Discontinuation of primary Pneumocystis carinii prophylaxis after reconstitution of CD4 cell counts in HIV-infected children
Simon Urschela; Tobias Schusterb; Dominik Dunschb; Uwe Wintergersta; Roland Hofstetterb; Bernd H. Belohradskya
AIDS 2001;15:1589-1591 (Letter)
Pneumocystis carinii pneumonia (PCP) is still one of the most common and most threatening infections in children perinatally infected with HIV. In 1997, the Centers for Disease Control and Prevention found PCP to represent one third of AIDS-defining conditions in children less than 13 years of age. The fact that children suffering from PCP often presented with CD4 cell counts far above the 200 cells/l, which are considered to be the level of immunodeficiency endangering adults, has led to age-related guidelines for primary PCP prophylaxis in HIV-infected children [1]. These guidelines refer to the lowest CD4 cell count ever measured (Nadir count). It is unclear whether the increase in the CD4 cell count under highly active antiretroviral therapy (HAART) also provides a reconstitution of immunological function.
Several studies in adults since 1999 have shown that after an increase of the CD4 cell count above the threshold of 200 cells/l, primary [2-6] and secondary PCP prophylaxis [7,8] can be safely discontinued. This knowledge has led to a change in the recent guidelines for PCP prophylaxis in adults, permitting discontinuation after an increase of the CD4 cell count above 200 cells/l [9]. However, no data are yet available on the situation in children.
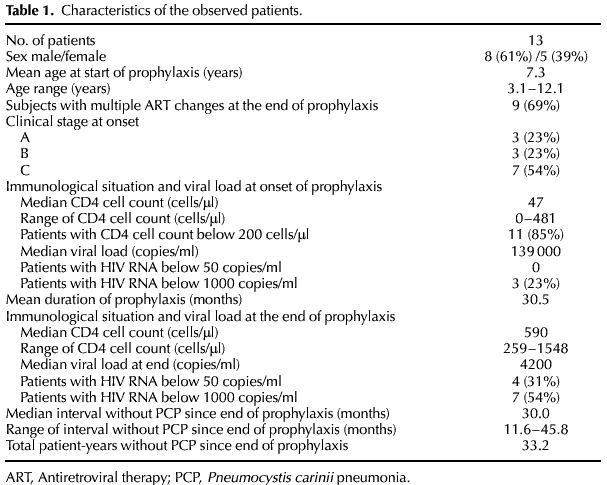
We retrospectively analysed the data of HIV-infected children in two German HIV centres for children (see Table 1); 13 children aged 3.1-12.1 years when primary PCP prophylaxis was begun were included. Eleven received trimethoprim-sulfamethoxazole (150 mg per m2 calculated on trimethoprim, twice a day on 3 days of the week), one received inhalative pentamidine and one dapsone (two times 12.5 mg per day), following international guidelines [1]. If the CD4 cell counts remained above the age-related threshold in at least two controls during 3 months, PCP prophylaxis was discontinued with the consent of the patient's parents or guardian.
All patients received at least triple antiretroviral therapy (ART) when prophylaxis was stopped, which was the primary ART in four of them (31%). The other nine patients (69% had at least two changes in ART in their medical history). At the onset of the PCP prophylaxis none of the patients had HIV-RNA levels below the polymerase chain reaction detection limit (50 copies/ml), at the time of stopping prophylaxis the viral load in four children had decreased below 50 copies/ml and in another three below 1000 copies/ml.
No PCP occurred in the observed interval after stopping prophylaxis, in the mean 30.6 months per patient (range 11.6-45.8 months). Furthermore, no patient developed an AIDS-defining event during the observed 33.2 patient-years.
Furrer et al. [3] used a historical collective of adults as a control group for their patients who discontinued PCP prophylaxis. They found an incidence of 6.1 per 100 patient-years (95% confidence intervals 4.5-8.1) for HIV-infected patients older than 16 years with CD4 cell counts below 200 cells/l in the pre-HAART era. Data collected between 1991 and 1993 showed a risk of 12% of HIV-infected children developing PCP in the first year of life without prophylaxis, independent of the CD4 cell count [9].
A recent study from South Africa in HIV-infected children aged 0-24 months and hospitalized with pneumonia [10] found 15 cases of PCP in 151 children. Only one of these patients belonged to a group of 59 receiving prophylaxis (1.7%), whereas the other 14 (15.2%) affected were part of a group of 92 children without prophylaxis, showing a significantly lower relative risk for children under prophylaxis.
A meta-analysis of more than 50 trials of the Pediatric AIDS Clinical Trials Group in the pre-HAART era [11] defined a PCP incidence of 1.3 per 100 patient-years in children, independent of the CD4 cell count and age. A total of 76% of the patients aged 2-6 years and 97% of the children over 6 years of age had CD4 cell counts below 200/l, indicating that the incidence of PCP in this group, fulfilling the same characteristics as our study group, was much higher. These data suggest a high probability of at least one case of PCP occurring in our collective during the observed 33.2 patient-years after discontinuation of the prophylaxis, if the increase in the CD4 cell count did not correspond to a reconstitution of the immunological function.
Our study is in agreement with the results of the studies on the discontinuation of PCP prophylaxis in adults. It seems to be safe for children beyond the second year of life to discontinue PCP prophylaxis after the CD4 cell count has reliably reconstituted above the age-related critical number under HAART. As a high CD4 cell count does not protect HIV-infected children from PCP during the first year of life, PCP prophylaxis remains essential in these infants. Further studies with larger quantities of patients enrolled need to be performed to verify these results.

REFERENCES
1.Centers for Disease Control and Prevention. Revised guidelines for prophylaxis against Pneumocystis cariniipneumonia for children infected with or perinatally exposed to human immunodeficiency virus. MMWR 1995, 44 (RR-4): 1 -11.
2.Schneider MME, Borleffs JCC, Stolk RP, Jaspers CAJJ, Hoepelman AIM. Discontinuation of prophylaxis for Pneumocystis cariniipneumonia in HIV-1-infected patients treated with highly active antiretroviral therapy. Lancet 1999, 353: 201 -203.
3.Furrer HJ, Egger M, Opravil M. et al. Discontinuation of primary prophylaxis against Pneumocystiscariniipneumonia in HIV-1-infected adults treated with combination antiretroviral therapy. N Engl J Med 1999, 340: 1301 -1306.
4.Weverling GJ, Mocroft A, Ledergerber B. et al. Discontinuation of Pneumocystis cariniipneumonia after start of highly active antiretroviral therapy in HIV-1-infection. Lancet 1999, 353: 1293 -1298.
5.Bienvenido GY, Von Bargen JC, Moormann AC, Holmberg SD. Discontinuation of chemoprophylaxis against Pneumocystis cariniipneumonia in patients with HIV infection. Ann Intern Med 2000, 132: 201 -205.
6.Furrer HJ, Opravil M, Rossi M. et al. Discontinuation of primary prophylaxis in HIV-1-infected patients at high risk of Pneumocystis cariniipneumonia: prospective multicentre study. AIDS 2001, 15: 501 -507.
7.Lopez Bernaldo de Quiros JC, Miro JM, Pena JM. et al. A randomized trial of discontinuation of primary and secondary prophylaxis against Pneumocystis carinii pneumonia after highly active antiretroviral therapy in patients with HIV infection. N Engl J Med 2001, 344: 159 -167.
8.Ledergerber B, Mocroft A, Reiss P. et al. Discontinuation of secondary prophylaxis against Pneumocystis carinii pneumonia in patients with HIV infection who have a response to antiretroviral therapy. N Engl J Med 2001, 344: 168 -174.
9.USPHS/IDSA Prevention of Opportunistic Infections Working Group. 1999 Guidelines for the prevention of opportunistic infections in persons infected with the human immunodeficiency virus. MMWR 1999, 46 (RR-12): 1 -46.
10.Abrams EJ. Opportunistic infections and other clinical manifestations of HIV disease in children. Pediatr Clin North Am 2000, 47: 79 -108.
11.Dankner WM, Lindsey JC, Levin MJ. et al. Correlates of opportunistic infections in children infected with the human immunodeficiency virus managed before highly active antiretroviral therapy. Pediatr Infect Dis J 2001, 20:40 -48.