| |
Durable virological response and functional cure of chronic hepatitis D after long-term peginterferon therapy - treatment duration 8-14 years
|
| |
| |
Download the PDF here
28 May 2021 Julian Hercun1| Grace E. Kim1| Ben L. Da1| Yaron Rotman1| David E. Kleiner2|Richard Chang3| Jeffrey S. Glenn4| Jay H. Hoofnagle5| Christopher Koh1|Theo Heller1
We demonstrate that in a selected group of patients and with close dose monitoring and adjustment, therapy can be tolerated and a durable virological response can be maintained for more than 4 years on average without relapse.
No liver-related deaths occurred in responders, even though their baseline characteristics and severity of liver disease were similar to non-responders. Thus, a durable response to treatment in HDV appears to change the natural history of the disease. Furthermore, non-response to peginterferon was associated with increased overall non-liver-related mortality. This finding is in line with previous reports on overall mortality in chronic hepatitis C virus infection treated with peginterferon.14 Achieving treatment response with peginterferon in viral hepatitis can potentially influence chronic inflammatory states and therefore reduce all-cause mortality.15
Achieving HBsAg loss, or functional cure, in HDV on treatment has been associated with a favourable prognosis. This outcome has been shown to be the best indicator of remaining HDV RNA negative.3, 11 In addition, seroconversion is the ultimate goal (albeit infrequently reached) in HBV and remains the ultimate goal in HDV therapy. Patients who develop HBsAg loss remain protected from relapse in the future. Extending therapy with the use of HBsAg titres in order to achieve functional cure has previously been suggested.16, 17 In this same group of subjects, the slope of decline in HBsAg titres paralleled the slope of the second phase of HDV RNA decline and responders demonstrated a faster HBsAg titre decline.17 In the future, the use of novel markers, such as HBV RNA, can potentially be useful in the assessment of viral kinetics and response to therapy.
The major shortcoming of this study was the limited number of subjects in this case series, but the small scale of study was partially compensated by the rigorous and long-term follow-up.
The search for a cure for delta hepatitis remains elusive, with unsatisfactory response to current available and experimental therapies. In this prospective follow-up of a series of patients treated with long-term peginterferon, treatment response occurred and was sustained with the use of HBsAg status to guide continuation or discontinuation of treatment. This study builds on previous findings of treatment response to long-term therapy and demonstrates benefits from tailored extension of treatment.
Summary
Background
Hepatitis delta virus (HDV) infection is the most aggressive form of chronic viral hepatitis. Response rates to therapy with 1- to 2-year courses of pegylated interferon alpha (peginterferon) treatment are suboptimal.
Aims
To evaluate the long-term outcomes of patients with chronic hepatitis D after an extended course of peginterferon.
Methods
Patients were followed after completion of trial NCT00023322 and classified based on virological response defined as loss of detectable serum HDV RNA at last follow-up. During extended follow-up, survival and liver-related events were recorded.
Results
All 12 patients who received more than 6 months of peginterferon in the original study were included in this analysis. The cohort was mostly white (83%) and male (92%) and ranged in age from 18 to 58 years (mean = 42.6). Most patients had advanced but compensated liver disease at baseline, a median HBV DNA level of 536 IU per mL and median HDV RNA level of 6.86 log10 genome equivalents per mL. The treatment duration averaged 6.1 years (range 0.8-14.3) with a total follow-up of 8.8 years (range 1.7-17.6). At last follow-up, seven (58%) patients had durable undetectable HDV RNA in serum, and four (33%) cleared HBsAg. Overall, one of seven (14%) responders died or had a liver-related event vs four of five (80%) non-responders.
Conclusions
With further follow-up, an extended course of peginterferon therapy was found to result in sustained clearance of HDV RNA and favourable clinical outcomes in more than half of patients and loss of HBsAg in a third.
1 INTRODUCTION
Chronic hepatitis delta virus (HDV) infection represents the most severe form of chronic viral hepatitis and has an estimated worldwide prevalence of 12-20 million persons.1, 2 HDV is a small, incomplete RNA virus which requires hepatitis B virus (HBV) co-infection for sustained replication and transmissibility.1 Patients with chronic HDV-HBV co-infection have a more aggressive hepatitis, progress to cirrhosis faster, and are at higher risk for HCC than patients with HBV alone. Unfortunately, therapies for chronic hepatitis D are suboptimal and the agents that are effective in chronic hepatitis B have little effect on disease progression in HDV-HBV co-infection. The only widely available therapy for chronic HDV infection is interferon alpha and its pegylated form, pegylated interferon alpha (peginterferon), but interferon is poorly tolerated, and response rates are low even with extended courses of 1-2 years. Non-response to treatment is common and patients with an on-treatment response usually relapse when therapy is stopped. An open label trial evaluating response rates to extended (3-5 years) therapy of peginterferon was conducted at the Clinical Center of the National Institutes of Health (NIH) (NCT00023322). In that study, 39% of patients achieved an endpoint of histological improvement or viral response at 3 years.3 In this report, we present the long-term follow-up of these patients 10 years after completion of the original protocol.
RESULTS
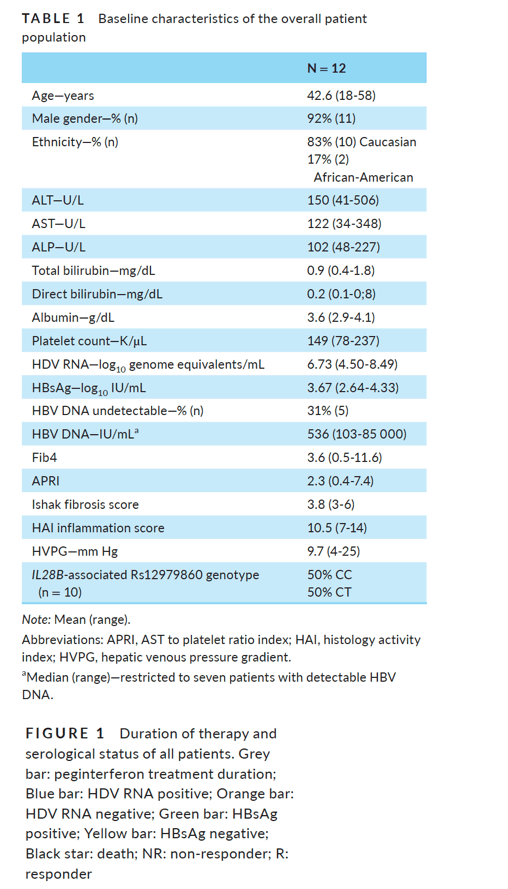
Twelve patients, from the original protocol of thirteen patients, completed at least 6 months of peginterferon therapy and were included in this analysis. Baseline characteristics at enrolment are summarised in Table 1. Patients were mostly Caucasian and male, with a mean age of 42.6 years at treatment initiation. All patients had fairly advanced but compensated liver disease at baseline with a mean Ishak fibrosis score of 3.8 (range 3-6) and HAI scores of 10.5 (range 7-14). Measurement of hepatic vein pressure gradient was performed in all 12 patients and averaged 9.7 mm Hg (range 4-25). Routine liver tests showed mean total bilirubin of 0.9 mg/dL, ALT 150 U/L, AST 122 U/L and alkaline phosphatase 102 U/L. Serum albumin averaged 3.6 g/dL and platelet count 149 K/µL.
The median HDV RNA was 7 300 000 GE/mL (6.86 log10 GE/mL). Five patients (42%) had undetectable or below the lower limit of quantification HBV DNA, and the median HBV viral load in those with quantifiable levels was 536 (range 103-85 000) IU/mL. HBeAg was detected in three patients and anti-HBe without HBeAg in nine patients. All patients were positive for HBsAg and levels averaged 3.7 log10 IU/mL (range 2.6-4.3).
Overall, the mean duration of therapy was 6.1 years (range 0.8-14.3) and follow-up after stopping therapy 5.5 years (0-15.3). Thus, the average total duration of treatment and follow-up was 8.8 years (range 1.7-17.6). Following the end of the clinical trial, five patients were treated for longer than the protocol defined duration of 5 years, under compassionate use for up to nine additional years.
Treatment response
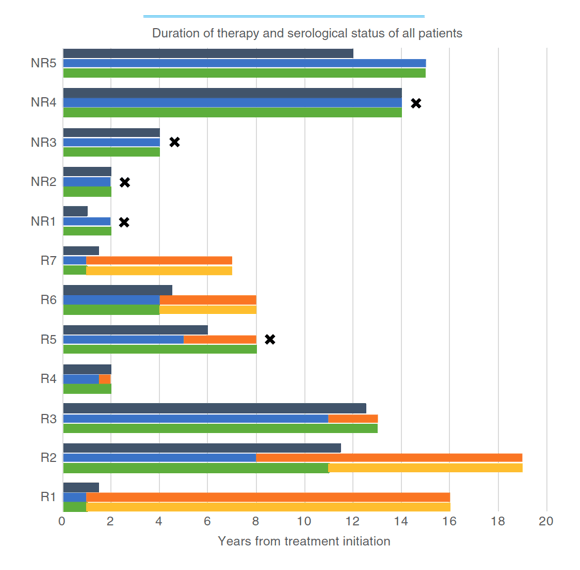
The timing of therapy, HDV RNA results and HBsAg status of the seven responders (R) and the five non-responders (NR) are shown graphically in Figure 1. At last available follow-up, seven (58%) patients had no detectable HDV RNA in serum. While this endpoint was achieved in five patients during the original protocol, two patients benefited from extension of treatment beyond 5 years and did not achieve a full virological response until after 8 and 11 years of therapy. No patients required a resumption of therapy once it was discontinued. Patients with virological response were followed for 54 months on average after treatment discontinuation (range 0-198).
Four patients (33%) cleared serum HBsAg during therapy at year 1 (R1 and R7), year 4 (R6) and year 11 (R2). The loss of HBsAg was sustained after stopping therapy in all four patients. All four patients who lost HBsAg subsequently developed anti-HBs, which however was not sustained in one case (R2). The three responders who remained HBsAg positive included one who was lost to follow-up while still on therapy (R4) and two who discontinued peginterferon but remained HDV RNA negative during follow-up of 6 months (R3) and 3.5 years (R5). One of the three subjects who was initially HBeAg positive had HBeAg loss after 1 year of peginterferon, but without development of anti-HBe over the course of the follow-up.
Two patients, both HBeAg positive non-responders, were started on anti-HBV therapy due to active HBV replication before initiation of peginterferon and were maintained on this therapy throughout follow-up. Two responders were started on anti-HBV therapy during peginterferon treatment due to an increase in HBV viral loads at the time of peginterferon discontinuation in one case and during peginterferon therapy in another. Both of these patients were maintained on treatment due to the occurrence of clinical events during follow-up. HBV viral replication was suppressed in all four patients on HBV therapy, as well as in all other patients who did not require therapy but were closely monitored. Only one non-responder had a transient HBV DNA increase at peginterferon discontinuation which did not require therapy and five patients remained with undetectable HBV DNA throughout follow-up.
Management of peginterferon therapy
Five patients were maintained on a constant dose of peginterferon of 180 µg/week, four tolerated an increased dose (up to 270 µg/week), while the remaining three patients required at least one dose reduction. Decrease in peginterferon dose was required within the first year on treatment in one responder due to anaemia, in one non-responder due to cytopenias and in one non-responder due to combined thrombopenia and anaemia. Temporary discontinuation was also required in the latter patient due to sepsis and in one responder due to neutropenic fever; however, re-increase was tolerated afterwards.
All patients were monitored for psychiatric and psychological effects prior and during therapy. Eight patients were evaluated by psychiatry and received pharmaceutical intervention; Five patients received antidepressants at the time of peginterferon initiation, with prophylactic pharmacological therapy in four of them. Out of this group, treatment was discontinued within a year in two cases. A single patient was treated with anti-psychotics and remained stable during the clinical trial but his psychiatric condition led to compliance issues on long-term follow-up. Two patients had antidepressant medications initiated while on therapy at 3 and 4 years into treatment, with eventual discontinuation of antidepressant while remaining on peginterferon in one case.
|
|
| |
| |
|
|
|