 |
 |
 |
| |
US Team Offers Fourth Candidate for Stem Cell Transplant HIV Cure
|
| |
| |
AIDS 2022, July 29-August 2, Montreal
Mark Mascolini
A 66-year-old man treated with stem-cell transplantation for leukemia appears to be the fourth HIV-infected person who maintained HIV control without antiretroviral therapy (ART) for an impressive time after stem-cell transplant [1]. Like previous people “cured” of HIV infection after stem-cell transplantation, this man received stem cells from an individual homozygous for the CCR5delta32 mutation, which can make cells impervious to HIV infection.
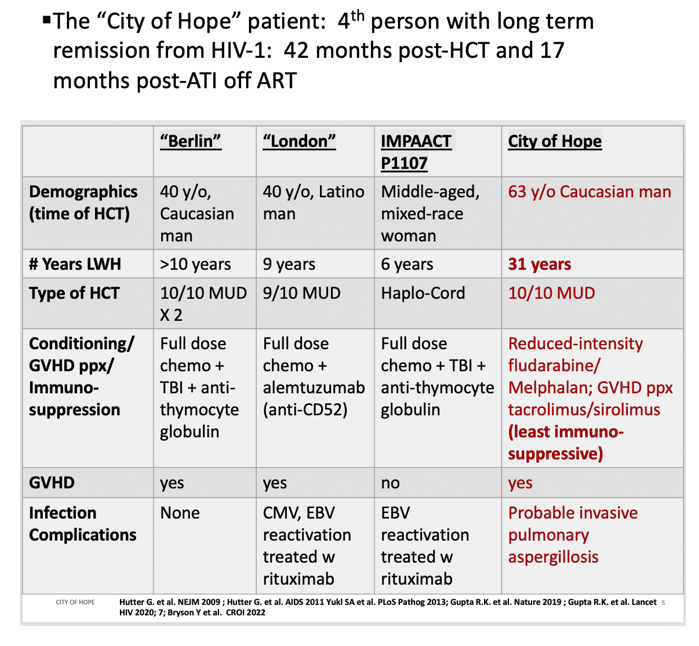
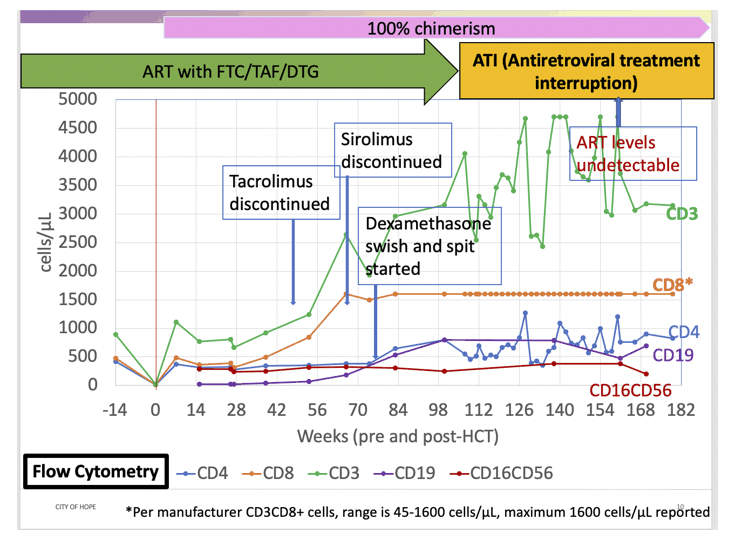
This fourth candidate for HIV cure after stem-cell transplantation received care at the City of Hope Comprehensive Cancer Center outside Los Angeles. At the time of this report, 42 months have passed since his allogeneic hematopoietic stem cell transplantation (alloHCT) and 17 months since he stopped standard three-drug ART.
Now 66 years old, this white man got his HIV diagnosis in 1988. His nadir (lowest-ever) CD4 count stood below 100, but he had no opportunistic infections. From 1997 through 2018, his CD4 count varied between 243 to 1007 and his HIV RNA load remained undetectable for many years. Resistance genotyping in 1999 showed that he had standard mutations conferring high-level resistance to zidovudine and abacavir, intermediate resistance to TDF and TAF, and low-level resistance to emtricitabine (FTC) and lamivudine (3TC). The K103N mutation conferred resistance to first-line nonnucleosides.
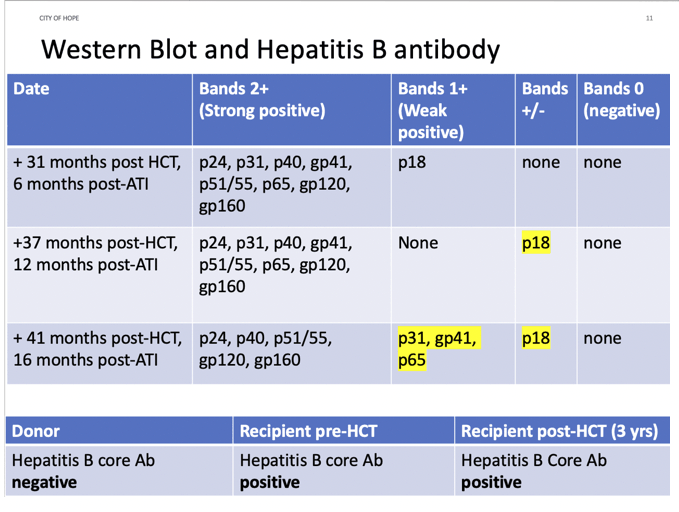
The man’s medical history includes hypertension, hyperlipidemia, anal dysplasia, hypogonadism, central lobular emphysema well-controlled by inhalers, and markers of hepatitis B virus infection. At age 63, the man added a diagnosis of acute myelogenous leukemia to his history, and three courses of chemotherapy led to remission. At that point he changed his ART to FTC, TAF, and dolutegravir to lower risk of drug-drug interactions.
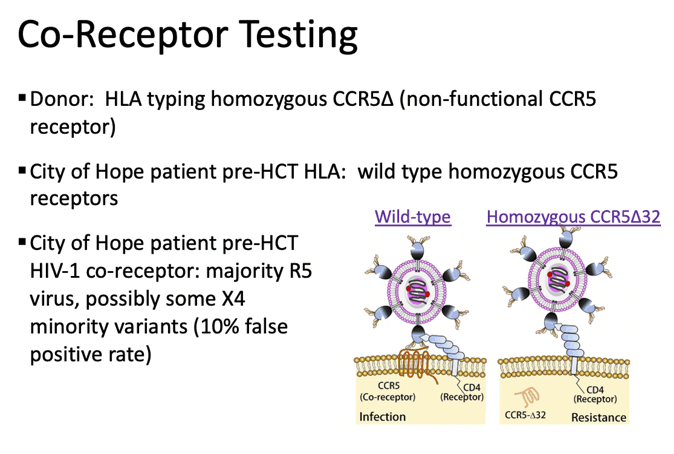
Testing for coreceptors that HIV uses to invade T cells showed that the stem cell donor was homozygous for CCR5delta32, rendering CCR5 receptors nonfunctional. (Homozygosity means inheriting a gene from both mother and father.) Before the stem cell transplant, the City of Hope patient had wild-type (nonmutated) homozygous CCR5 receptors. Most of this man’s HIV isolates used R5 coreceptors, though he may have had some X4 minority variants.
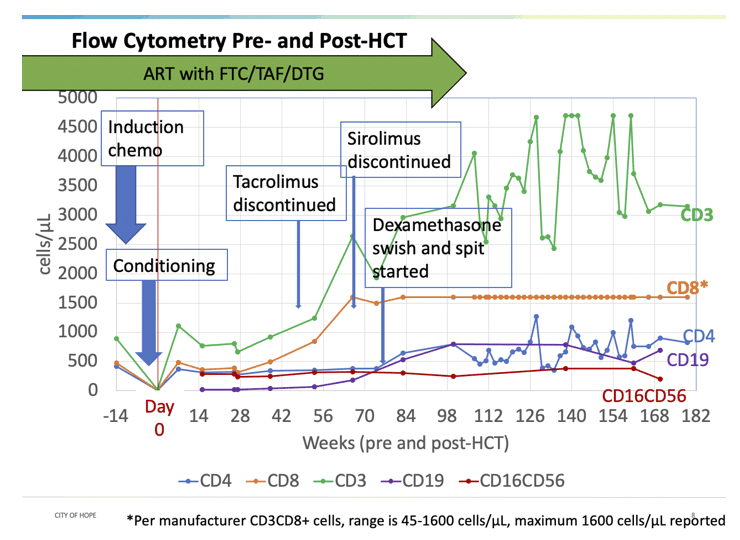
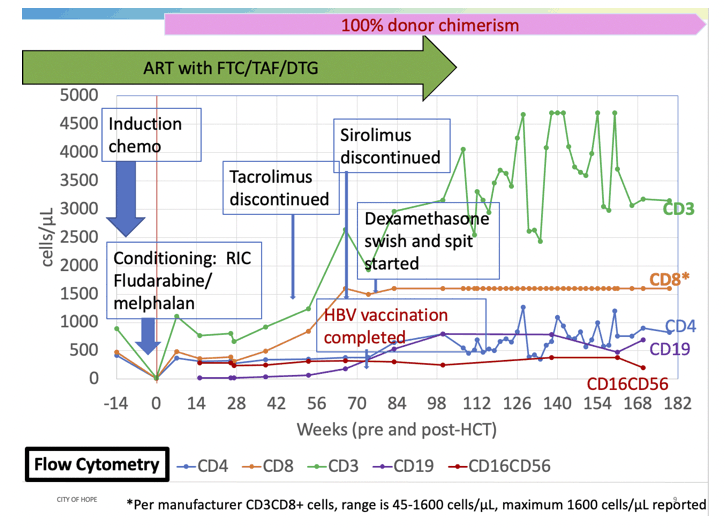
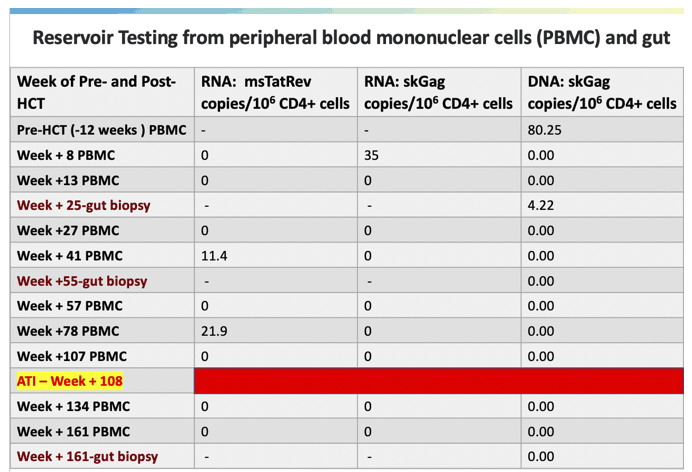
The man continued ART more than 100 weeks after his stem cell transplant then stopped. Antiretroviral levels became undetectable several weeks after he stopped ART. Testing of peripheral blood mononuclear cells (PBMCs) 107 weeks after stem cell transplant showed no trace of HIV RNA per million CD4 cells. These tests for HIV reservoir virus remained negative 134 and 161 weeks after stem cell transplant and in cells collected by gut biopsy.
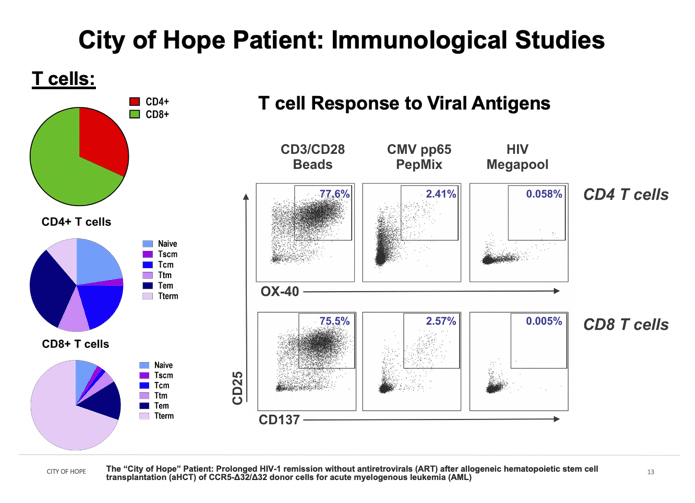
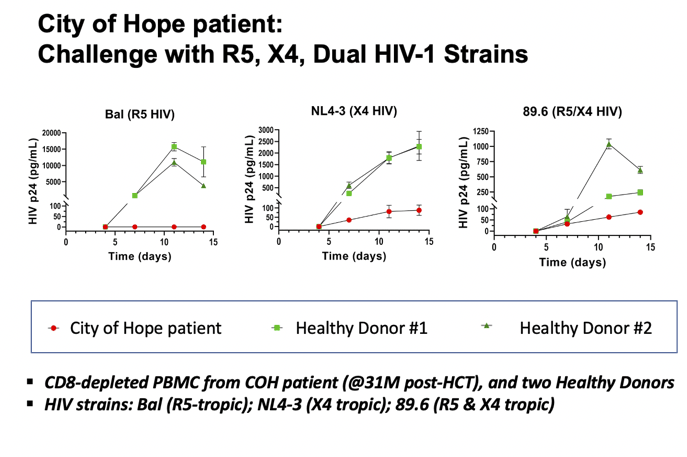
Viral challenge of CD8-depleted PBMCs from this man showed no infection by measuring HIV p24 antigen when the challenge used an R5 lab strain (Bal). But low-level infection was detected after challenge with an X4 strain (NL4-3) or a dual R5/X4 strain (89.6).
The City of Hope team listed some similarities and differences between their patient and the Berlin, London, and IMPAACT P1107 stem-cell transplant patients. The Berlin, London, and IMPAACT individuals were a 40-year-old white man, a 40-year-old Hispanic man, and a middle-aged mixed-race woman, while the City of Hope patient was a 63-year-old white man. For those 4 people, the number of years lived with HIV at transplant were more than 10, 9, 6, and 31. The Berlin, London, and City of Hope men used matched unrelated donors, while the IMPAACT woman used a haplo-cord transplant (donated cord blood stem cells and half-matched [haploidentical] cells from a related donor). The 3 men had graft-versus-host disease after transplant and the woman didn’t. The Berlin patient had no infectious complications; the London man had cytomegalovirus and Epstein-Barr virus (EBV) reactivation treated by rituximab; the IMPAACT woman had EBV reactivation treated with rituximab; the City of Hope man had probable invasive pulmonary aspergillosis.
The world awaits continued follow-up of this stem cell transplant patient and peer review of data collected so far.
Reference
1. Dickter JK, Weibel S, Cardoso A, et al. The 'City of Hope'patient: prolonged in HIV-1 remission without antiretrovirals (ART) after allogeneic hematopoietic stem cell transplantation (alloHCT) of CCR5-delta32/delta32 donor cells for acute myelogenous leukemia (AML). AIDS 2022, July 29-August 2, Montreal. Abstract OALBB0104.





|
| |
|
 |
 |
|
|