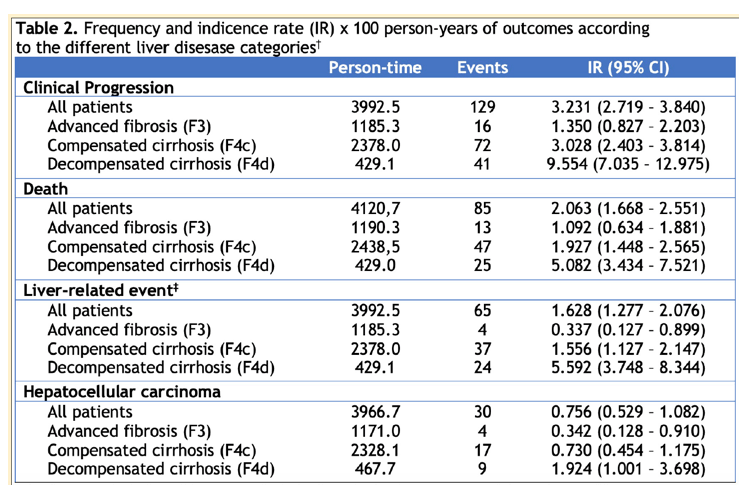
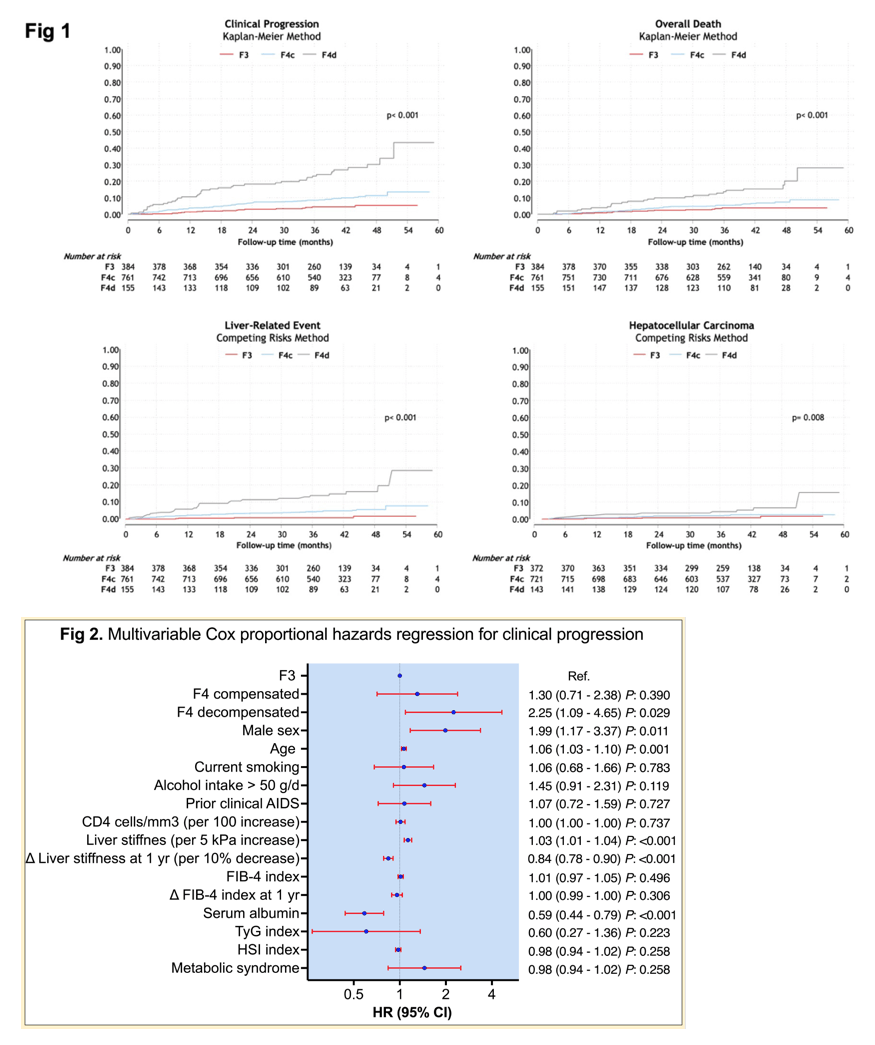
A total of 1300 patients were included with a median age of 52 years; 79% males; 87% prior injection drug use; 98% on ART; 94% with undetectable HIV-RNA; median CD4+ 525 cells/mm3. Liver disease: 384 (30%) F3, 761 (59%) F4c, and 155 (12%) F4d. After a median follow-up of 40.9 (34.5 - 45.1) months, 89 patients were lost, 85 died, 65 had a new LRE (DEC or HCC), and 30 were diagnosed with HCC. The frequency and indicence rate of outcomes by liver disesase category is shown in the Table. The following variables were found to be independently associated with CP: F4d (vs F3) (adjusted hazard ratio [aHR] 2.25; 95%CI 1.09-4.65, P=.029), male sex (aHR 1.99; 95%CI 1.17-3.37, P=.011), age (aHR 1.06; 95%CI 1.03-1.10, P=.001), LS (aHR 1.03; 95%CI 1.01-1.04, P<.001), D-LS (aHR 0.98; 95%CI 0.98-0.99, P<.001), and serum albumin (aHR 0.59; 95%CI 0.44-0.79, P<.001).
Conclusion:
Our results suggest that among coinfected patients with well-controlled HIV and with advanced F3/F4, the risk of CP following DAA-induced SVR increased with liver disease severity at the beginning of therapy and with a lower decrease in LS one year after its finalization. Further work should be done to develop prediction scores to inform clinical decision-making in this population group

|
| |
|
 |
 |
|
|