| |
Aging-Related Comorbidity Burden Among Women and Men With or At-Risk for HIV in the US, 2008-2019
|
| |
| |
Download the PDF here
Download the PDF here
Multimorbidity, the presence of 2 or more chronic conditions, represents a growing public health threat.18,19 Multimorbidity prevalence is rising in the US, leading to concerns that its impact on health-related quality of life, health care utilization and costs, and mortality, which is already substantial, may be amplified.20-22 In population studies across varied high-income settings, female sex has emerged as a risk factor for multimorbidity development and progression.
These data highlight the complex interplay of sex and gender, race, and social determinants of health in mediating health outcomes as evidenced by mixed data among PWH regarding the association of race with comorbidity burden.
How psychosocial-biologic pathways may converge to increase multimorbidity risk in PWH, especially for women and people in impoverished communities, is an area of active investigation. Social determinants of health and trauma history have been linked with chronic inflammation via activation of stress responses, which in turn affects comorbidity risk, potentially exacerbated in PWH and women
Conclusions and Relevance In this cross-sectional study, the overall burden of aging-related comorbidities was higher in women vs men, particularly among PWH, and the distribution of comorbidity prevalence differed by sex. Comorbidity screening and prevention strategies tailored by HIV serostatus and sex or gender may be needed.
Meaning Clinical guidance and tools for promoting healthy aging in HIV are urgently needed, and these results suggest that novel strategies developed for comorbidity screening and prevention in persons with HIV would ideally consider sex and gender differences in comorbidity risk and address social determinants of health
Our study supports development of innovative, holistic approaches to promote healthy aging in HIV that prioritize screening and prevention of multimorbidity, integrate assessment of traditional and HIV-related factors, and consider sociobiologic influences of sex and gender. Future studies should also evaluate the optimal timing to commence aging-related comorbidity risk-assessment and intervention, which likely differs by sex and gender, HIV serostatus, and other social determinants of health.
Discussion
Leveraging data from the largest and longest US observational cohort study of persons with and without HIV, we found that among nearly 6000 participants with a median observation of 17 years, the burden of 10 aging-related NACM was higher in women vs men overall and particularly among PWH. The most prevalent NACM were hypertension, psychiatric illness, dyslipidemia, liver disease, and bone disease; and the distribution of prevalent NACM differed by sex. HIV serostatus and age significantly modified the estimated NACM burden by sex, but results were attenuated when adjusting for traditional comorbidity risk factors. Our findings suggest that HIV is associated with sex or gender differences in aging-related comorbidity development, which has important implications for developing and/or refining NACM screening and prevention strategies to promote healthy aging in this population.
Antiretroviral therapy (ART) has dramatically improved the lifespan of persons with HIV (PWH), such that more than 50% of US PWH were aged 50 years or older in 2019.1 For individuals with access to care, despite the gap in overall life expectancy by HIV status narrowing over 2 decades [this study found 9 years reduced survival in their Kaiser study population], the gap in comorbidity-free survival persists: between 2014 and 2016, PWH lived 16.3 fewer healthy years than peers without HIV.2 Aging-related non-AIDS comorbidities (NACM) represent a growing health challenge for PWH, in whom comorbidity burden is higher and onset a decade earlier than the general population.3-6 The downstream impact is immense, including reduced quality of life, premature mortality, and increased health care utilization and cost.7,8
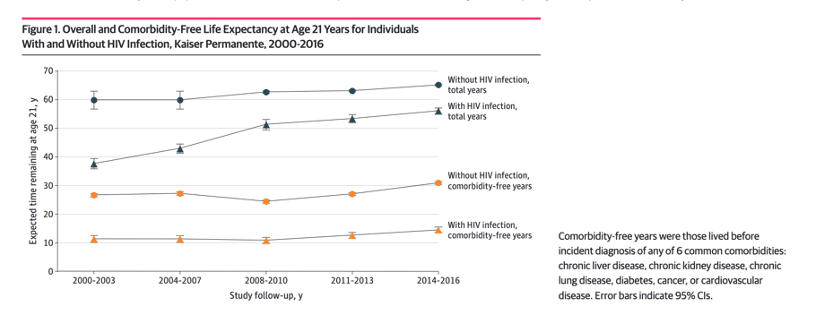
From 2014 to 2016, overall life expectancy at 21 years of age increased to 56.0 years for individuals with HIV infection and to 65.1 years for uninfected adults (difference, 9.1 years; 95% CI, 7.9-10.2 years). From 2011 to 2016, overall life expectancy at 21 years of age for individuals with HIV infection who initiated ART at a CD4 cell count of 500/μL or greater was 57.4 years (95% CI, 55.7-59.1 years) and for uninfected adults was 64.2 years (95% CI, 64.0-64.4 years), corresponding to a difference of 6.8 years (95% CI, 5.0-8.5 years) (Table 3).
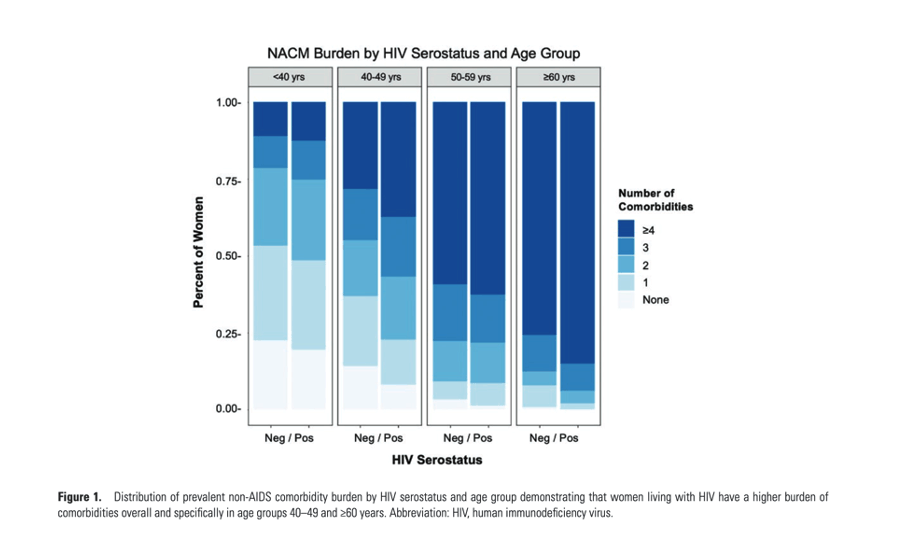
We previously found that women with HIV had a significantly higher prevalent and incident burden of aging-related comorbidities than women without HIV.15,16 Building on these observations, our study combined data from the largest and longest-running observational US cohorts of women and men with and without HIV to assess the association of HIV and comorbidity burden by sex.
|
|
| |
| |
|
|
|