 |
 |
 |
| |
NAFLD AND ITS COMBINATION WITH NASH
PREDICT DM DEVELOPMENT IN PEOPLE WITH HIV
|
| |
| |
CROI 2023 Feb 20-23
Win Min Han1, Tanakorn Apornpong1, Jedsadakorn Bonrungsirisap1, Thanathip Wichiangsan1, Hay Mar Su Lwin1, Sivaporn Gatechompol1, Sasiwimol Ubolyam1, Stephen J. Kerr2, Anchalee Avihingsanon1
1Thai Red Cross AIDS Research Center, Bangkok, Thailand, 2Chulalongkorn University, Bangkok, Thailand
program abstract
Background: We investigated the association of non-alcoholic fatty liver disease (NAFLD) plus or minus a concurrent diagnosis of non-alcoholic steato-hepatitis (NASH) with incident diabetes mellitus (DM) among Thai people living with HIV (PLWH).
Methods: This prospective study analysed PLWH aged ≥18 years, on stable stiffness (LS) and controlled attenuated parameter (CAP) values were collected from FibroScan. NAFLD was defined as CAP >248 dB/m, whereas NASH was defined as FibroScan-AST (FAST) score >0.67. Baseline was defined as the first FibroScan date. PLWH with hepatitis B or C virus infection, those with excessive alcohol consumption or with DM diagnosed prior to baseline were excluded. Cox proportional hazard models were used to investigate the association of NAFLD and NASH with incident DM. We also investigated the association of NAFLD with DM at baseline with incident NASH.
Results: Among 847 eligible PLWH, the median age at baseline was 46 (IQR 39-52) years (43% female). Median baseline CD4 was 588 (IQR 443-759) cells/mm3 and 90% had HIV-1 RNA < 50 copies/mL. Median CAP value and FAST score was 215 (IQR 184-254) dB/m and 0.22 (IQR 0.12-0.43) respectively. 28% (235/847) and 15% (116/781) had NAFLD and NASH at baseline, respectively.
During a median follow-up time of 3.3 (IQR 2.7-3.6) years, 28 developed DM (incidence rate=11.0 [95%CI 7.6-15.9] per 1000 person-years).
Baseline NAFLD was associated with an increased risk of incident DM (hazard ratio[HR]: 2.8, 95%CI 1.3-6.4) after adjusting for age, sex, family history of DM, ART duration ART, and didanosine exposure, and time-updated BMI, hypertension and dyslipidemia.
Combined NAFLD and NASH at baseline increased the risk of incident DM (HR: 3.1, 95%CI 1.1-9.3).
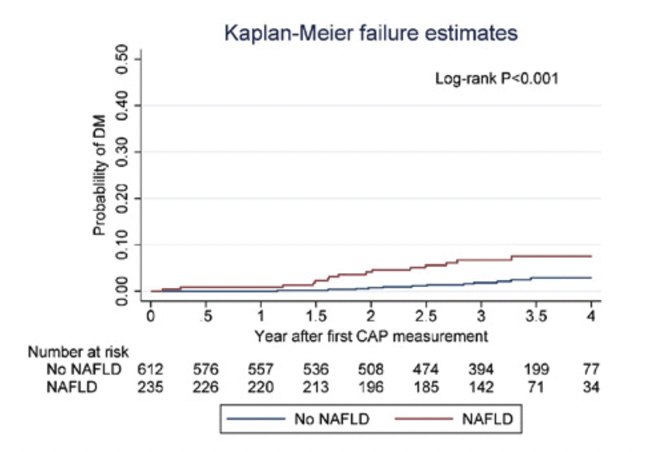
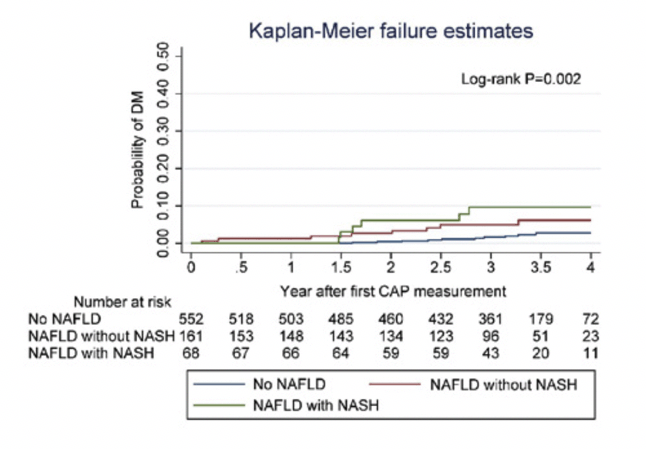
Figure 1A and 1B show the probability of incident DM stratified by NAFLD and NASH status at baseline. Baseline NASH alone showed a non-significant but elevated risk of incident DM (HR:1.8, 0.7-4.4). In a separate analysis including DM at baseline (but excluding NASH at baseline), NAFLD with DM at baseline was associated with incident NASH (HR: 2.5, 95%CI 1.1-6.0).
Conclusion: NAFLD alone or combined with NASH strongly predicts DM development in PLWH, highlighting the need for DM risk assessment and management in PLWH with NAFLD. Further mechanistic studies investigating the underlying metabolic associations of NAFLD or NASH and DM development in PLWH are warranted.
Figure 1A. Probability of DM development by baseline NAFLD status (N=847); Figure 1B. Probability of DM development by baseline NAFLD with NASH status among PLWH with FAST score (N=781)
|
| |
|
 |
 |
|
|