| |
Homeless HCV Treatment-Holistic Care - Patient Centered Required
|
| |
| |
Download the PDF here
Download the PDF here
Download the PDF here
1-Treat The Person, Holistic Care Required for Homeless, IDU
Being able to contact homeless is a barrier to providing sustained successful treatment, as many are not easily reachable may not have cell phones, may share cell phones, may be distracted from treatment. So upon initial contact it is important to identify ways to stay in touch with client: where do they work; who are there friends & their contact info; here do they "hang" out. So attempts tp get in touch can be increased with multiple potential ways to gt in touch.
Developing trust with the client is one of the biggest if not the biggest barrier in successfully treating for HCV. This is a population with extreme mistrust of the "system", of doctors, because IDUS have never been treated humanely, have always been unable to maintain relationships for healthcare, but now that we want to treat them for HCV these barriers become very serious and must be overcome to be successful, so developing a relationship with the client or patient is the most important foundation for building the trust necessary for them to feel they are cared for, accepted & that you the clinician & provider care about them & will help them & provide the needs & support required: housing, food to eat, that you really care, clothing, and more. Jules Levin, NATAP
CDC now recommends one-time hepatitis C testing of all adults (18 years and older). CDC continues to recommend people with risk factors, including people who inject drugs, be tested regularly.
2011 - Hepatitis C virus infection in USA: an estimate of true prevalence - 'estimated 5.2 to 7.1 million HCV+ in USA'
The upper limit of our estimates is 7.1 million total infected persons; hence, the actual number may be much higher than our conservative estimate
2-Homeless definition: U.S. Department of Health and Human Services
A homeless person is defined as an individual
• who lacks housing (without regard to whether the individual is a member of a family), including an individual whose primary residence during the night is a supervised public or private facility (e.g., shelter) that provides temporary living accommodations and an individual who is a resident in transitional housing;
• without permanent housing who may live on the streets; stay in a shelter, mission, single-room occupancy facility, abandoned building or vehicle; or in any other unstable or nonpermanent situation;
• who is "doubled up," a term that refers to a situation where individuals are unable to maintain their housing situation and are forced to stay with a series of friends and/or extended family members.
In addition, previously homeless individuals who are to be released from a prison or a hospital may be considered homeless if they do not have a stable housing situation to which they can return. A recognition of the instability of an individual's living arrangements is critical to the definition of homelessness.
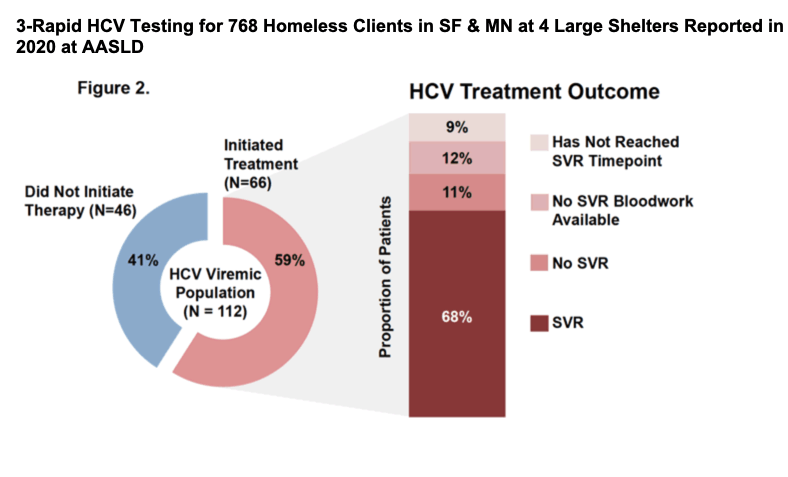
https://www.natap.org/2020/AASLD/AASLD_176.htm
pdf attached
Of the 107 participants with detectable HCV RNA, 66 (61.7%) initiated standard of care HCV treatment (44 in San Francisco and 22 in Minneapolis). The treatment regimens prescribed were as follows: 43 patients (65.2%) received glecaprevir/pibrentasvir, 18 patients (27.3%) sofosbuvir/velpatasvir, 2 patients (3%) elbasvir/grazoprevir, and 1 (1.5%) patient each of sofosbuvir/ledipasvir, sofosbuvir/ledipasvir+ribavirin, and sofosbuvir/velpatasvir/voxilaprevir.
Abstract
Hepatitis C virus (HCV) prevalence is high among people experiencing homelessness, but barriers to scaling up HCV testing and treatment persist. We aimed to implement onsite HCV testing and education and evaluate the effectiveness of low-barrier linkage to HCV therapy among individuals accessing homeless shelters. HCV rapid testing was performed at four large shelters in San Francisco (SF) and Minneapolis (MN). Sociodemographic status, HCV risk, barriers to testing, and interest in therapy were captured. Participants received information about HCV. Those testing positive underwent formal HCV education and onsite therapy. Multivariable modeling assessed predictors of receipt of HCV therapy and sustained virologic response (SVR). A total of 766 clients were tested. Median age was 53.7 years, 68.2% were male participants, 46.3% were Black, 27.5% were White, 13.2% were Hispanic, and 57.7% had high school education or less; 162 (21.1%) were HCV antibody positive, 107 (66.0%) had detectable HCV RNA (82.1% with active drug use, 53.8% history of psychiatric illness), 66 (61.7%) received HCV therapy, and 81.8% achieved SVR. On multivariate analysis, shelter location (MN vs. SF, odds ratio [OR], 0.3; P = 0.01) and having a health care provider (OR, 4.1; P = 0.02) were associated with receipt of therapy. On intention to treat analysis, the only predictor of SVR when adjusted for age, sex, and race was HCV medication adherence (OR, 14.5; P = 0.01). Conclusion: Leveraging existing homeless shelter infrastructure was successful in enhancing HCV testing and treatment uptake. Despite high rates of active substance use, psychiatric illness, and suboptimal adherence, over 80% achieved HCV cure. This highlights the critical importance of integrated models in HCV elimination efforts in people experiencing homelessness that can be applied to other shelter settings.
----------------------
A hepatitis C elimination model in healthcare for the homeless
organization: A novel reflexive laboratory algorithm and equity assessment, Portland, OR 2021
We implemented a streamlined opt-out HCV screening and linkage-to-care program in two healthcare for the homeless clinics and a medically supported withdrawal center.
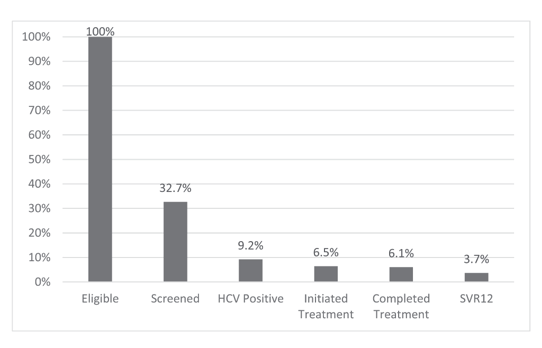
Of 11,035 clients engaged in services between May 2017 and March 2020, 3,607 (32.7%) were screened. Of those screened, 1,020 (28.3%) were HCV PCR positive. Of those with detectable RNA, 712 (69.8%) initiated treatment and 670 (94.1%) completed treatment. Of those initiating treatment, 407 (57.2%) achieved SVR12. There were eight treatment failures and six reinfections.
Nearly half of all patients were experiencing homelessness (33.8%) or in transitional housing (14.0%). Approximately one third had alcohol use disorder (31.7%), opioid use disorder (28.6%), and/or stimulant use disorder (32.4%). Of 11,035 clients engaged in services between May 2017 and March 2020, 3607 (32.7%) were screened.
Pdf attached
------------------------
Development of a Community-based HCV Treatment Completion Intervention Among HCV Positive Homeless Adults, Los Angeles, Oct 2022
This randomized controlled trial (RCT) will test the efficacy of a Community Health Worker/Registered Nurse (CHW-RN) HCV intervention for homeless individuals, many who are also drug users.
The CHW/RN intervention will occur over a 2 or 3 month (8-12 weeks) period depending on the Direct-Acting Antiviral (DAA) prescribed. Homeless adults assigned to the CHW/RN HCV treatment group will receive culturally-sensitive education, case management, and daily DOT delivery of DAA by an RN-guided CHW. The CHW will run a brief (20 min) weekly 1:1 education and 20 min case management session over the 8 or 12 weeks and will deliver all components of the program (which will be developed and refined during Phase I).
Among homeless populations, risk factors for HCV include older age, IDU, needle sharing, previous incarceration, veteran status, fair-or-poor health status, and sharing toothbrushes. Among the 48% of HCV-infected homeless persons who did not inject drugs, correlates of HCV infection include older age, less education, use of drugs, and history of multiple tattoos. While HCV treatment for PWID can reduce HCV prevalence, despite recommended guidelines, only 1-6% of drug-using HCV-infected persons have received treatment.
https://clinicaltrials.gov/ct2/show/NCT04513899
------------------------
Clients' perceptions of barriers and facilitators to implementing hepatitis C virus care in homeless shelters, 2020
We identified key barriers to HCV testing and treatment at the individual level (limited knowledge and misconceptions about HCV infection, mistrust of health care providers, co-morbid conditions of substance use, psychiatric and chronic medical conditions), system level (limited advocacy for HCV services by shelter staff), and social level (stigma of homelessness). Individual, system, and social facilitators to HCV care described by participants included internal motivation, financial incentives, prior experiences with rapid HCV testing, and availability of affordable direct acting antiviral (DAA) treatment, respectively.
https://bmcinfectdis.biomedcentral.com/articles/10.1186/s12879-020-05103-6
------------------------------
Reported in 2004
Correlates of Hepatitis C virus infection in homeless men:
a latent variable approach
Homeless individuals are at risk for numerous health problems including Hepatitis C virus (HCV). HCV is primarily caused by sharing of equipment associated with injection drug use (IDU). In the current study, we assessed differences among HCV-negative and HCV-positive homeless men residing in Los Angeles (N = 198; about 50% HCV positive) on a number of risk factors and behaviors. Findings revealed several significant correlates of HCV-positive status. HCV-positivity was significantly and positively associated with a history of substance use (IDU and non-IDU), recent IDU-related behaviors including equipment sharing, other forms of sharing (e.g., toothbrushes, razors), homelessness severity, tattoos, sexually transmitted diseases, a jail/prison history, and greater age. Lifetime alcohol problems were not associated with HCV. Although associations of HCV with current IDU-related behaviors are not surprising, it is alarming that these behaviors were recent.
Those who work among homeless populations should be aware not only of the high likelihood of HCV infection in this population but also of the
transmission risk due to continued IDU sharing behaviors. Substance abuse treatment should be implemented to hinder the spread of HCV in this vulnerable population. Also, needle exchange and provision of clean ancillary IDU equipment should be encouraged in areas where homeless people are known to congregate.
https://escholarship.org/content/qt0t29f06x/qt0t29f06x_noSplash_10f7c09e400783e72b8cf39f7c59b3ba.pdf
| |
| |
| |
|
|
|