 |
 |
 |
| |
Rise in Heart Disease Risk With Age Slightly Greater With HIV Than in General Population.......[DAD study also shows that reducing risk factors can have a big impact on reducing heart disease]
|
| |
| |
20th Conference on Retroviruses and Opportunistic Infections, March 3-6, 2013, Atlanta
Mark Mascolini
After men with HIV pass age 40, their risk of cardiovascular disease appears to grow somewhat more year by year than it does in three general-population risk equations, according to results of a D:A:D Study analysis [1].
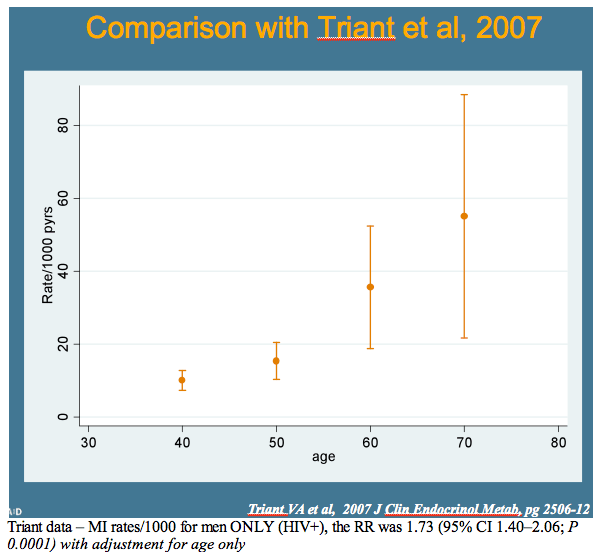
Despite mounting research, how much HIV and age contribute to cardiovascular risk remains difficult to define. A well-planned study published in 2007 found a higher risk of myocardial infarction (MI) in HIV-positive than HIV-negative people--especially women--in a Massachusetts healthcare system, and the risk difference between the two groups widened with age [2].
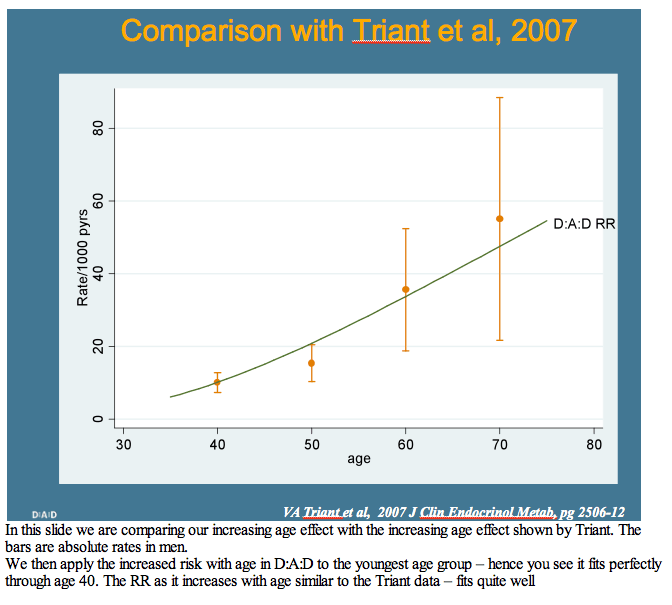
Researchers with D:A:D, the prospective cohort study that assesses adverse event rates and risks in a large HIV-positive group, hypothesized that "if the risk of cardiovascular disease increases faster with age in HIV-positive persons, then we would expect the risk of cardiovascular disease events per year older to be higher in D:A:D relative to the general population."
The analysis focused on D:A:D men without prior cardiovascular disease and with a full set of cardiovascular risk data available, including age, family history of heart disease, smoking, diabetes, total cholesterol, HDL cholesterol, and systolic blood pressure. Endpoints recorded were (1) MI, (2) coronary heart disease (CHD, including MI or an invasive coronary procedure), and (3) cardiovascular disease (CHD or stroke).
The D:A:D team used Poisson regression analysis to fit a number of age effects adjusted for cardiovascular disease risk factors (family history, smoking, cumulative lopinavir and indinavir use, abacavir use within 6 months, diabetes, total cholesterol, HDL cholesterol, and systolic blood pressure). They compared the D:A:D aging effect with three general-population cardiovascular risk equations that have (1) broadly similar endpoints, (2) prospective follow-up, and (3) active ascertainment of endpoints: the Framingham Heart Study, CUORE (an Italian male cohort), and ASSIGN (a Scottish cohort).
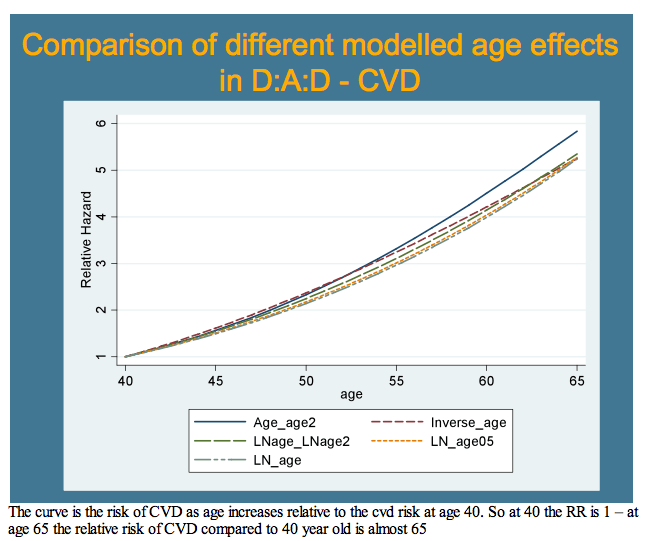
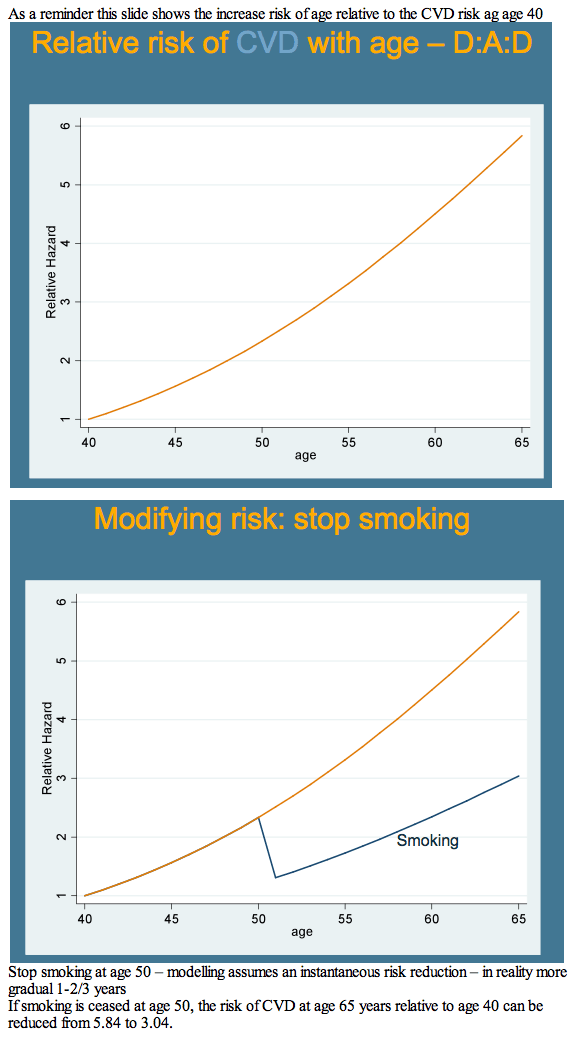
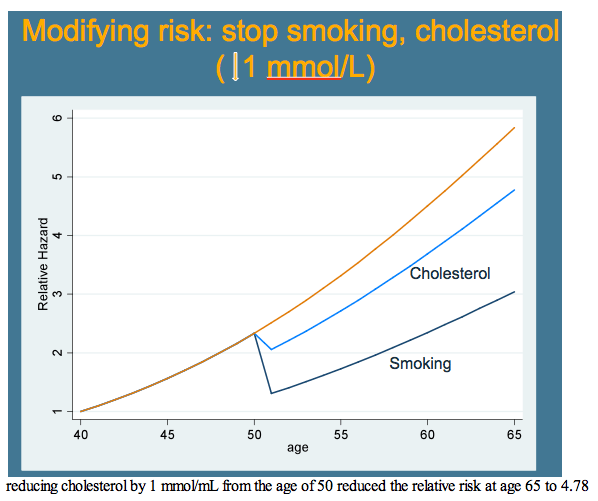
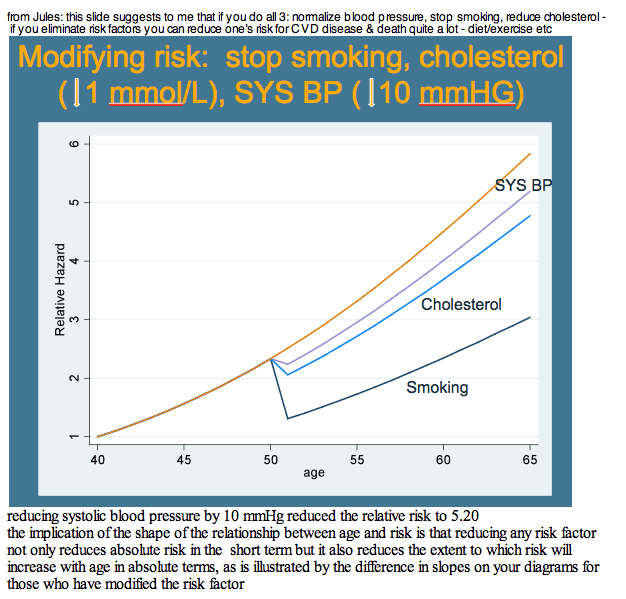
Next the D:A:D team graphically compared relative risk of heart disease from age 40 to age 65, year by year. They could not statistically compare D:A:D to the general population equations, so they determined how risk changed year by year in the other equations with the 95% confidence interval around the change in the D:A:D model. They also modeled risk modification at age 50, separately calculating the impact of stopping smoking, lowering cholesterol by 1 mmol/L (89 mg/dL), and reducing systolic blood pressure by 10 mm Hg.
The analysis included 24,323 D:A:D men through 139,115 person-years of follow-up. During that time there were 474 MIs, 683 cases of CHD, and 884 cases of cardiovascular disease (as defined above). Crude event rates for MI, CHD, and cardiovascular disease were, as expected, higher at age 60 to 65 than at age 40 to 45:
Heart disease incidence at age 40 to 45 versus 60 to 65 in D:A:D men:
-- MI incidence: 2.29 versus 6.53 per 1000 person-years
-- CHD incidence: 3.11 versus 11.91 per 1000 person-years
-- Cardiovascular disease: 3.65 versus 15.89 per 1000 person-years
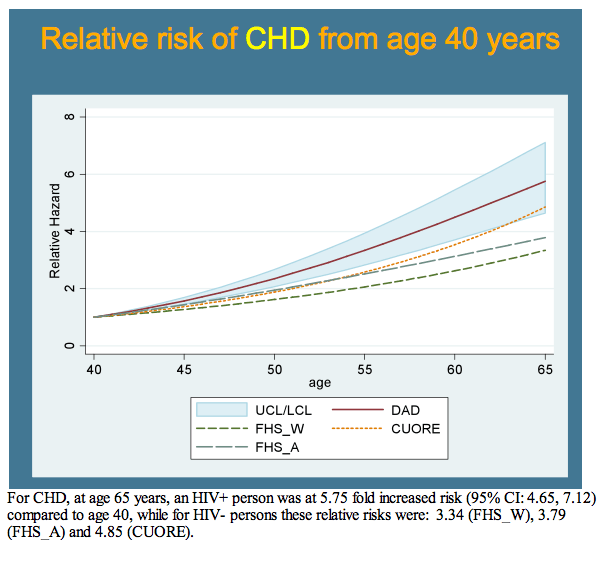
Relative risk of CHD from age 40 through 65 was somewhat greater in D:A:D men than in any of the three general-population risk models--in the sense that the 95% confidence interval around the D:A:D risk curve always lay just above the curves for the other models up age 60. (Because the D:A:D team could not make statistical comparisons, these differences can only be appreciated visually. The slides are online at www.retroconference.org. Click on "View Webcasts and Podcasts," then search for the presenter's name, "Petoumenos.")
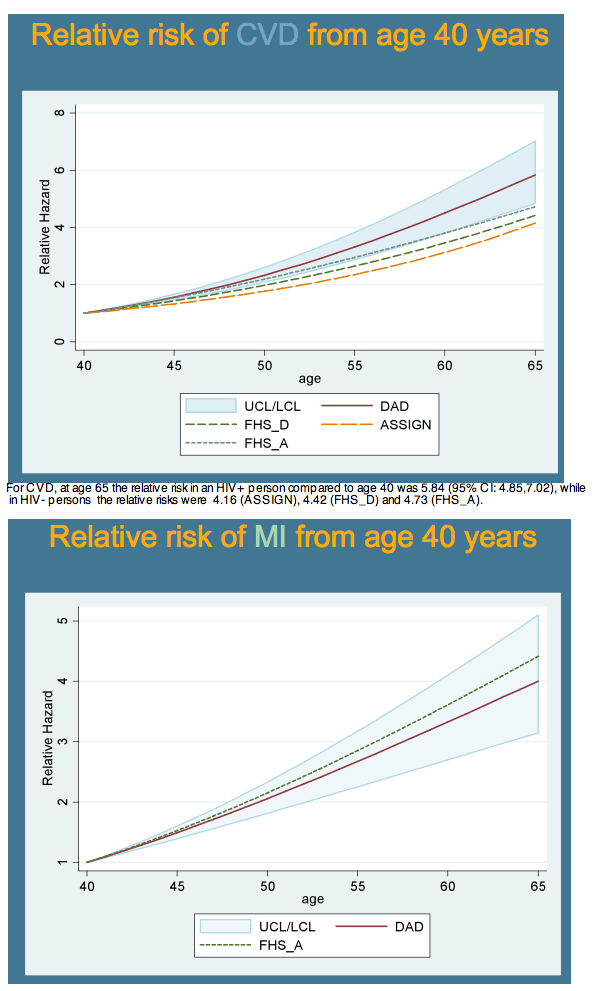
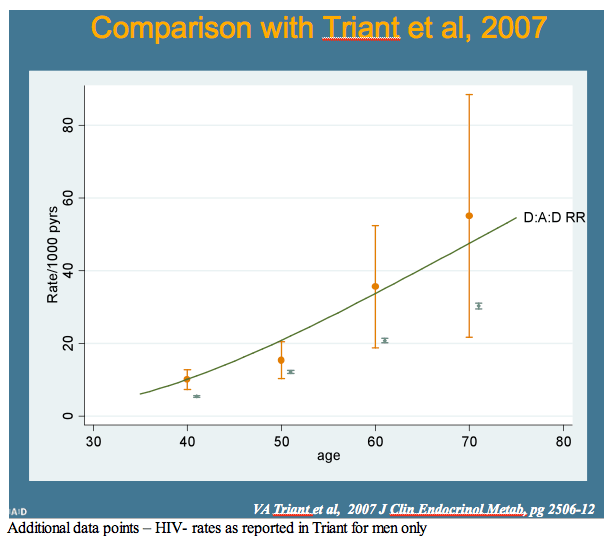
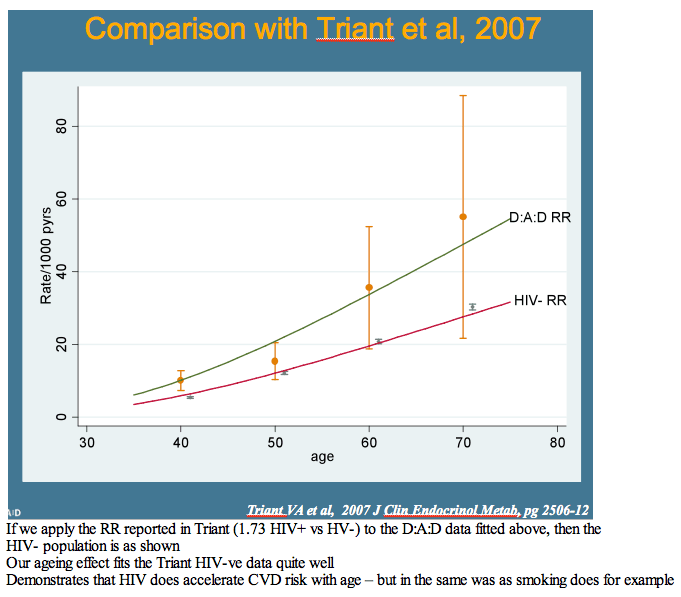
Relative risk of cardiovascular disease in D:A:D also increased slightly faster after age 40 than risk in the other three models. Relative risk of MI with increasing age after 40 years was largely similar in D:A:D and Framingham. These increasing risks with age in D:A:D men fit closely with the age-related risk charted in the Massachusetts study [2]. Of three preventive interventions modeled starting at age 50--stopping smoking, cutting cholesterol by 1 mmol/L, and lowering blood pressure by 10 mm Hg--smoking had the biggest impact.
The researchers concluded that cardiovascular disease risk increases with age in D:A:D, "but only slightly faster" than in general-population risk equations. The investigators believe their analysis "suggests that the additional multiplicative risk of HIV infection is not unlike other risk factors such as smoking." They proposed that cardiovascular risk in people with HIV may be lowered by early intervention (that is, at younger ages) to reduce those risks.
References
1. Petoumenos K, El-Sadr W, d'Arminio Monforte A, et al. Increased risk of cardiovascular disease with age in men: a comparison of D:A:D with HIV- cardiovascular disease risk equations. 20th Conference on Retroviruses and Opportunistic Infections. March 3-6, 2013. Atlanta. Abstract 61.
2. Triant VA, Lee H, Hadigan C, Grinspoon SK. Increased acute myocardial infarction rates and cardiovascular risk factors among patients with human immunodeficiency virus disease. J Clin Endocrinol Metab. 2007;92:2506-2512. https://academic.oup.com/jcem/article/92/7/2506/2598256?login=false
Triant 2007 Study in JCEM:
HIV Infection Appears To Increase Risk Of Heart Attack: doubled risk in HIV+ vs HIV-negative in Mass Gen Hosp study
http://www.natap.org/2007/HIV/042507_02.htm
"In summary, our data from a large cohort of HIV-infected patients demonstrate increased AMI rates and cardiovascular risk factors compared to a non-HIV population, particularly among women. The AMI event rate was approximately two-fold elevated in the HIV cohort, and this difference was seen over multiple age ranges."
The rate of AMI per 1000 person years was higher among HIV patients in this study than in the DAD study, but our study included older patients as well and was from a U.S. population, with potentially different AMI rates and cardiovascular risk factors than the European-based population of the DAD study. Furthermore, the background rate among the entire reference population was similar to that seen in other large U.S. databases, including the Framingham Heart Study, suggesting that this study reliably captured AMI events across the two large hospitals for which we have data. Importantly, the relative risk of AMI in HIV patients was approximately two-fold increased over controls, and thus likely to be clinically significant.
These data suggest that cardiovascular disease will likely become an increasing problem for HIV-infected patients as the population lives longer and ages. Race was also significant in the overall model as an independent predictor of AMI. AMI risk was significantly increased among African-American relative to Caucasians and in Hispanics relative to Caucasians. Among HIV patients, African American race was significant as a predictor of AMI.





|
| |
|
 |
 |
|
|