 |
 |
 |
| |
Effect of Obesity on Response to Antiretroviral Therapy in SIV-infected Rhesus Macaques
|
| |
| |
CROI 2024 March 3-6 Denver
Kristin Sauter1, Diana Takahashi1, Melissa Kirigiti1, Sarah R Lindsley1, Hannah Blomenkamp1, Heather Hofmeister, Gabriela Webb2, Oleg Varlamov1, Jonah Sacha2, Charles Roberts1,3, Paul Kievit1
Divisions of 1Metabolic Health & Disease, 2Pathobiology and Immunology, and 3Developmental and Reproductive Sciences, Oregon National Primate Research Center, Oregon Health and Science University Funded by NIDDK R01 DK122843

program abstract
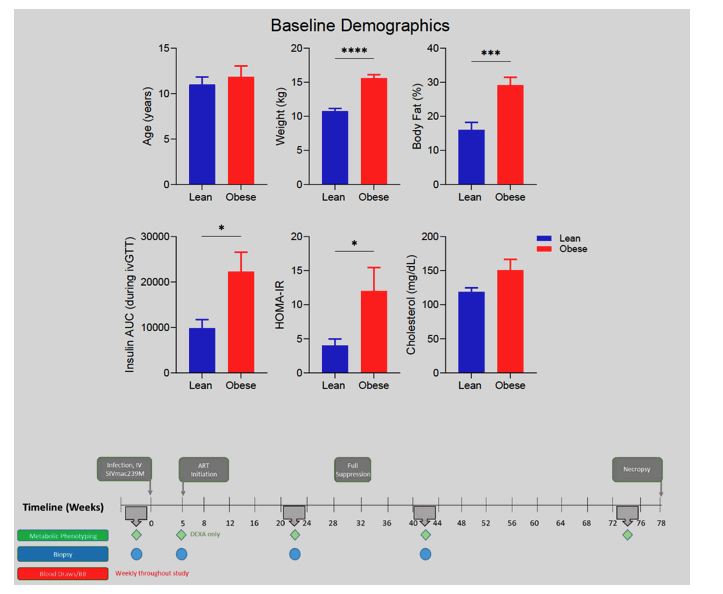
Background: Modern antiretroviral therapy (ART) regimens are associated with increased risk of weight gain and overt metabolic disease. Adipokines play a role in adipose tissue dysfunction and are indicators of cardiometabolic disease risk. A reduced adiponectin:leptin ratio (ALR) is a predictive biomarker that correlates with a number of metabolic risk factors, as well as with markers of chronic inflammation. We employed the rhesus macaque model of SIV infection to determine if a modern ART regimen comprised of TDF, FTC, and DTG would elicit metabolic dysfunction with a corresponding decrease in the ALR, and if this effect was exacerbated by pre-existing obesity.
Methods: Lean, metabolically healthy (n=6) and western-style diet-induced obese (n=5) adult male macaques were infected i.v. with SIVmac239 and ART was initiated at 5 weeks post-infection and continued for 16 months. Baseline and longitudinal assessments of plasma, adipose tissue morphology, and systemic measures of metabolism were obtained.
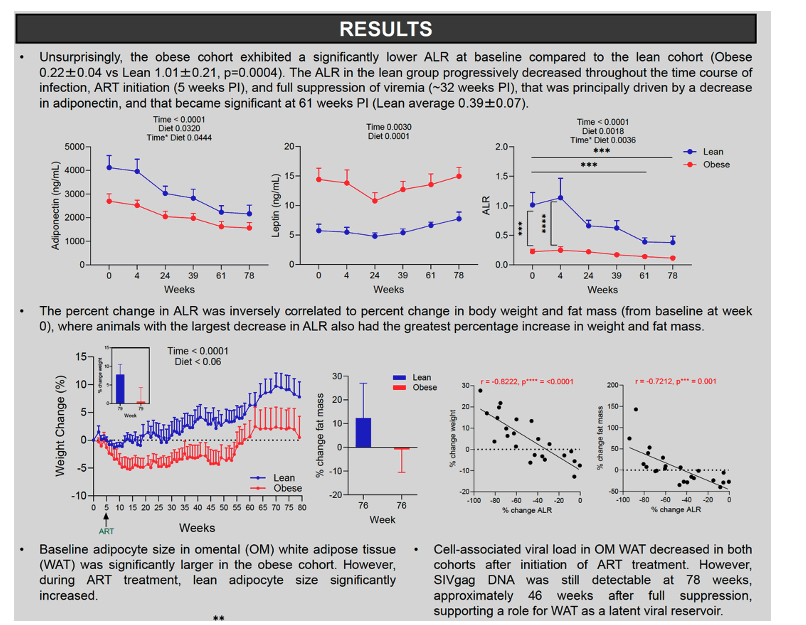
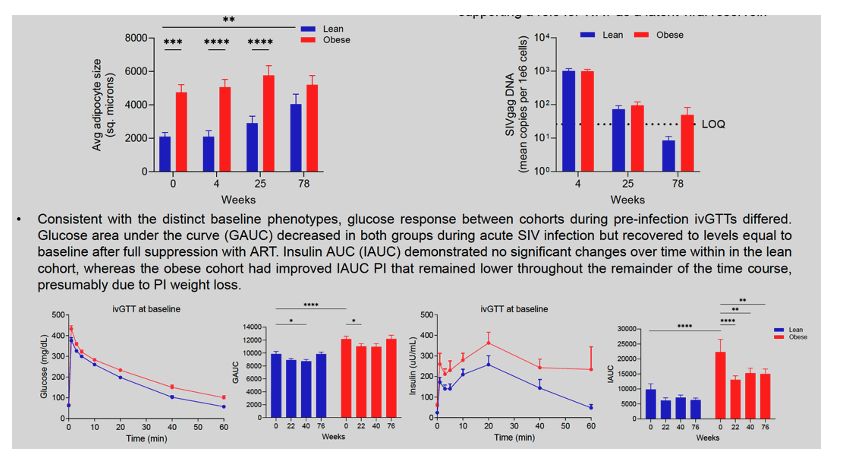
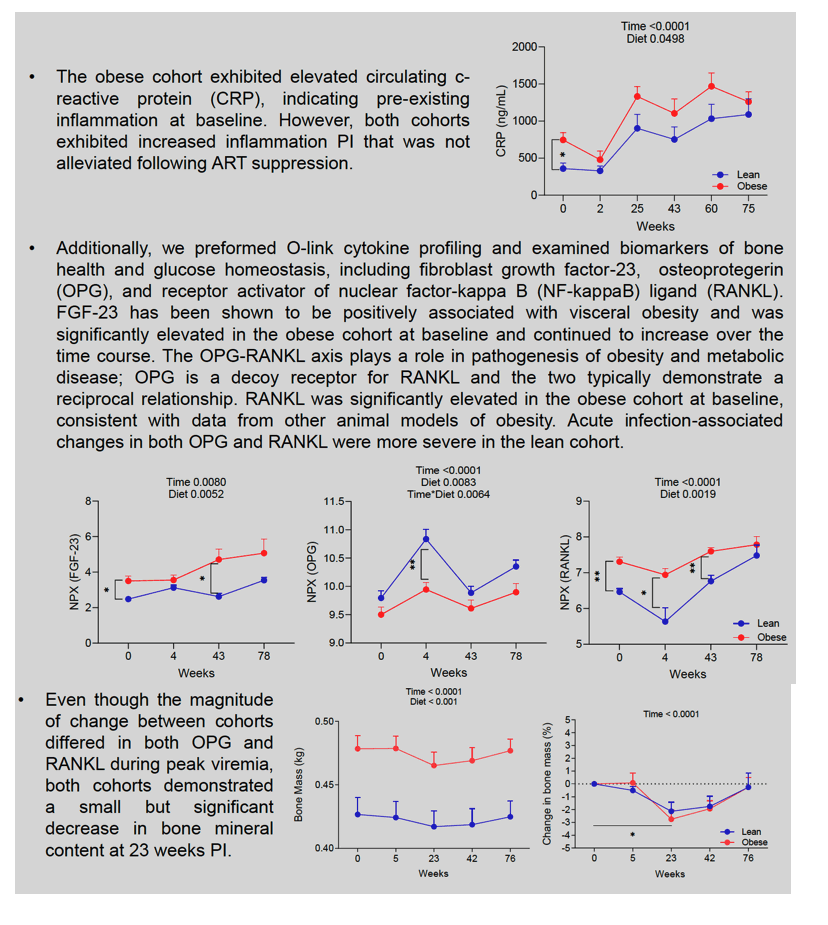
Results: Unsurprisingly, the obese cohort exhibited a significantly lower ALR at baseline compared to the lean cohort (Obese 0.21±0.06 vs Lean 0.87±0.32, p=0.02). The lean cohort experienced a progressive decrease in ALR that was driven by a decrease in adiponectin, throughout the time course of chronic infection, ART initiation, and full suppression of viremia, that became significant at 56 weeks post-infection (PI) (Lean average 0.30±0.05). The change in ALR was inversely correlated to % change in body weight and fat mass, where animals in the lean group with the largest decrease in their ALR also had the greatest weight and fat mass gain. Additionally, the change in ALR in all animals was inversely correlated to % change in fasting insulin levels and HOMA-IR. The obese cohort also exhibited significantly elevated circulating C-reactive protein (CRP) and lipopolysaccharide (LPS)-binding protein (LBP) at baseline compared to the lean cohort. The lean cohort exhibited a drastic increase in both CRP and LBP throughout the time course. The ALR was inversely correlated to CRP levels at necropsy.
Conclusion: SIV infection and subsequent ART significantly decrease the ALR in lean animals to values similar to those seen in pre-diabetic and dysmetabolic obese animals. Thus, SIV and ART induce an obese phenotype in initially lean animals. Therefore, weight gain and/or increases in BMI in people living with HIV are not adequate measures as cardiometabolic risks may be independent of these factors.

|
| |
|
 |
 |
|
|