| |
"HIV infection remained independently associated with a higher number of AANCC (OR 1.58) [age-associated non-communicable comorbidity]" HIV+ had more comorbidities & more than 3, 2 & 1 comorbidities respectively vs HIV-neg....new study published confirming prior studies
|
| |
| |
[new study published today: "Cross-sectional comparison of the prevalence of age-associated comorbidities and their risk factors between HIV-infected and uninfected individuals: the AGEhIV Cohort Study" full text below] - "Short Summary: Age-associated comorbidities (cardiovascular and renal disease) were more prevalent among HIV-positives compared to HIV-negatives. Comorbidity was associated with cardiovascular risk factors, but also with HIV infection, immune deficiency, and (to a lesser extent) systemic inflammation, and prior high-dose ritonavir use.......
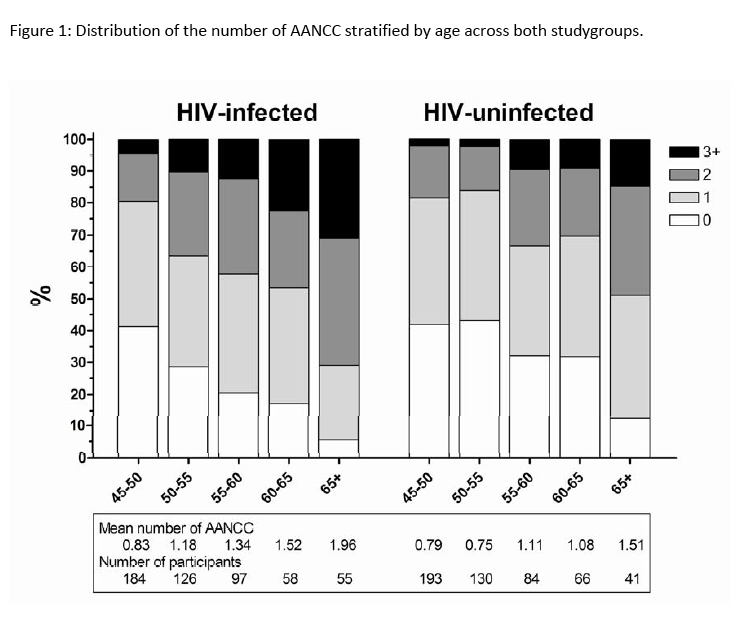
"HIV-positives had a significantly higher mean number of AANCC than HIV-uninfected controls (1.3 (SD 1.14) vs. 1.0 (SD 0.95), p<0.001)......The proportion of participants with ≥1 AANCC was also significantly higher among those with HIV (69.4% vs. 61.8%, p=0.009)......The mean number of AANCC within the 50-55, 60-65, and 65+ age-categories was significantly higher among HIV-infected than HIV-uninfected participants (Figure 1). Furthermore, the distribution of the number of AANCC for HIV-positives in each 5-year age-stratum resembled the distribution for those without HIV who are 5 years older"
"Systolic (135 (IQR 126-147) vs. 133 (IQR 125-143) mmHg, p=0.006) and diastolic blood pressure (81 (IQR 75-89) vs. 79 (IQR 72-85) mmHg, p<0.001) were significantly higher among HIV-positives. Significantly fewer HIV-positives were physically active (44.3% vs. 53.0%, p=0.005) and they had significantly lower levels of 25-OH vitamin D2+D3 (47 (IQR 29-71) vs. 54 (39-72) nmol/L, p<0.001)."
"HIV-infected participants compared to uninfected controls of similar age had a significantly higher prevalence of AANCC, both in terms of composite comorbidity burden, and more specifically of hypertension, cardio- and peripheral vascular disease, and impaired renal function......In multivariable analysis only duration of having CD4-counts <200 cells/mm3 remained an independent risk factor for AANCC.......median levels of each of these biomarkers, except D-dimer, were significantly higher among HIV-positives versus HIV-negatives......Adding hsCRP and sCD14(inflammation/activation) to the above mentioned regression model (analyzing both study groups jointly) showed both markers to be (borderline) significantly associated with AANCC......An above-normal waist-to-hip ratio was an independent risk factor for AANCC, both in the cohorts combined ( OR 1.49 per 0.1 higher ratio, 95% CI 1.23-1.80, p<0.001) and in the HIV-infected (OR 1.35 per 0.1 higher ratio, 95% CI 1.04-1.76, p=0.024) and HIV-uninfected groups separately (OR 1.78.......Our findings thus add robustness to the notion that AANCC indeed are more prevalent among those living with HIV, including in those with a sustained response to antiretroviral treatment.......HIV infection was independently associated with a higher total number of AANCC, as were age, smoking, and positive family history for myocardial infarction, hypertension, diabetes mellitus type 2, or hypercholesterolemia. These traditional risk factors, as well as higher waist-to-hip ratio, independently also contributed to risk of AANCC in each of the studygroups. A borderline significant interaction between age and HIV infection suggested a stronger age-effect among HIV-positives. A longer time spent at a CD4-count<200 cells/mm3 and to a lesser extent more systemic inflammation and innate immune activation, as reflected in higher hsCRP and sCD14 levels, as well as longer prior use of "high-dose" ritonavir (≥400mg/24hrs) were additional factors contributing to AANCC burden........only cumulative duration of high (≥400mg/24hrs) but not of lower doses of ritonavir remained borderline significantly associated with risk of AANCC (OR 1.08 per year "high-dose" ritonavir-use"
Comorbidities and coinfections among HIV patients 50 years and older compared to HIV-negs in large US healthcare database..........http://www.natap.org/2010/AGE/AGE_16.htm
SAME STUDY Published Below Today PRESENTED at 2012 IAC in Wash DC: Comorbidity and ageing with HIV: A prospective comparative cohort study (Dutch study)
http://www.natap.org/2012/IAS/IAS_55.htm
XIX International AIDS Conference, July 26th 2012
the AGEhIV investigators found that similar numbers of cumulative AANCCs (comorbidities) appeared to occur 5 years earlier in HIV-positive people than in HIV-negative people, Average numbers of AANCCs were higher with HIV in every age group
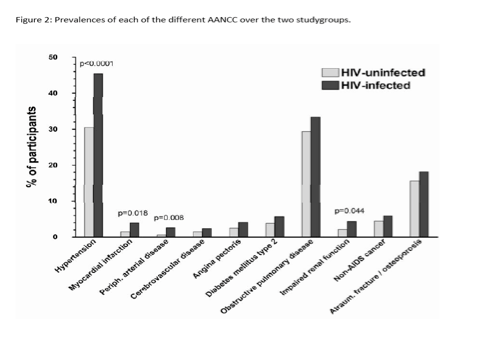
Compared with HIV-negative people, those with HIV had significantly higher rates of eight AANCCs:
-- Hypertension: about 43% versus 30%, P < 0.0001
-- Non-AIDS cancer: about 12% versus 6%, P = 0.001
-- Angina pectoris: about 6% versus 4%, P = 0.005
-- Myocardial infarction: about 5% versus 1%, P = 0.003
-- Peripheral arterial insufficiency: about 4% versus <1%, P = 0.003
-- Chronic liver disease: about 8% versus 1%, P < 0.0001
-- Cerebrovascular disease: about 5% versus 1%, P = 0.022
-- Reduced renal function: about 5% versus 1%, P = 0.006
Italian Study
Premature Age-Related Comorbidities Among HIV-Infected Persons Compared With the General Population
Clinical Infectious Diseases, Giovanni Guaraldi
http://www.natap.org/2011/HIV/102111_01.htm
----------------------------
"HIV infection is associated with inflammation, innate immune activation, and altered coagulation [37-39], which are generally considered important drivers for comorbidity in both HIV-uninfected and HIV-infected individuals[15,16,40,41]. Higher levels of sCD14 and hsCRP, but not of sCD163 or Ddimer, were borderline significantly associated with increased risk for AANCC......We found that although HIV infection status, duration of HIV infection, duration of ART-use, and duration of immune deficiency (i.e. duration of having CD4-counts <200 cells/mm3) were each univariably associated with AANCC, these associations were all confounded by duration of immune deficiency."
"In conclusion, all AANCC were numerically more prevalent, and peripheral arterial, cardiovascular disease, and impaired renal function significantly so, in this cohort of HIV-infected individuals with largely sustained suppressed viremia on cART. Besides cardiovascular risk factors, HIV infection and longer time spent with severe immune deficiency increased the risk of higher AANCC burden. Less pronounced contributions were identified from residual inflammation, immune activation and prior high-dose ritonavir use. The trend towards a stronger association between age and AANCC burden amongst HIV-infected participants might support the hypothesis of premature or accelerated aging in HIV. [8-10]. Whether this reflects HIV acting as an additive risk factor for comorbidity development in conjunction with traditional risk factors, or includes HIV impacting on and accelerating the biology of aging itself, remains to be elucidated.[18,48]."
------------------------
Cross-sectional comparison of the prevalence of age-associated comorbidities and their risk factors between HIV-infected and uninfected individuals: the AGEhIV Cohort Study
Clinical Infectious Diseases Advance Access published September 2, 2014
Download the PDF here
Judith Schouten1,3, Ferdinand W. Wit1,2, Ineke G. Stolte2,4, Neeltje Kootstra5, Marc van der Valk2, Suzanne G. Geerlings2, Maria Prins2,4, Peter Reiss1,2,6, on behalf of the AGEhIV Cohort Study Group
1Academic Medical Center, Dept. of Global Health and Amsterdam Institute for Global Health and Development, Amsterdam, The Netherlands
2Academic Medical Center, Dept. of Internal Medicine, Div. of Infectious Diseases, Center for Infection and Immunity Amsterdam (CINIMA), Amsterdam, The Netherlands
3Academic Medical Center, Dept. of Neurology, Amsterdam, The Netherlands; 4Public Health Service Amsterdam, Infectious Diseases Research, Amsterdam, The Netherlands; 5Academic Medical Center, Dept. of Experimental Immunology, Amsterdam, The Netherlands; 6HIV Monitoring Foundation, Amsterdam
Abstract
Background. HIV-infected individuals may be at increased risk of age-associated non-communicable comorbidity (AANCC).
Methods. Cross-sectional analyses of AANCC prevalence (including cardiovascular, metabolic, pulmonary, renal, bone, and malignant disease) and risk factors in a prospective cohort study of HIV-1-infected individuals and HIV-uninfected controls, aged ≥45 and comparable regarding most lifestyle and demographic factors.
Results. HIV-positives (n=540) had a significantly higher mean number of AANCC than HIV-negatives (n=524) (1.3 (SD 1.14) vs. 1.0 (SD 0.95), p<0.001), with significantly more HIV-positives having ≥1 AANCC (69.4% vs. 61.8%, p=0.009).
Hypertension, myocardial infarction, peripheral arterial disease, and impaired renal function were significantly more prevalent among HIV-positives.
Risk of AANCC by ordinal logistic regression was independently associated with age, smoking, positive family history for cardiovascular/metabolic disease, and higher waist-to-hip ratio, but also with HIV infection (OR 1.58, 95% CI 1.23-2.03, p<0.001). In those with HIV, longer exposure to CD4-counts <200 cells/mm3, and to a lesser extent higher levels of hsCRP and sCD14, and longer prior use of high-dose ritonavir (≥400 mg/24hrs) were each also associated with a higher risk of AANCC.
Conclusions. All AANCC were numerically more prevalent, with peripheral arterial, cardiovascular disease, and impaired renal function significantly so, among HIV-positives compared to HIV-uninfected controls. Besides recognised cardiovascular risk factors, HIV infection and longer time spent with severe immune deficiency increased the risk of a higher composite AANCC burden. There was a less pronounced contribution from residual inflammation, immune activation and prior high-dose ritonavir use.
|
|
| |
| |
|
|
|