| |
Genotype 3 Report - Treatment history, 3 Guidelines (EASL, UK, AASLD/IDSA/IAS), prevalence, after disease progression
|
| |
| |
Reported by Jules Levin
NATAP
Genotype 3 it may surprise you is the 2nd most prevalent in numbers globally after genotype 1 with about 85 million who have GT1 and 43 million who have genotype 3, see linked to report for a breakdown of the epidemiology collected for the numbers in the USA and throughout the world, you will see surprisingly high prevalence reported in India (60-80%), Pakistan (67% with GT3b), in Thailand genotype 3 is dominant with 53% with G3a, in Australia a study reported 31% with GT3 - [http://www.natap.org/2015/HCV/061515_04.htm] lower percentages but still surprisingly high in Western Europe with variability from country to country (for example 47% in UK). In the USA its estimated 12-20%, but clearly we need better data to understand where GT3 is most prevalent, which geographic areas, which patient populations. It has also been said that GT3 appears more common among IDUs, but we need a breakdown to understand among whom with IDU background. It is estimated there are 10 million IDUs globally with HCV (published in 2011by the CDC [http://www.natap.org/2011/newsUpdates/072811_01.htm], in the USA its reported in published paper by the CDC in 2014: Using data from national population-based U.S. surveys, we estimated that persons who ever injected drugs comprised 2.6% (CI: 1.8%-3.3%) of the U.S. population. This represents approximately 6,612,488 million PWID (range: 4,583,188-8,641,788) aged 13 years or older in 2011. Although PWID comprise 3% or less of the U.S. population, they account for 22% of all persons living with HIV infection (http://www.natap.org/2014/HCV/053014_01.htm). Among HIV-infected although its estimated that 30% also have HCV this is misleading because among those infected with HIV by IDU or sexually by men with IDU history the rate of CV-infection is likely to be much higher- an estimated 75-90%. It is widely accepted that HCV GT3 progresses more quickly, it has a more serious potential to progress to advanced disease & to HCC more quickly and more frequently [http://www.natap.org/2015/HCV/061515_07.htm], so one of the key questions is - should GT3 be prioritized for treatment alongside the prioritization for advanced stage F3/F4 disease. Based on the data it appears to me clearly that treatment for patients with GT3 should be prioritized since risk for disease progression is so high, double that compared to Gt1.
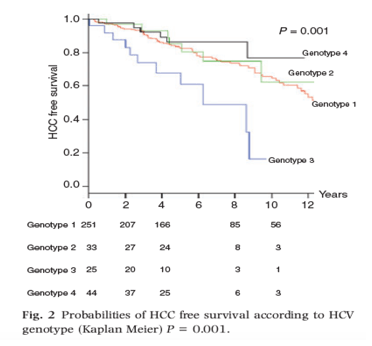
Here are additional reports on GT3 prevalence, treatment & disease progression:
Genotype 3 - prevalence, treatment - (06/30/15)
This is a review of treatments for genotype 3 including Sof/Rbv which was the previously recommended treatment for GT3 in mono and coinfection. There have been a number of studies in previous years reporting Sof/Rbv for GT3 including Phase 2 and Phase 3 studies, these include VALENCE, FISSION, POSITRON, FUSSION, LONESTAR-2. As well, there has been data with Harvoni from ELECTRON-2. These data are included in this review. There is previous data on Peg/Rbv+SOF for GT3 but the latest was reported a EASL 2015, the BOSON Study, at the bottom of this report, which was considered good data results & provided convincing data for the field that this regimen provides good SVR results. Then there is Daclatasvir+Sofosbuvir (with/without Rbv). There have been a number of relevant studies providing data on this regimen either for 12 weeks in naives non-cirrhotics or for cirrhotics and treatment-experienced cirrhotics or non-cirrhotics. There are the ALLY Phase 3 studies, a number of cohort & compassionate use studies all presented at EASL April 2015 in Vienna, these studies are in this report including the French, UK, and BMS cohort studies & compassionate use studies. As well, The Guidelines from 3 groups are in this report. Also included in this report are data from TARGET, a study in the so-called "real-world", data from the TARGET group from a real-world setting, the latest data reported at EASL 2015. In August 2015 the FDA is expected to approve Daclatasvir+Sofosbuvir for genotype 3.
Sofosbuvir in Combination With Pegylated Interferon-alfa and Ribavirin for 12 Weeks Provides High SVR Rates in HCV-Infected Genotype 2 or 3 Treatment-Experienced Patients With and Without Compensated Cirrhosis: Results From the LONESTAR-2 Study.......http://www.natap.org/2014/APASL/APASL_07.htm
Phase 3 Randomized Controlled Trial of All-Oral Treatment With Sofosbuvir + Ribavirin for 12 Weeks Compared to 24 Weeks of PEG + Ribavirin in Treatment-Naïve GT 2/3 HCV-Infected Patients (FISSION).....http://www.natap.org/2013/EASL/EASL_14.htm
---------------------
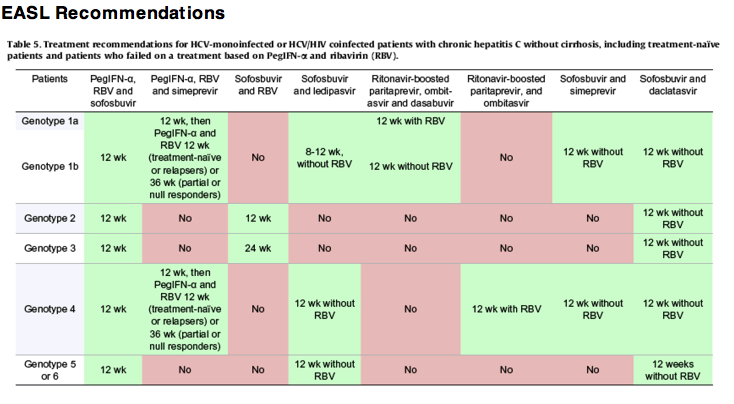
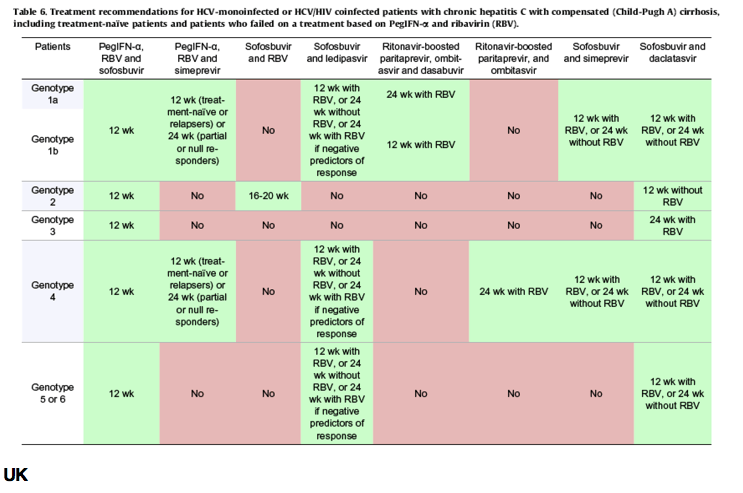
https://www.medicines.org.uk/emc/print-document?documentId=29129
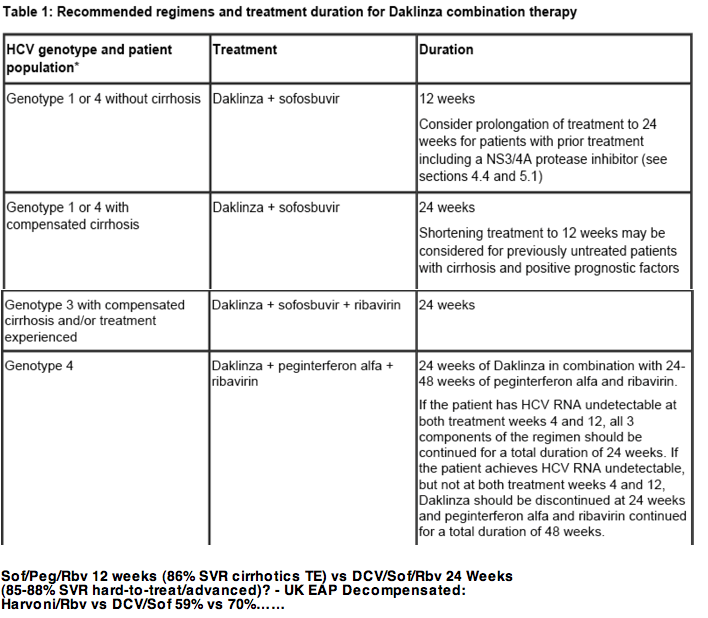
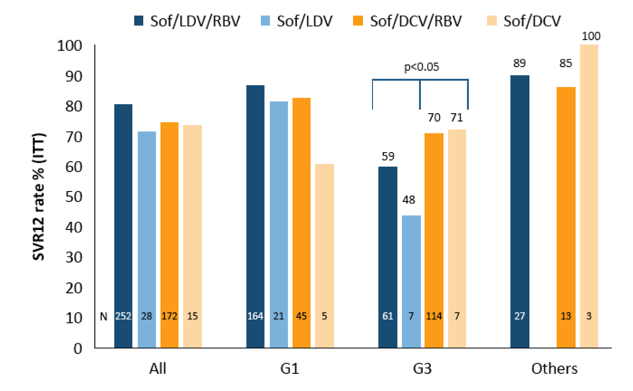
Clinical Pharm of HIV & Hepatitis Population Viral Kinetic Modeling: SVR Prediction in HCV GT-3 Cirrhotic Patients With 24 Weeks of Daclatasvir + Sofosbuvir Administration - (05/29/15)
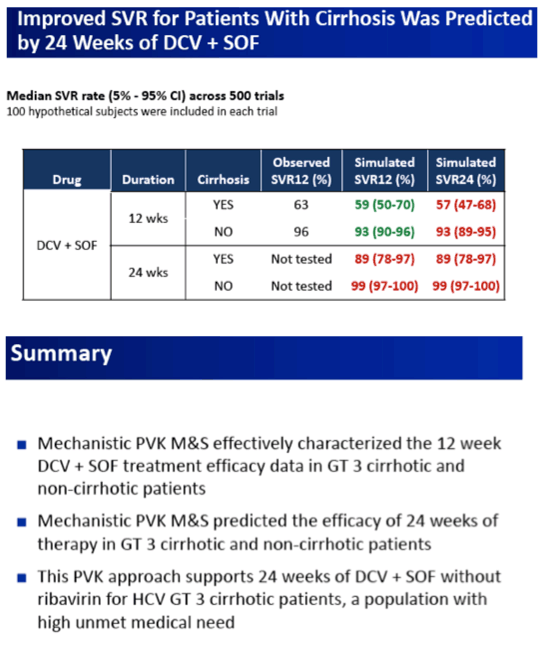
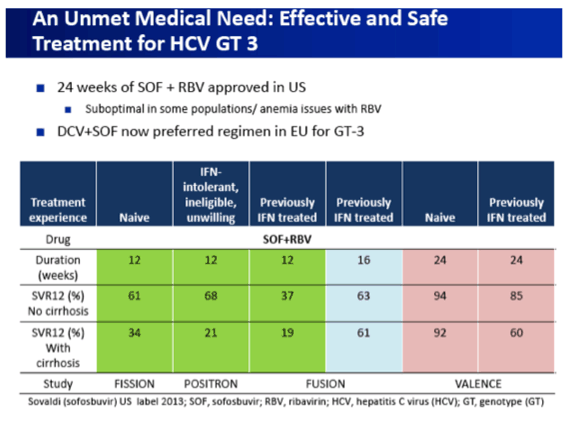
Table 1: Recommended regimens and treatment duration for Daklinza combination therapy SmPC
Due to limitations in the pivotal study many uncertainties remain regarding the most effective way to use Daklinza for
treatment of genotypes 2 and 3 infection, and how to tailor regimens according to important factors potentially
affecting the virological response.
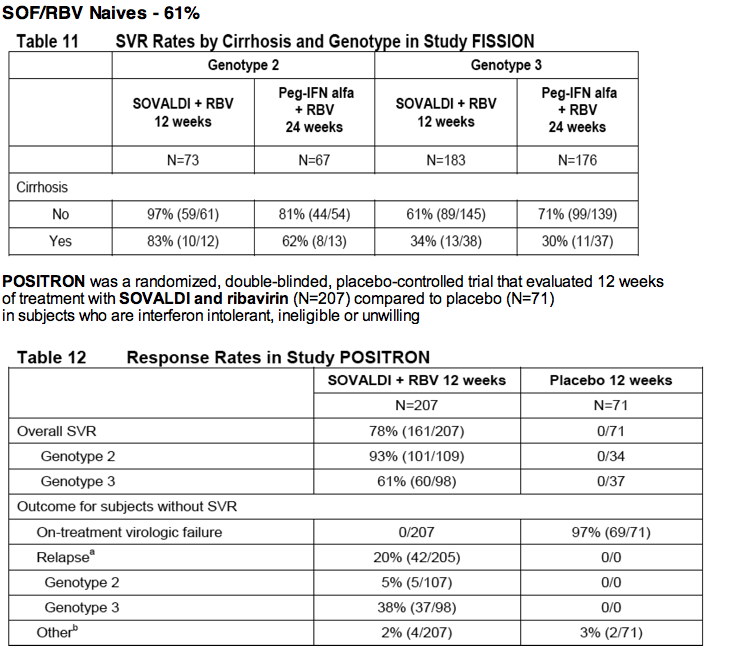
24 Weeks SOF/Rbv
Treatment Experienced Cirrhotics 60% SVR with 24 Weeks SOF/Rbv
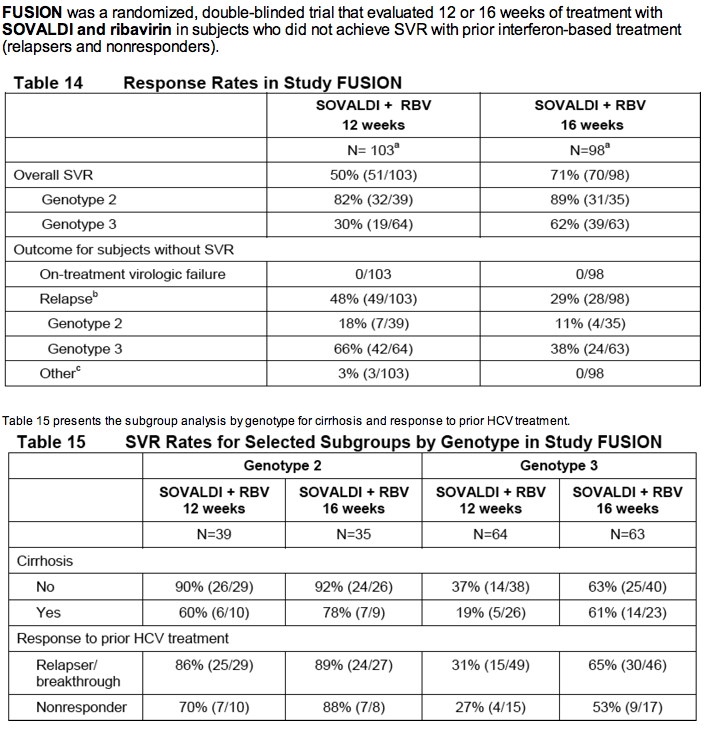
The VALENCE trial evaluated SOVALDI in combination with weight-based ribavirin for the treatment of genotype 2 or 3 HCV infection in treatment-naïve subjects or subjects who did not achieve SVR with prior interferon-based treatment, including subjects with compensated cirrhosis.
Based on emerging data, this trial was unblinded and all genotype 2 HCV-infected subjects continued the original planned treatment and received SOVALDI + ribavirin for 12 weeks, and duration of treatment with SOVALDI + ribavirin in genotype 3 HCV-infected subjects was extended to 24 weeks. Eleven genotype 3 subjects had already completed SOVALDI + ribavirin for 12 weeks at the time of the amendment.
58% of the subjects were treatment-experienced and 65% of those subjects experienced relapse/breakthrough to prior HCV treatment.
Table 16 presents the response rates for the treatment groups of SOVALDI + ribavirin for 12 weeks and 24 weeks.
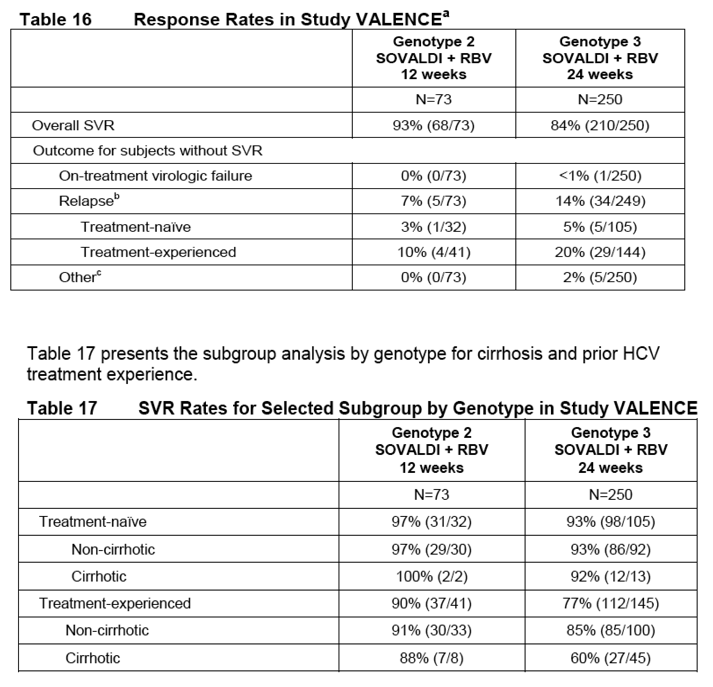
SOVALDI was studied in an open-label clinical trial (Study PHOTON-1) evaluating the safety and efficacy of 12 or 24 weeks of treatment with SOVALDI and ribavirin in subjects with genotype 1, 2 or 3 chronic hepatitis C co-infected with HIV-1. Genotype 2 and 3 subjects were either HCV treatment-naïve or experienced, whereas genotype 1 subjects were all treatment-naïve.


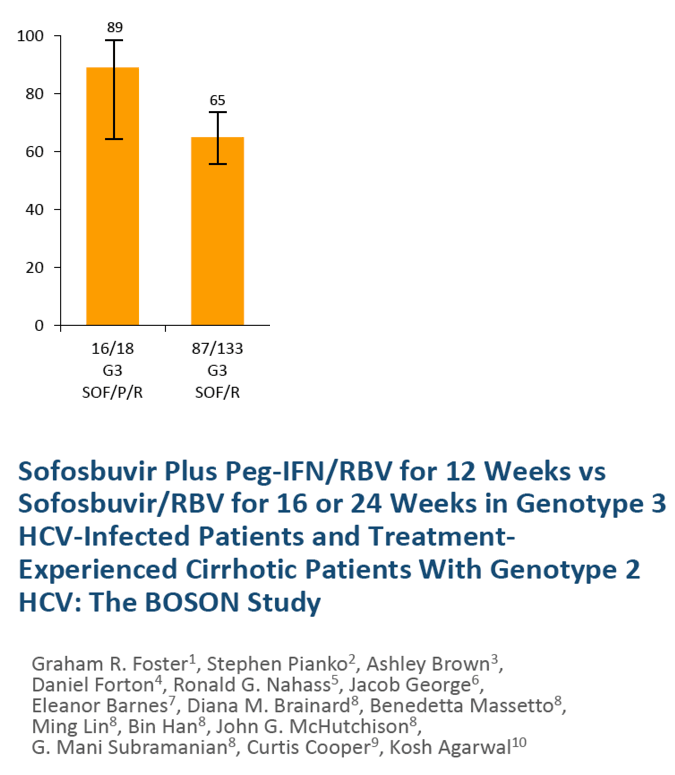
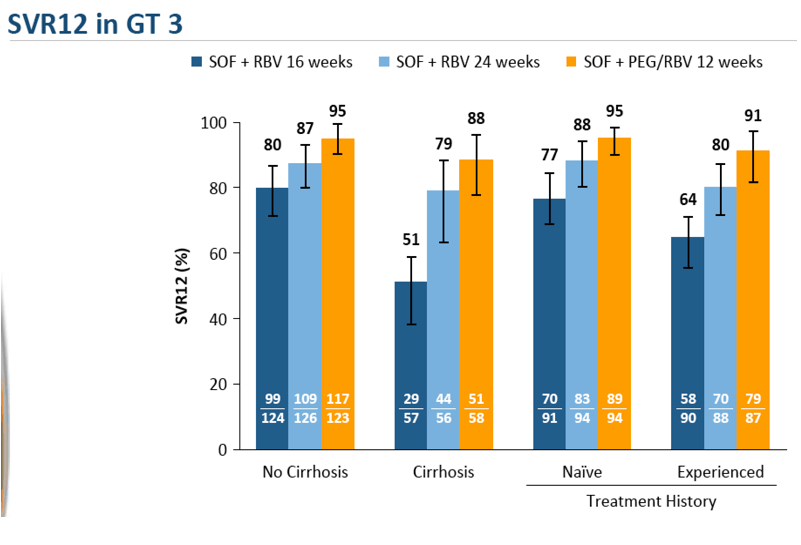
The combination of sofosbuvir plus PEG-IFN and RBV was evaluated in patients with HCV genotype 3
infection. In 2 phase II clinical trials, PROTON and ELECTRON, 38 of 39 (97%) treatment-naive patients
with HCV genotype 3 infection achieved SVR with sofosbuvir plus PEG-IFN (4-12 weeks of therapy) and
RBV. (Gane, 2013b) For many patients with HCV genotype 3 infection, the adverse effects and increased
monitoring requirements of PEG-IFN make this less acceptable than the recommended regimen of
sofosbuvir plus weight-based RBV. However, the shortened treatment period may be of interest to some.
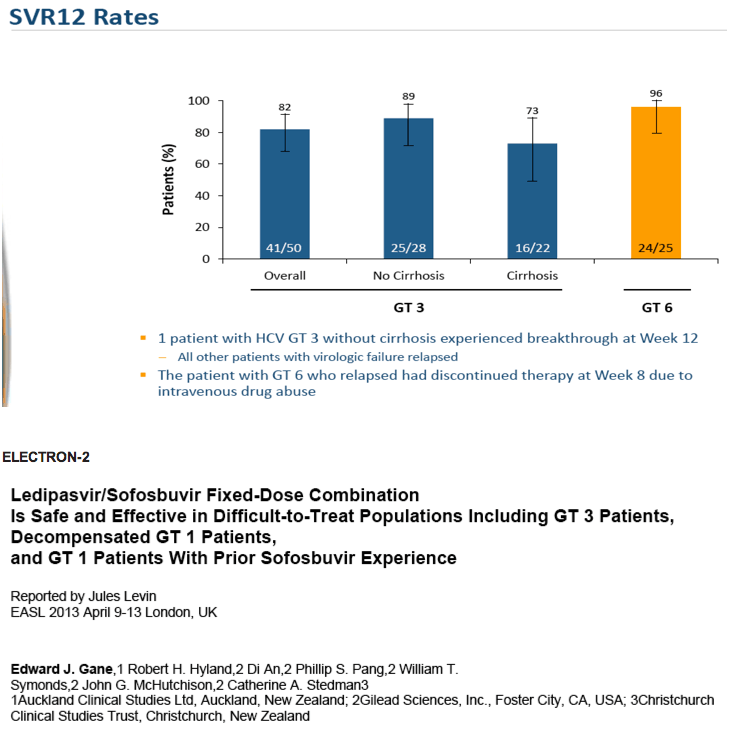
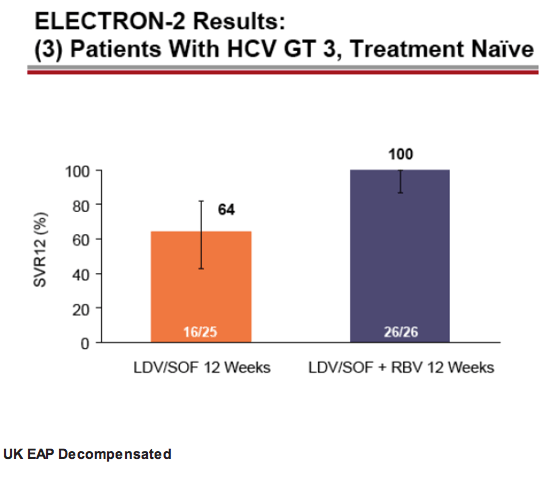
Very limited phase II data are available from a single-center study (ELECTRON-II), which examined
ledipasvir/sofosbuvir with (n=26) or without (n=25) RBV for 12 weeks in treatment-naive patients with HCV
genotype 3 infection, 15% of whom had cirrhosis. All 26 (100%) patients in the RBV-containing arm
achieved SVR12 compared with 16 of 25 (64%) of those in the RBV-free arm. Although these data raise
the possibility that the addition of ledipasvir to sofosbuvir and ribavirin may shorten the course of therapy
for persons with HCV genotype 3 infection, the high EC50 of ledipasvir for HCV genotype 3 (Wong, 2013);
(Kohler, 2014) and the homogenous patient population studied limit the generalizability of this study. Until
further data are available to confirm these findings, a recommendation for use of this regimen cannot be
made at this time. (Gane, 2013b)
FDA PI June 2015
Antiviral Activity
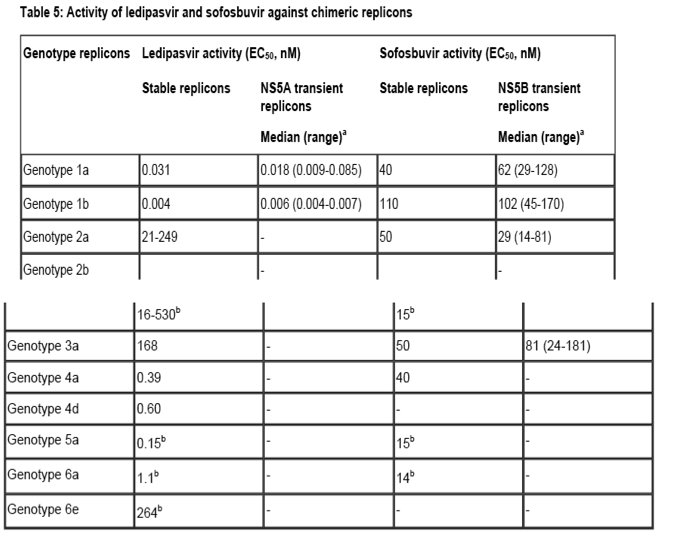
In HCV replicon assays, the EC50 values of ledipasvir against full-length replicons from genotypes 1a and 1b were 0.031 nM and 0.004 nM, respectively. The median EC50 values of ledipasvir against chimeric replicons encoding NS5A sequences from clinical isolates were 0.018 nM for genotype 1a (range 0.009-0.085 nM; N=30) and 0.006 nM for genotype 1b (range 0.004-0.007 nM; N=3). Ledipasvir has less antiviral activity compared to genotype 1 against genotypes 4a, 5a, and 6a, with EC50 values of 0.39 nM, 0.15 nM, and 1.1 nM, respectively. Ledipasvir has substantially lower activity against genotypes 2a, 2b, 3a, and 6e with EC50 values of 21-249 nM, 16-530 nM, 168 nM, and 264 nM, respectively.
In HCV replicon assays, the EC50 values of sofosbuvir against full-length replicons from genotypes 1a, 1b, 2a, 3a, and 4a, and chimeric 1b replicons encoding NS5B from genotypes 2b, 5a, or 6a ranged from 14-110 nM. The median EC50 value of sofosbuvir against chimeric replicons encoding NS5B sequences from clinical isolates was 62 nM for genotype 1a (range 29-128 nM; N=67), 102 nM for genotype 1b (range 45-170 nM; N=29), 29 nM for genotype 2 (range 14-81 nM; N=15), and 81 nM for genotype 3a (range 24-181 nM; N=106). In replication competent virus assays, the EC50 values of sofosbuvir against genotypes 1a and 2a were 30 nM and 20 nM, respectively. Evaluation of sofosbuvir in combination with ledipasvir showed no antagonistic effect in reducing HCV RNA levels in replicon cells.
SMPC
HCV replicons with reduced susceptibility to sofosbuvir have been selected in cell culture for multiple genotypes
including 1b, 2a, 2b, 3a, 4a, 5a and 6a
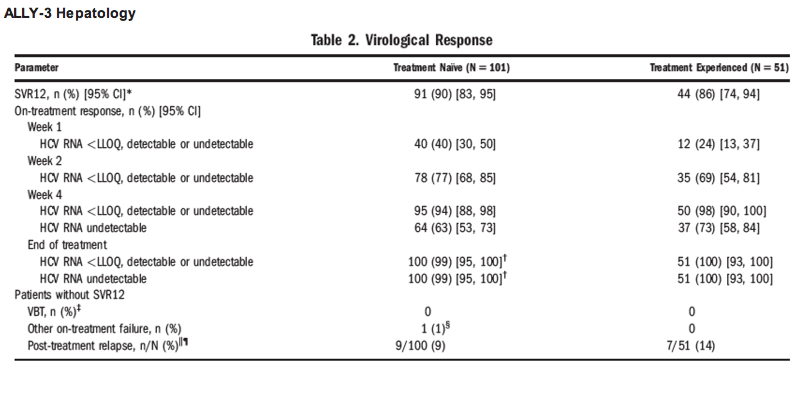
ALLY 3 is a phase III study of the investigational once-daily nonstructual protein 5A (NS5A) inhibitor
daclatasvir (60 mg) plus sofosbuvir (400 mg) for 12 weeks; the study included 101 treatment-naive patients
and demonstrated an SVR12 rate of 90%. In treatment-naive patients without cirrhosis (Metavir F0-F3),
97% achieved SVR12, and in treatment-naive patients with cirrhosis (Metavir F4), 58% achieved
SVR12. (Nelson, 2014) Although approved by regulatory authorities in some regions, daclatasvir is not
available for use in the United States at this time.
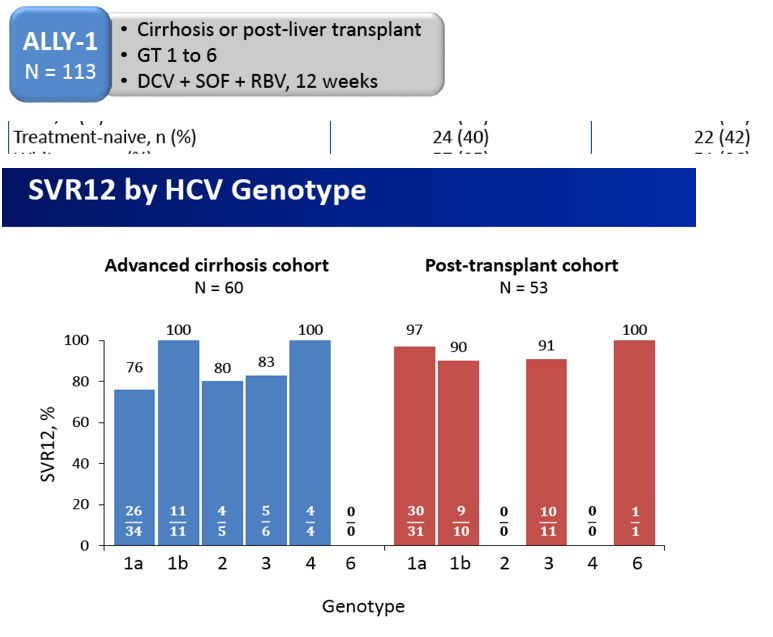
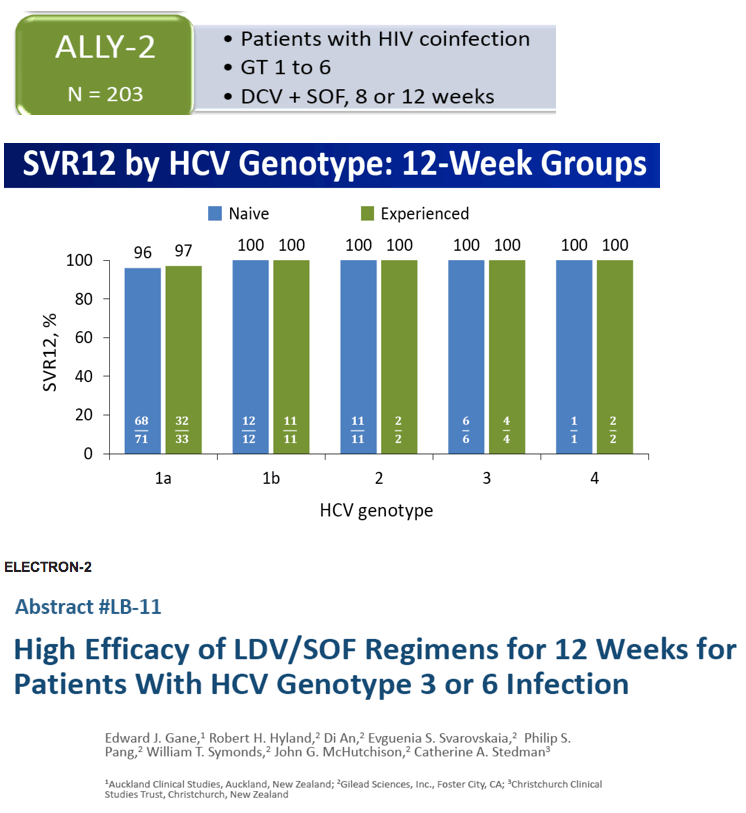
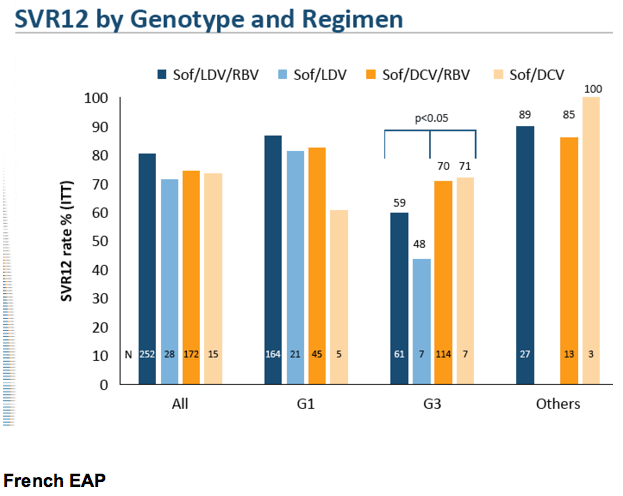
- numbers are small regarding whether use of Rbv makes a difference but that is a question - the SVR results do not distinguish between with or without Rbv. ??
The objective of the French Compassionate Use Program was to provide DCV treatment to patients with no available treatment options
This interim analysis describes the study population and reports the efficacy results for GT 3-infected patients
Advanced liver disease (≥ F3), or
· HCV extra-hepatic manifestations, or
· Post-liver transplant recurrence of HCV infection, or
· An indication for liver or kidney transplant
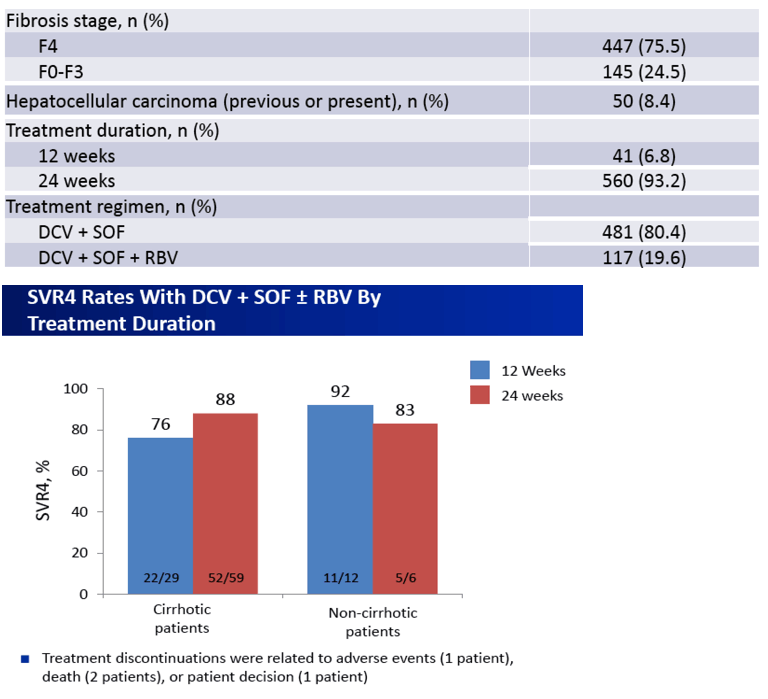
Europe, European Medicines Agency's Committee for Medicinal Products for Human Use (CHMP)6, a compassionate use program (CUP) for the combination DCV + SOF +/-RBV was opened where allowed by local regulations
-This analysis reports interim findings from the European CUP in 5 European countries (Germany, Austria, Netherlands, Sweden and Norway) (AI444-237)
At high risk of hepatic decompensation or death within 12 months if left untreated
-Have no available treatment options
Open-label DCV 60 mg plus SOF 400 mg once daily for 24 weeks
·Dose adjustment for DCV was allowed for patients on concomitant antiretroviral therapy

|
|
| |
| |
|
|
|