 |
 |
 |
| |
Phone calls for PrEP persistence in Kenyan
women in postabortal care: a cluster randomized trial.
|
| |
| |
Low PrEP Uptake and Persistence in Kenyan Women, But Phone Program Helps
CROI 2024 (Conference on Retroviruses and Opportunistic Infections), March 3-6, 2024, Denver
Mark Mascolini
Only a small fraction of women at high HIV risk in Kenya-those attending a postabortion clinic-started preexposure prophylaxis (PrEP) in the 6 months after receiving postabortion care and testing negative for HIV [1]. And tiny proportions refilled their PrEP prescription after 1 month. But a phone reminder protocol almost tripled the proportion of women who refilled their PrEP prescription in a cluster-randomized trial.
Renee Heffron (University of Alabama at Birmingham) and colleagues in Africa and the US see three simultaneous epidemics in young women in Kenya-HIV infection, curable sexually transmitted infections, and unintended pregnancy. Among Kenyan women in 2012, 20- to 24-year-olds had an induced abortion rate of about 80 per 1000 women [2]. Because of their recent sexual history, women attending postabortion care clinics may be more open to talking about reproductive health than other women.
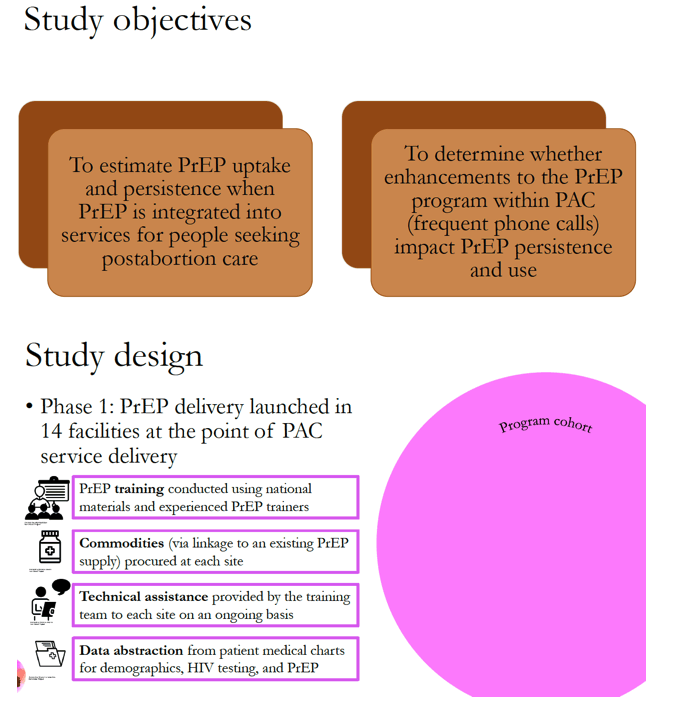
Indeed, research by Heffron and colleagues detected strong PrEP interest among these women as well as risk factors for HIV infection. They conducted this study to estimate PrEP uptake and persistence (continued use) when PrEP is part of postabortion care and to see if a phone-call program could improve PrEP adherence.
The PrEP delivery program began with staff training by experienced PrEP trainers at 14 postabortion care facilities. Researchers gathered data on demographics, HIV testing, and PrEP use in women using these clinics. Within this PrEP delivery rollout, Heffron and coworkers planned a cluster-randomized trial, randomizing clinics to the phone intervention or usual care.
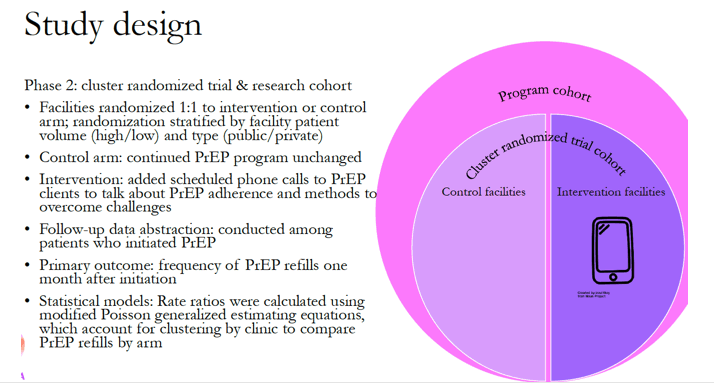
The phone program stipulated PrEP reminder calls 4, 10, 28, and 32 days after a woman started PrEP if she missed a follow-up appointment. After the first month, reminder calls came every 2 weeks, and after 3 months, reminders came monthly. Women attending control clinics got no calls.
The investigators used modified Poisson generalized estimating equations accounting for clustering by clinic to compare PrEP refills in the two study arms. Callers talked to women about PrEP adherence and methods to overcome challenges. The primary outcome was frequency of self-reported PrEP refills 1 month after PrEP began. Women could also have urine tests for presence of tenofovir, indicating recent PrEP use.
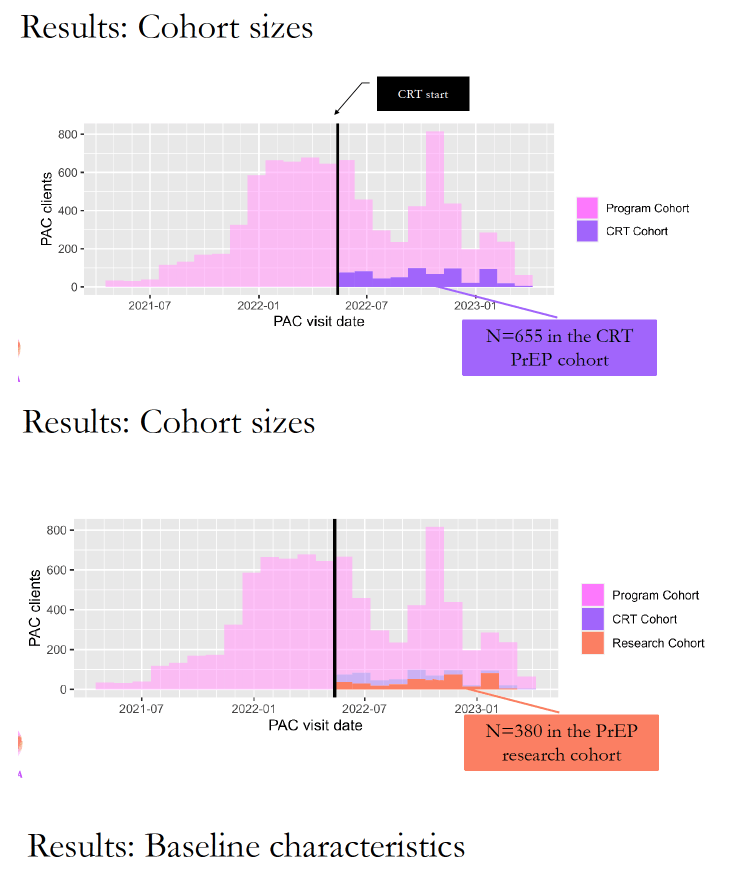
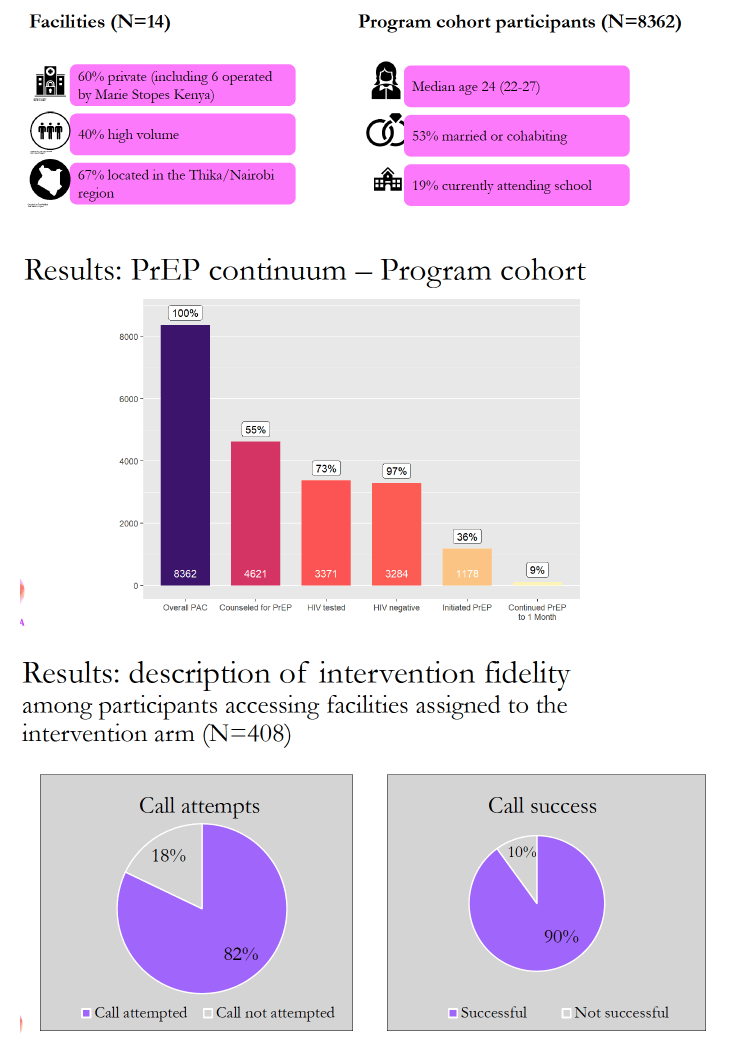
The analysis involved 8362 women attending postabortion clinics from April 2021 to March 2023. Median age of the 8362 women stood at 24 (interquartile range 22 to 27), 53% were married of cohabiting, and 19% currently attended school.
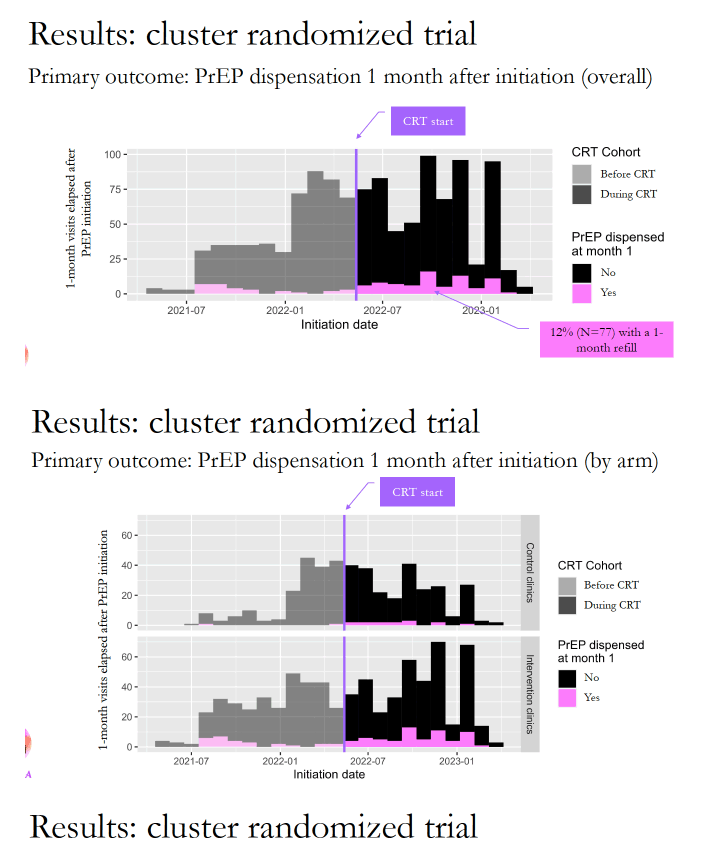
Of the 8362 women, 4621 (55%) got PrEP counseling, of whom 3371 (73%) got tested for HIV. Among tested women, 3284 (97%) tested negative for HIV, and of those 3284 women, 1178 (36%) started PrEP. Only12% of women who started PrEP continued for 1 month-a disturbing outcome especially in women who had the support that comes with a randomized trial and presumably had high motivation to start and continue PrEP because of their sexual history.
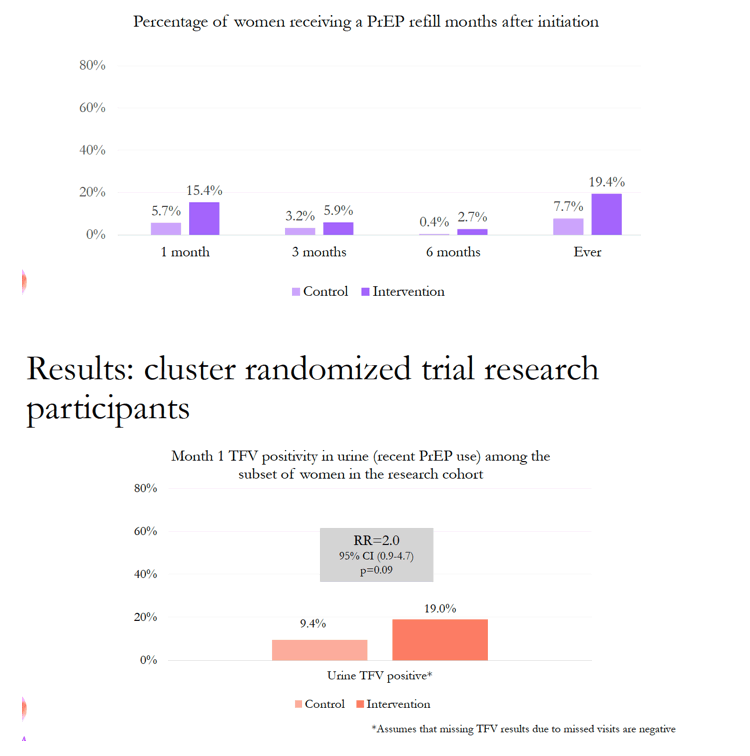
The PrEP research cohort included 380 women. Among women randomized to get reminder calls, calls were attempted for 82%, and callers rated 90% of those calls successful. The call program did improve PrEP refill rates. One month after women started PrEP, 15.4% in the intervention program versus 5.7% in the control group refilled their PrEP prescription. Three months after PrEP began, those proportions were 5.9% versus 3.2%, and after 6 months 2.7% versus 0.4%. Overall, 19.4% of women in the call reminder group versus 7.7% in the no-call group refilled their PrEP prescription.
Poisson generalized estimating equations determined that women in the reminder call program had almost a 3-fold higher chance of refilling their prescription 1 month after starting PrEP (rate ratio [RR] 2.7, 95% confidence interval [CI] 0.9 to 8.2, just short of statistical significance at P = 0.08). Women in the call program had almost a doubled chance of refilling a PrEP prescription at 3 months, but that improvement did not reach statistical significance (RR 1.8, 95% CI 0.4 to 7.9, P = 0.4). Six months after starting PrEP, women getting calls had almost a 7-fold higher chance of refilling their PrEP prescription, a statistically significant difference from the no-call control group (RR 6.7, 95% CI 1.1 to 40.6, P = 0.04). Women getting reminder calls had an overall 2.5-fold greater chance of getting a PrEP refill, but that difference fell short of statistical significance (RR 2.5, 95% CI 0.8 to 7.9, P = 0.12).
One month after starting PrEP, 19.0% of women in the intervention group versus 9.4% in the control group had tenofovir detectable in urine, a result indicating recent PrEP use. But that association stopped a little short of statistical significance (RR 2.0, 95% CI 0.9 to 4.7, P = 0.09).
Heffron and colleagues concluded that the phone-call protocol tested in their cluster randomized trial may improve 1-month PrEP prescription refilling, but numbers of women starting PrEP in this trial were too low to show a statistically significant benefit for the intervention. The researchers believe their findings show that PrEP can be integrated into postabortion care services and so reach women vulnerable to many types of stigma and running a continuing risk of condom-free sex. But that integration "depends on providing foundational PrEP knowledge plus ongoing technical support."
References
1. Heffron R, Etyang L, Nyerere B, et al. Phone calls for PrEP persistence in Kenyan women in postabortal care: a cluster randomized trial. CROI 2024 (Conference on Retroviruses and Opportunistic Infections), March 3-6, 2024, Denver. Abstract 169.
2. Mohamed SF, Izugbara C, Moore AM, et al. The estimated incidence of induced abortion in Kenya: a cross-sectional study. BMC Pregnancy Childbirth. 2015;15:185. doi: 10.1186/s12884-015-0621-1. PMID: 26294220. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4546129/



|
| |
|
 |
 |
|
|